Abstract
Cancer stem cells (CSCs) encompass a subset of highly aggressive tumor cells that are involved in tumor initiation and progression. This study investigates the function of regulator of calcineurin 2 (RCAN2) in the stem cell property in colorectal cancer (CRC). By analyzing four GEO datasets, we obtained RCAN2 as a stemness-related gene in CRC. RCAN2 was poorly expressed in CRC tissues and cells, especially in CSCs. RCAN2 restoration reduced calcineurin activity and promoted phosphorylation and degradation of nuclear factor of activated T cells 1 (NFATC1) protein, leading to reduced stemness of CSCs. JunD proto-oncogene (JUND), whose protein level was increased in CRC samples and CRC stem cells, bound to RCAN2 and suppressed its transcription. The abundant ubiquitin specific peptidase 7 (USP7) in CSCs enhanced JUND protein stability through deubiquitination modification. Lentivirus-mediated knockdown of USP7 or JUND also blocked the calcineurin-NFATC1 signaling and reduced the protein levels of stemness-related proteins. Moreover, the USP7 knockdown weakened the colony/sphere formation ability as well as the tumorigenicity of CSCs, and it reduced the CSC content in xenograft tumors. However, further restoration of JUND rescued the stemness of the CSCs. Overall, this study demonstrates that USP7-mediated JUND suppresses RCAN2 transcription and activates NFATC1 to enhance stem cell property in CRC.
Graphical abstract
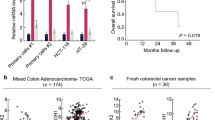
1. RCAN2 is poorly expressed in CRC tissues and cells and especially in CSCs.
2. RCAN2 reduces stemness of CSCs by blocking calcineurin-NFATC1 signal transduction.
3. JUND binds to RCAN2 promoter to suppresses RCAN2 transcription.
4. USP7 enhances JUND protein stability via deubiquitination modification.
5. Downregulation of USP7 or JUND restores RCAN2 level and suppresses stemness of CSCs.









Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article. Additional raw data may be available from the corresponding author for reasonable reasons.
References
Akincilar SC, Chua JYH, Ng QF, Chan CHT, Eslami SZ, Chen K, et al. Identification of mechanism of cancer-cell-specific reactivation of hTERT offers therapeutic opportunities for blocking telomerase specifically in human colorectal cancer. Nucleic Acids Res. 2022. https://doi.org/10.1093/nar/gkac479.
Ashida R, Tominaga K, Sasaki E, Watanabe T, Fujiwara Y, Oshitani N, et al. AP-1 and colorectal cancer. Inflammopharmacology. 2005;13(1–3):113–25. https://doi.org/10.1163/156856005774423935.
Barrett CS, Millena AC, Khan SA. TGF-beta Effects on prostate cancer cell migration and invasion require FosB. Prostate. 2017;77(1):72–81. https://doi.org/10.1002/pros.23250.
Biller LH, Schrag D. Diagnosis and treatment of metastatic colorectal cancer: a review. JAMA. 2021;325(7):669–85. https://doi.org/10.1001/jama.2021.0106.
Brown RE, Jacobse J, Anant SA, Blunt KM, Chen B, Vega PN, et al. MTG16 regulates colonic epithelial differentiation, colitis, and tumorigenesis by repressing E protein transcription factors. JCI Insight 7(10). https://doi.org/10.1172/jci.insight.153045
Calzolari C, Seracini D, Burgio G, Gaeta G, Marvulli I, Giovannucci-Uzielli ML, et al. A new case of fronto-nasal dysplasia associated with craniosynostosis. Pediatr Med Chir. 1988;10(5):537–40.
Cao L, Zhang Q, Cheng S, Chen Z, Hua Z, Yang J, et al. Long non-coding RNAs and genes contributing to the generation of cancer stem cells in hepatocellular carcinoma identified by RNA sequencing analysis. Oncol Rep. 2016;36(5):2619–24. https://doi.org/10.3892/or.2016.5120.
Dekker E, Tanis PJ, Vleugels JLA, Kasi PM, Wallace MB. Colorectal cancer. Lancet. 2019;394(10207):1467–80. https://doi.org/10.1016/S0140-6736(19)32319-0.
Deng F, Wu Z, Xu M, Xia P. YAP activates STAT3 signalling to promote colonic epithelial cell proliferation in DSS-induced colitis and colitis associated cancer. J Inflamm Res. 2022;15:5471–82. https://doi.org/10.2147/JIR.S377077.
Deng J, Liao Y, Liu J, Liu W, Yan D. Research progress on epigenetics of diabetic cardiomyopathy in type 2 diabetes. Front Cell Dev Biol. 2021;9:777258. https://doi.org/10.3389/fcell.2021.777258.
Favoriti P, Carbone G, Greco M, Pirozzi F, Pirozzi RE, Corcione F. Worldwide burden of colorectal cancer: a review. Updates Surg. 2016;68(1):7–11. https://doi.org/10.1007/s13304-016-0359-y.
Fraile JM, Quesada V, Rodriguez D, Freije JM, Lopez-Otin C. Deubiquitinases in cancer: new functions and therapeutic options. Oncogene. 2012;31(19):2373–88. https://doi.org/10.1038/onc.2011.443.
Galoczova M, Coates P, Vojtesek B. STAT3, stem cells, cancer stem cells and p63. Cell Mol Biol Lett. 2018;23:12. https://doi.org/10.1186/s11658-018-0078-0.
Ghaffari S, Hanson C, Schmidt RE, Bouchonville KJ, Offer SM, Sinha S. An integrated multi-omics approach to identify regulatory mechanisms in cancer metastatic processes. Genome Biol. 2021;22(1):19. https://doi.org/10.1186/s13059-020-02213-x.
Gupta R, Bhatt LK, Johnston TP, Prabhavalkar KS. Colon cancer stem cells: potential target for the treatment of colorectal cancer. Cancer Biol Ther. 2019;20(8):1068–82. https://doi.org/10.1080/15384047.2019.1599660.
Hou X, Xia J, Feng Y, Cui L, Yang Y, Yang P, et al. USP47-mediated deubiquitination and stabilization of TCEA3 attenuates pyroptosis and apoptosis of colorectal cancer cells induced by chemotherapeutic doxorubicin. Front Pharmacol. 2021;12:713322. https://doi.org/10.3389/fphar.2021.713322.
Ji Q, Zhou L, Sui H, Yang L, Wu X, Song Q, et al. Primary tumors release ITGBL1-rich extracellular vesicles to promote distal metastatic tumor growth through fibroblast-niche formation. Nat Commun. 2020;11(1):1211. https://doi.org/10.1038/s41467-020-14869-x.
Kim JH, Kim K, Kim I, Seong S, Jeong BC, Nam KI, et al. RCANs regulate the convergent roles of NFATc1 in bone homeostasis. Sci Rep. 2016;6:38526. https://doi.org/10.1038/srep38526.
Li R, Zhou J, Wu X, Li H, Pu Y, Liu N, et al. Jianpi Jiedu Recipe inhibits colorectal cancer liver metastasis via regulating ITGBL1-rich extracellular vesicles mediated activation of cancer-associated fibroblasts. Phytomedicine. 2022;100:154082. https://doi.org/10.1016/j.phymed.2022.154082.
Li X, Kong L, Yang Q, Duan A, Ju X, Cai B, et al. Parthenolide inhibits ubiquitin-specific peptidase 7 (USP7), Wnt signaling, and colorectal cancer cell growth. J Biol Chem. 2020;295(11):3576–89. https://doi.org/10.1074/jbc.RA119.011396.
Liang Q, Wang Y, Lu Y, Zhu Q, Xie W, Tang N, et al. RANK promotes colorectal cancer migration and invasion by activating the Ca(2+)-calcineurin/NFATC1-ACP5 axis. Cell Death Dis. 2021;12(4):336. https://doi.org/10.1038/s41419-021-03642-7.
Ling H, Cao CH, Han K, Lv YR, Ma XD, Cao JH, et al. CEP63 upregulates YAP1 to promote colorectal cancer progression through stabilizing RNA binding protein FXR1. Oncogene. 2022;41(39):4433–45. https://doi.org/10.1038/s41388-022-02439-y.
Liu H, Wang K, Chen S, Sun Q, Zhang Y, Chen L, et al. NFATc1 phosphorylation by DYRK1A increases its protein stability. PLoS One. 2017;12:e0172985. https://doi.org/10.1371/journal.pone.0172985.
Liu K, Jiang L, Shi Y, Liu B, He Y, Shen Q, et al. Hypoxia-induced GLT8D1 promotes glioma stem cell maintenance by inhibiting CD133 degradation through N-linked glycosylation. Cell Death Differ. 2022;29(9):1834–49. https://doi.org/10.1038/s41418-022-00969-2.
Liu K, Pu J, Nie Z, Shi Y, Jiang L, Wu Q, et al. Ivacaftor inhibits glioblastoma stem cell maintenance and tumor progression. Front Cell Dev Biol. 2021a;9:678209. https://doi.org/10.3389/fcell.2021.678209.
Liu Y, Wang C, Cheng P, Zhang S, Zhou W, Xu Y, et al. FHL1 inhibits the progression of colorectal cancer by regulating the Wnt/beta-catenin signaling pathway. J Cancer. 2021b;12(17):5345–54. https://doi.org/10.7150/jca.60543.
Munro MJ, Wickremesekera SK, Peng L, Tan ST, Itinteang T. Cancer stem cells in colorectal cancer: a review. J Clin Pathol. 2018;71(2):110–6. https://doi.org/10.1136/jclinpath-2017-204739.
Niitsu H, Hinoi T, Kawaguchi Y, Sentani K, Yuge R, Kitadai Y, et al. KRAS mutation leads to decreased expression of regulator of calcineurin 2, resulting in tumor proliferation in colorectal cancer. Oncogenesis. 2016;5(8):e253. https://doi.org/10.1038/oncsis.2016.47.
Novellasdemunt L, Foglizzo V, Cuadrado L, Antas P, Kucharska A, Encheva V, et al. USP7 Is a tumor-specific WNT activator for APC-mutated colorectal cancer by mediating beta-catenin deubiquitination. Cell Rep. 2017;21(3):612–27. https://doi.org/10.1016/j.celrep.2017.09.072.
Ruiz EJ, Lan L, Diefenbacher ME, Riising EM, Da Costa C, Chakraborty A, et al. JunD, not c-Jun, is the AP-1 transcription factor required for Ras-induced lung cancer. JCI Insight. 2021;6(13). https://doi.org/10.1172/jci.insight.124985
Siegel RL, Miller KD, Goding Sauer A, Fedewa SA, Butterly LF, Anderson JC, et al. Colorectal cancer statistics, 2020. CA Cancer J Clin. 2020;70(3):145–64. https://doi.org/10.3322/caac.21601.
Singh SK, Chen NM, Hessmann E, Siveke J, Lahmann M, Singh G, et al. Antithetical NFATc1-Sox2 and p53-miR200 signaling networks govern pancreatic cancer cell plasticity. EMBO J. 2015;34(4):517–30. https://doi.org/10.15252/embj.201489574.
Song Y, Jiang Y, Tao D, Wang Z, Wang R, Wang M, et al. NFAT2-HDAC1 signaling contributes to the malignant phenotype of glioblastoma. Neuro Oncol. 2020;22(1):46–57. https://doi.org/10.1093/neuonc/noz136.
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209–49. https://doi.org/10.3322/caac.21660.
Vasefifar P, Motafakkerazad R, Maleki LA, Najafi S, Ghrobaninezhad F, Najafzadeh B, et al. Nanog, as a key cancer stem cell marker in tumor progression. Gene. 2022;827:146448. https://doi.org/10.1016/j.gene.2022.146448.
Walcher L, Kistenmacher AK, Suo H, Kitte R, Dluczek S, Strauss A, et al. Cancer stem cells-origins and biomarkers: perspectives for targeted personalized therapies. Front Immunol. 2020;11:1280. https://doi.org/10.3389/fimmu.2020.01280.
Wang J, Shang L, Zhang J, Yu Z, Huang J, Jin J, et al. Nfatc1(+) colonic stem cells contribute to regeneration upon colitis. J Gastroenterol Hepatol. 2022;37(4):734–40. https://doi.org/10.1111/jgh.15790.
Wang X, Ghareeb WM, Zhang Y, Yu Q, Lu X, Huang Y, et al. Hypermethylated and downregulated MEIS2 are involved in stemness properties and oxaliplatin-based chemotherapy resistance of colorectal cancer. J Cell Physiol. 2019;234(10):18180–91. https://doi.org/10.1002/jcp.28451.
Wang Y, Fu J, Jiang M, Zhang X, Cheng L, Xu X, et al. MiR-410 is overexpressed in liver and colorectal tumors and enhances tumor cell growth by silencing FHL1 via a direct/indirect mechanism. PLoS One. 2014;9(10):e108708. https://doi.org/10.1371/journal.pone.0108708.
Xiao B, Liu L, Chen Z, Li A, Xia Y, Wang P, et al. A novel overall survival prediction signature based on cancer stem cell-related genes in osteosarcoma. Front Cell Dev Biol. 2021;9:753414. https://doi.org/10.3389/fcell.2021.753414.
Xu H, Liu L, Li W, Zou D, Yu J, Wang L, et al. Transcription factors in colorectal cancer: molecular mechanism and therapeutic implications. Oncogene. 2021;40(9):1555–69. https://doi.org/10.1038/s41388-020-01587-3.
Xu Y, Chen J, Xiao L, Chung HK, Zhang Y, Robinson JC, et al. Transcriptional regulation of importin-alpha1 by JunD modulates subcellular localization of RNA-binding protein HuR in intestinal epithelial cells. Am J Physiol Cell Physiol. 2016;311(6):C874–83. https://doi.org/10.1152/ajpcell.00209.2016.
Yang P, Xie J, Li Y, Lin HP, Fenske W, Clementino M, et al. Deubiquitinase USP7-mediated MCL-1 up-regulation enhances arsenic and benzo(a)pyrene co-exposure-induced cancer stem cell-like property and tumorigenesis. Theranostics. 2020;10(20):9050–65. https://doi.org/10.7150/thno.47897.
Zhu Y, Gu L, Lin X, Cui K, Liu C, Lu B, et al. LINC00265 promotes colorectal tumorigenesis via ZMIZ2 and USP7-mediated stabilization of beta-catenin. Cell Death Differ. 2020;27(4):1316–27. https://doi.org/10.1038/s41418-019-0417-3.
Funding
This work was supported by Pudong New Area Science and Technology Development Fund for People’s Livelihood Research Projects of Public Institutions (Medical and Health Projects) (No. PKJ2021-Y24).
Author information
Authors and Affiliations
Contributions
Y.L.C. wrote the original draft, participated in the design of the study, and performed the experiments. L.L.C. performed the experiments, data collection, and interpretation. J.T. and G.Y.C. performed the experiments and analyzed the data. J.R.J. and M.X. provided resources, administration supports, and data amendment. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All patients signed the informed consent form. The present study was approved by the Ethics Committee of the Pudong New Area People’s Hospital (No. PAPH20210122).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chang, Y., Chen, L., Tang, J. et al. USP7-mediated JUND suppresses RCAN2 transcription and elevates NFATC1 to enhance stem cell property in colorectal cancer. Cell Biol Toxicol 39, 3121–3140 (2023). https://doi.org/10.1007/s10565-023-09822-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-023-09822-9