Abstract
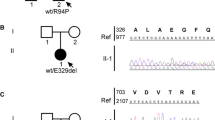
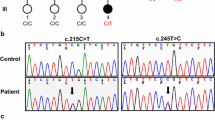
Charcot-Marie-Tooth (CMT) disease represents a distinct subgroup of inherited peripheral neuropathies with a significant prevalence throughout the world and manifests both phenotypic and genetic heterogeneity. Electrophysiological studies subclassify CMT mainly as demyelinating or axonal types. In this study, we investigated the molecular characteristics of a Turkish cohort of 23 probands out of 34 symptomatic demyelinating CMT individuals from January 2019 to December 2021. In order to identify the underlying genetic cause, we applied a rational algorithm: PMP22 gene was initially analyzed for duplication, if PMP22-duplication testing was negative, other most causative genes (GJB1, MPZ) and PMP22 were then sequenced and if no variant was detected at aforementioned tests, whole exome sequencing (WES) test was finally performed. A total of 17 patients (≅ 74%; n = 23) were found to harbor a disease-causing variant in demyelinating CMT-related genes and among the variants, PMP22-duplication was the most frequent (≅ 41%). CMT1, CMTX, and CMT4 subtypes were manifested in ten, five, and two individuals respectively. GJB1 and SBF2 genes were the only detected genes associated with the CMTs other than CMT1. We also reported totally five novel variants: c.379A > C (p.Ile127Leu) and c.548G > T (p.Arg183Leu) variants in GJB1, c.988G > T (p.Glu330Ter) variant in NEFL, c.765_770delCCCTAT (p.Pro256_Ile257del) and c.2552A > C (p.His851Pro) variants in SBF2. As the understanding of pathophysiology and molecular mechanisms of CMT continues to evolve rapidly, many therapeutic strategy options including promising small-molecular compounds, gene replacement therapy, or disease-modifying therapies will soon be implemented in the clinical setting.


Similar content being viewed by others
References
Laurá M, Pipis M, Rossor AM, Reilly MM (2019) Charcot-Marie-Tooth disease and related disorders: an evolving landscape. Curr Opin Neurol 32(5):641–650. https://doi.org/10.1097/WCO.0000000000000735
Stojkovic T (2016) Hereditary neuropathies: an update. Rev Neurol (Paris) 172(12):775–778. https://doi.org/10.1016/j.neurol.2016.06.007
Dyck PJ, Lambert EH. Lower motor and primary sensory neuron diseases with peroneal muscular atrophy. I. Neurologic, genetic and electrophysiologic findings in hereditary polyneuropathies. Arch Neurol 1968;18(6):603–618, https://doi.org/10.1001/archneur.1968.00470360025002.
Dyck PJ (1975) Inherited neuronal degeneration and atrophy affecting peripheral motor, sensory, and autonomic neurons. In: Dyck PJ, Thomas PK, Lambert EH (eds) Peripheral neuropathy, 1st edn. W. B. Saunders, Philadelphia, pp 825–867
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of medical genetics and genomics and the association for molecular pathology. Genet Med 17(5):405–424. https://doi.org/10.1038/gim.2015.30
Lupski JR, de Oca-Luna RM, Slaugenhaupt S, Pentao L, Guzzetta V, Trask BJ et al (1991) DNA duplication associated with Charcot-Marie-Tooth disease type 1A. Cell 66(2):219–232. https://doi.org/10.1016/0092-8674(91)90613-4
Roa BB, Dyck PJ, Marks HG, Chance PF, Lupski JR (1993) Dejerine-Sottas syndrome associated with point mutation in the peripheral myelin protein 22 (PMP22) gene. Nat Genet 5(3):269–273. https://doi.org/10.1038/ng1193-269
Hayasaka K, Ohnishi A, Takada G, Fukushima Y, Murai Y (1993) Mutation of the myelin P0 gene in Charcot-Marie-tooth neuropathy type 1. Biochem Biophys Res Commun 194(3):1317–1322. https://doi.org/10.1006/bbrc.1993.1968
Bergoffen J, Scherer SS, Wang S, Scott MO, Bone LJ, Paul DL et al (1993) Connexin mutations in X-linked Charcot-Marie-Tooth disease. Science 262(5142):2039–2042. https://doi.org/10.1126/science.8266101
Saporta AS, Sottile SL, Miller LJ, Feely SM, Siskind CE, Shy ME (2011) Charcot-Marie-Tooth disease subtypes and genetic testing strategies. Ann Neurol 69(1):22–33. https://doi.org/10.1002/ana.22166
DiVincenzo C, Elzinga CD, Medeiros AC, Karbassi I, Jones JR, Ewans MC et al (2014) The allelic spectrum of Charcot–Marie–Tooth disease in over 17,000 individuals with neuropathy. Mol Genet Genomic Med 2(6):522–529. https://doi.org/10.1002/mgg3.106
Fridman V, Bundy B, Reilly MM, Pareyson D, Bacon C, Burns J, Day J et al (2015) CMT subtypes and disease burden in patients enrolled in the Inherited Neuropathies Consortium natural history study: a cross-sectional analysis. J Neurol Neurosurg Psychiatry 86(8):873–878. https://doi.org/10.1136/jnnp-2014-308826
Murphy SM, Laura M, Fawcett K, Pandraud A, Liu YT, Davidson GL et al (2012) Charcot–Marie–Tooth disease: frequency of genetic subtypes and guidelines for genetic testing. J Neurol Neurosurg Psychiatry 83(7):706–710. https://doi.org/10.1136/jnnp-2012-302451
Sivera R, Sevilla T, Vílchez JJ, Martínez-Rubio D, Chumillas MJ, Vázquez JF et al (2013) Charcot–Marie–Tooth disease: genetic and clinical spectrum in a Spanish clinical series. Neurology 81(18):1617–1625. https://doi.org/10.1212/WNL.0b013e3182a9f56a
Gess B, Schirmacher A, Boentert M, Young P (2013) Charcot–Marie–Tooth disease: frequency of genetic subtypes in a German neuromuscular center population. Neuromuscul Disord 23(8):647–651. https://doi.org/10.1016/j.nmd.2013.05.005
Manganelli F, Tozza S, Pisciotta C, Bellone E, Iodice R, Nolano M et al (2014) Charcot–Marie–Tooth disease: frequency of genetic subtypes in a Southern Italy population. J Peripher Nerv Syst 19(4):292–298. https://doi.org/10.1111/jns.12092
Hayashi M, Abe A, Murakami T, Yamao S, Arai H, Hattori H et al (2013) Molecular analysis of the genes causing recessive demyelinating Charcot-Marie-Tooth disease in Japan. J Hum Genet 58(5):273–278. https://doi.org/10.1038/jhg.2013.15
Felice KJ, Whitaker CH, Khorasanizadeh S (2021) Diagnostic yield of advanced genetic testing in patients with hereditary neuropathies: a retrospective single-site study. Muscle Nerve 64(4):454–461. https://doi.org/10.1002/mus.27368
Bissar-Tadmouri N, Parman Y, Boutrand L, Deymeer F, Serdaroglu P, Vandenberghe A et al (2000) Mutational analysis and genotype/phenotype correlation in Turkish Charcot-Marie-Tooth type 1 and HNPP patients. Clin Genet 58(5):396–402. https://doi.org/10.1034/j.1399-0004.2000.580511.x
Deymeer F, Matur Z, Poyraz M, Battaloglu E, Oflazer-Serdaroglu P, Parman Y (2011) Nerve conduction studies in Charcot-Marie-Tooth disease in a cohort from Turkey. Muscle Nerve 43(5):657–664. https://doi.org/10.1002/mus.21932
Yalcintepe S, Gurkan H, Dogan IG, Demir S, Sag SO, Kabayegit ZM et al (2021) The ımportance of multiple gene analysis for diagnosis and differential diagnosis in Charcot Marie Tooth disease. Turk Neurosurg 31(6):888–895. https://doi.org/10.5137/1019-5149.JTN.33661-21.3
Candayan A, Çakar A, Yunisova G, ÖzdağAcarlı AN, Atkinson D, Topaloğlu P et al (2021) Genetic survey of autosomal recessive peripheral neuropathy cases unravels high genetic heterogeneity in a Turkish cohort. Neurol Genet 7(5):e621. https://doi.org/10.1212/NXG.0000000000000621
Candayan A, Parman Y, Battaloğlu E (2022) Clinical and genetic survey for Charcot-Marie-Tooth neuropathy based on the findings in Turkey, a country with a high rate of consanguineous marriages. Balkan Med J 39(1):3–11. https://doi.org/10.4274/balkanmedj.galenos.2021.2021-11-13
Volodarsky M, Kerkhof J, Stuart A, Levy M, Brady LI, Tarnopolsky M et al (2021) Comprehensive genetic sequence and copy number analysis for Charcot-Marie-Tooth disease in a Canadian cohort of 2517 patients. J Med Genet 58(4):284–288. https://doi.org/10.1136/jmedgenet-2019-106641
Milley GM, Varga ET, Grosz Z, Nemes C, Arányi Z, Boczán J et al (2018) Genotypic and phenotypic spectrum of the most common causative genes of Charcot-Marie-Tooth disease in Hungarian patients. Neuromuscul Disord 28(1):38–43. https://doi.org/10.1016/j.nmd.2017.08.007
Lorefice L, Murru MR, Coghe G, Fenu G, Corongiu D, Frau J et al (2017) Charcot-Marie-Tooth disease: genetic subtypes in the Sardinian population. Neurol Sci 38(6):1019–1025. https://doi.org/10.1007/s10072-017-2905-x
Vaeth S, Christensen R, Dunø M, Lildballe DL, Thorsen K, Vissing J et al (2019) Genetic analysis of Charcot-Marie-Tooth disease in Denmark and the implementation of a next generation sequencing platform. Eur J Med Genet 62(1):1–8. https://doi.org/10.1016/j.ejmg.2018.04.003
Kleopa KA, Abrams CK, Scherer SS (2012) How do mutations in GJB1 cause X-linked Charcot-Marie-Tooth disease? Brain Res 1487:198–205. https://doi.org/10.1016/j.brainres.2012.03.068
Shy ME, Siskind C, Swan ER, Krajewski KM, Doherty T, Fuerst DR et al (2007) CMT1X phenotypes represent loss of GJB1 gene function. Neurology 68(11):849–855. https://doi.org/10.1212/01.wnl.0000256709.08271.4d
Bort S, Nelis E, Timmerman V, Sevilla T, Cruz-Martínez A, Martínez F et al (1997) Mutational analysis of the MPZ, PMP22 and Cx32 genes in patients of Spanish ancestry with Charcot-Marie-Tooth disease and hereditary neuropathy with liability to pressure palsies. Hum Genet 99(6):746–754. https://doi.org/10.1007/s004390050442
Lu YY, Lyu H, Jin SQ, Zuo YH, Liu J, Wang ZX et al (2017) Clinical and genetic features of Chinese X-linked Charcot-Marie-Tooth type 1 disease. Chin Med J (Engl) 130(9):1049–1054. https://doi.org/10.4103/0366-6999.204925
Tsai PC, Yang DM, Liao YC, Chiu TY, Kuo HC, Su YP et al (2016) Clinical and biophysical characterization of 19 GJB1 mutations. Ann Clin Transl Neurol 3(11):854–865. https://doi.org/10.1002/acn3.347
Hauw F, Fargeot G, Adams D, Attarian S, Cauquil C, Chanson JB et al (2021) Charcot-Marie-Tooth disease misdiagnosed as chronic inflammatory demyelinating polyradiculoneuropathy: an international multicentric retrospective study. Eur J Neurol 28(9):2846–2854. https://doi.org/10.1111/ene.14950
Bortolozzi M (2018) What’s the function of connexin 32 in the peripheral nervous system? Front Mol Neurosci 11:227. https://doi.org/10.3389/fnmol.2018.00227
Vondracek P, Seeman P, Hermanova M, Fajkusova L (2005) X-linked Charcot-Marie-Tooth disease: phenotypic expression of a novel mutation Ile127Ser in the GJB1 (connexin 32) gene. Muscle Nerve 31(2):252–255. https://doi.org/10.1002/mus.20166
Nicholson GA, Yeung L, Corbett A (1998) Efficient neurophysiologic selection of X-linked Charcot-Marie-Tooth families: ten novel mutations. Neurology 51(5):1412–1416. https://doi.org/10.1212/wnl.51.5.1412
Dubourg O, Azzedine H, Verny C, Durosier G, Birouk N, Gouider R et al (2006) Autosomal-recessive forms of demyelinating Charcot-Marie-Tooth disease. Neuromol Med 8:75–86. https://doi.org/10.1385/nmm:8:1-2:75
Patzkó A, Shy ME (2011) Update on Charcot-Marie-Tooth disease. Curr Neurol Neurosci Rep 11(1):78–88. https://doi.org/10.1007/s11910-010-0158-7
Marat AL, Dokainish H, McPherson PS (2011) DENN domain proteins: regulators of Rab GTPases. J Biol Chem 286(16):13791–13800. https://doi.org/10.1074/jbc.R110.217067
Hirano R, Takashima H, Umehara F, Arimura H, Michizono K, Okamoto Y et al (2004) SET binding factor 2 (SBF2) mutation causes CMT4B with juvenile onset glaucoma. Neurology 63(3):577–580. https://doi.org/10.1212/01.wnl.0000133211.40288.9a
Azzedine H, Bolino A, Taïeb T, Birouk N, Di Duca M, Bouhouche A et al (2003) Mutations in MTMR13, a new pseudophosphatase homologue of MTMR2 and Sbf1, in two families with an autosomal recessive demyelinating form of Charcot-Marie-Tooth disease associated with early-onset glaucoma. Am J Hum Genet 72(5):1141–1153. https://doi.org/10.1086/375034
Senderek J, Bergmann C, Weber S, Ketelsen UP, Schorle H, Rudnik-Schöneborn S et al (2003) Mutation of the SBF2 gene, encoding a novel member of the myotubularin family, in Charcot-Marie-Tooth neuropathy type 4B2/11p15. Hum Mol Genet 12(3):349–356. https://doi.org/10.1093/hmg/ddg030
Robinson FL, Dixon JE (2005) The phosphoinositide-3-phosphatase MTMR2 associates with MTMR13, a membrane-associated pseudophosphatase also mutated in type 4B Charcot-Marie-Tooth disease. J Biol Chem 280(36):31699–31707. https://doi.org/10.1074/jbc.M505159200
Jordanova A, De Jonghe P, Boerkoel CF, Takashima H, De Vriendt E, Ceuterick C et al (2003) Mutations in the neurofilament light chain gene (NEFL) cause early onset severe Charcot-Marie-Tooth disease. Brain 126(Pt 3):590–597. https://doi.org/10.1093/brain/awg059
Mersiyanova IV, Perepelov AV, Polyakov AV, Sitnikov VF, Dadali EL, Oparin RB et al (2000) A new variant of Charcot-Marie-Tooth disease type 2 is probably the result of a mutation in the neurofilament-light gene. Am J Hum Genet 67(1):37–46. https://doi.org/10.1086/302962
Georgiou D-M, Zidar J, Korosec M, Middleton LT, Kyriakides T, Christodoulou K (2002) A novel NF-L mutation pro22-to-ser is associated with CMT2 in a large Slovenian family. Neurogenetics 4(2):93–96. https://doi.org/10.1007/s10048-002-0138-4
Berciano J, García A, Peeters K, Gallardo E, De Vriendt E, Palayo-Negro AL et al (2015) NEFL E396K mutation is associated with a novel dominant intermediate Charcot-Marie-Tooth disease phenotype. J Neurol 262(5):1289–1300. https://doi.org/10.1007/s00415-015-7709-4
Abe A, Numakura C, Saito K, Koide H, Oka N, Honma A et al (2009) Neurofilament light chain polypeptide gene mutations in Charcot-Marie-Tooth disease: nonsense mutation probably causes a recessive phenotype. J Hum Genet 54(2):94–97. https://doi.org/10.1038/jhg.2008.13
Yum SW, Zhang J, Mo K, Li J, Scherer SS (2009) A novel recessive NEFL mutation causes a severe, early-onset axonal neuropathy. Ann Neurol 66(6):759–770. https://doi.org/10.1002/ana.21728
Sasaki T, Gotow T, Shiozaki M, Sakaue F, Saito T, Julien J-P et al (2006) Aggregate formation and phosphorylation of neurofilament-L Pro22 Charcot-Marie-Tooth disease mutants. Hum Mol Genet 15(6):943–952. https://doi.org/10.1093/hmg/ddl011
Cutrupi AN, Brewer MH, Nicholson GA, Kennerson ML (2018) Structural variations causing inherited peripheral neuropathies: a paradigm for understanding genomic organization, chromatin interactions, and gene dysregulation. Mol Genet Genomic Med 6(3):422–433. https://doi.org/10.1002/mgg3.390
Salpietro V, Manole A, Efthymiou S, Houlden H (2018) A review of copy number variants in inherited neuropathies. Curr Genomics 19(6):412–419. https://doi.org/10.2174/1389202919666180330153316
Author information
Authors and Affiliations
Contributions
Taner KARAKAYA: conceptualization, methodology, ınvestigation, resources, visualization, writing—original draft preparation, writing—review and editing. Ayberk TURKYILMAZ: data curation, ınvestigation, supervision, resources, writing—review and editing. Gunes SAGER: conceptualization, visualization, ınvestigation, resources. Rahsan INAN: resources. Oguzhan YARALI: data curation, resources. Alper Han CEBI: data curation, resources. Yasemin AKIN: resources, supervision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Karakaya, T., Turkyilmaz, A., Sager, G. et al. Molecular characterization of Turkish patients with demyelinating Charcot-Marie-Tooth disease. Neurogenetics 23, 213–221 (2022). https://doi.org/10.1007/s10048-022-00693-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10048-022-00693-6