Abstract
Background
Chimeric antigen receptor (CAR)-T-cell therapy is a revolutionary treatment that has become a mainstay of advanced cancer treatment. Conventional glypican-3 (GPC3)-CAR-T cells have not produced ideal clinical outcomes in advanced hepatocellular carcinoma (HCC), and the mechanism is unclear. This study aims to investigate the clinical utility of novel GPC3-7–19-CAR-T cells constructed by our team and to explore the mechanisms underlying their antitumor effects.
Methods
We engineered a novel GPC3-targeting CAR including an anti-GPC3 scFv, CD3ζ, CD28 and 4-1BB that induces co-expression of IL-7 at a moderate level (500 pg/mL) and CCL19 at a high level (15000 pg /mL) and transduced it into human T cells. In vitro, cell killing efficacy was validated by the xCELLigence RTCA system, LDH nonradioactive cytotoxicity assay and was confirmed in primary HCC organoid models employing a 3D microfluid chip. In vivo, the antitumor capacity was assessed in a humanized NSG mouse xenograft model. Finally, we initiated a phase I clinical trial to evaluate the safety and effect of GPC3-7–19-CAR-T cells in the clinic.
Results
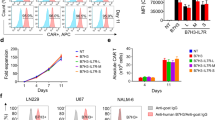
GPC3-7–19-CAR-T cells had 1.5–2 times higher killing efficiency than GPC3-CAR-T cells. The tumor formation rates in GPC3-7–19-CAR-T cells treated model were reduced (3/5vs.5/5), and the average tumor volumes were 0.74 cm3 ± 1.17 vs. 0.34 cm3 ± 0.25. Of note, increased proportion of CD4+ TEM and CD8+ TCM cells was infiltrated in GPC3-7–19-CAR-T cells group. GPC3-7–19-CAR-T cells obviously reversed the immunosuppressive tumor microenvironment (TME) by reducing polymorphonuclear (PMN)-myeloid-derived suppressor cells (MDSCs) and regulatory T (Treg) cells infiltration and recruiting more dendritic cells (DCs) to HCC xenograft tumor tissues. In one patient with advanced HCC, GPC3-7–19-CAR-T-cell treatment resulted in tumor reduction 56 days after intravenous infusion.
Conclusions
In conclusion, GPC3-7–19-CAR-T cells achieved antitumor effects superior to those of conventional GPC3-CAR-T cells by reconstructing the TME induced by the dominant CD4+ TEM and CD8+ TCM cell subsets. Most importantly, GPC3-7–19-CAR-T cells exhibited good safety and antitumor efficacy in HCC patients in the clinic.
Graphical Abstract
► Novel GPC3-7-19-CAR-T cells designed with mediate level of IL-7 secretion and high level of CCL19 secretion, which could recruit more mature DCs to assist killing on GPC3+HCCs.
►DC cells recruited by CCL19 could interact with CD4+ T cells and promote the differentiation of CD4+TEFF cells into CD4+TEM and CD8+TCM subsets, leading a better anti-tumor effect on GPC3+HCCs.
►Compared with conventional GPC3-CAR-T, GPC3-7-CCL19-CAR-T cells could reverse tumor immunosuppressive microenvironment by reducing PMN-MDSC and Treg cell infiltration.








Similar content being viewed by others
Data and materials availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- CAR:
-
Chimeric antigen receptor
- ScFv:
-
Single-chain variable fragment
- GPC3:
-
Conventional glypican-3
- HCC:
-
Hepatocellular carcinoma
- IL:
-
Interleukin
- IFN:
-
Interferon
- TNF:
-
Tumor necrosis factor
- TGF:
-
Transforming growth factor
- CCL:
-
Chemokine (C–C motif) ligand
- TME:
-
Tumor microenvironment
- TIME:
-
Tumor immune microenvironment
- PMN:
-
Polymorphonuclear
- MDSCs:
-
Myeloid-derived suppressor cells
- M-MDSCs:
-
Monocyte-like MDSCs
- PMN-MDSCs:
-
Polymorphonuclear-like-MDSCs
- Treg :
-
Regulatory T-cells
- Th :
-
T helper cells
- Ts :
-
Cytotoxic T cells
- Tcm :
-
Central memory T cells
- Tem :
-
Effector memory T cells
- TDE :
-
Terminally differentiated T cells
- DCs:
-
Dendritic cells
- NK:
-
Natural killer
- PBMC:
-
Peripheral blood mononuclear cell
- Mono:
-
Monocytes
- PB:
-
Peripheral blood
- T2A:
-
2A peptide
- s.c:
-
Subcutaneous injection
- i.v:
-
Intravenous injection
- TCM :
-
Central memory T cell
- TEM :
-
Effector memory T cell
- PFS:
-
Progression-free survival
- TAAs:
-
Tumor-associated antigens
- E/T:
-
Effector-to-target
- SD:
-
Stable response
- PK:
-
Pharmacokinetic
- PD:
-
Pharmacodynamic
- RECIST:
-
Response Evaluation Criteria in Solid Tumors
References
Abou-Alfa GK, Puig O, Daniele B, et al. Randomized phase II placebo controlled study of codrituzumab in previously treated patients with advanced hepatocellular carcinoma. J Hepatol. 2016;65(2):289–95. https://doi.org/10.1016/j.jhep.2016.04.004.
Adachi K, Kano Y, Nagai T, et al. IL-7 and CCL19 expression in CAR-T cells improves immune cell infiltration and CAR-T cell survival in the tumor. Nat Biotechnol. 2018;36(4):346–51. https://doi.org/10.1038/nbt.4086.
Alizadeh D, Wong RA, Yang X, et al. IL15 Enhances CAR-T Cell Antitumor Activity by Reducing mTORC1 Activity and Preserving Their Stem Cell Memory Phenotype. Cancer Immunol Res. 2019;7(5):759–72. https://doi.org/10.1158/2326-6066.CIR-18-0466.
Baier JL, Mattner J. Mechanisms of autoimmune liver disease. Discov Med. 2014;18(100):255–63.
Binnewies M, Roberts EW, Kersten K, et al. Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat Med. 2018;24(5):541–50. https://doi.org/10.1038/s41591-018-0014-x.
Chabannon C, Bonini C. Structure of and Signalling Through Chimeric Antigen Receptor. 2022:3–5. https://doi.org/10.1007/978-3-030-94353-0_1.
Feucht J, Sun J, Eyquem J, et al. Calibration of CAR activation potential directs alternative T cell fates and therapeutic potency. Nat Med. 2019;25(1):82–8. https://doi.org/10.1038/s41591-018-0290-5.
Goto S, Sakoda Y, Adachi K, et al. Enhanced anti-tumor efficacy of IL-7/CCL19-producing human CAR-T cells in orthotopic and patient-derived xenograft tumor models. Cancer Immunol Immunother. 2021;70(9):2503–15. https://doi.org/10.1007/s00262-021-02853-3.
Hong M, Clubb JD, Chen YY. Engineering CAR-T Cells for Next-Generation Cancer Therapy. Cancer Cell. 2020;38(4):473–88. https://doi.org/10.1016/j.ccell.2020.07.005.
Hu B, Ren J, Luo Y, et al. Augmentation of Antitumor Immunity by Human and Mouse CAR T Cells Secreting IL-18. Cell Rep. 2017;20(13):3025–33. https://doi.org/10.1016/j.celrep.2017.09.002.
Ishiguro T, Sugimoto M, Kinoshita Y, et al. Anti-glypican 3 antibody as a potential antitumor agent for human liver cancer. Cancer Res. 2008;68(23):9832–8. https://doi.org/10.1158/0008-5472.CAN-08-1973.
Kudo M. Recent advances in systemic therapy for hepatocellular carcinoma in an aging society: 2020 update. Liver Cancer. 2020;9(6):640–62. https://doi.org/10.1159/000511001.
Li C, Jiang P, Wei S, et al. Regulatory T cells in tumor microenvironment: new mechanisms, potential therapeutic strategies and future prospects. Mol Cancer. 2020;19(1):116. https://doi.org/10.1186/s12943-020-01234-1.
Li X, Ramadori P, Pfister D, et al. The immunological and metabolic landscape in primary and metastatic liver cancer. Nat Rev Cancer. 2021;21(9):541–57. https://doi.org/10.1038/s41568-021-00383-9.
Lin Z, Lu D, Wei X, et al. Heterogeneous responses in hepatocellular carcinoma: the achilles heel of immune checkpoint inhibitors. Am J Cancer Res. 2020;10(4):1085–102.
Lindau D, Gielen P, Kroesen M, et al. The immunosuppressive tumour network: myeloid-derived suppressor cells, regulatory T cells and natural killer T cells. Immunology. 2013;138(2):105–15. https://doi.org/10.1111/imm.12036.
Liu G, Rui W, Zhao X, et al. Enhancing CAR-T cell efficacy in solid tumors by targeting the tumor microenvironment. Cell Mol Immunol. 2021;18(5):1085–95. https://doi.org/10.1038/s41423-021-00655-2.
Nakano K, Orita T, Nezu J, et al. Anti-glypican 3 antibodies cause ADCC against human hepatocellular carcinoma cells. Biochem Biophys Res Commun. 2009;378(2):279–84. https://doi.org/10.1016/j.bbrc.2008.11.033.
Park JH, Riviere I, Gonen M, et al. Long-term follow-up of CD19 CAR therapy in acute lymphoblastic leukemia. N Engl J Med. 2018;378(5):449–59. https://doi.org/10.1056/NEJMoa1709919.
Pedroza-Gonzalez A, Verhoef C, Ijzermans JN, et al. Activated tumor-infiltrating CD4+ regulatory T cells restrain antitumor immunity in patients with primary or metastatic liver cancer. Hepatology. 2013;57(1):183–94. https://doi.org/10.1002/hep.26013.
Qi C, Gong J, Li J, et al. Claudin18.2-specific CAR T cells in gastrointestinal cancers: phase 1 trial interim results. Nat Med. 2022;28(6):1189–98. https://doi.org/10.1038/s41591-022-01800-8.
Ren D, Liu W, Ding S, et al. Protocol for generating human immune system mice and hydrodynamic injection to analyze human hematopoiesis in vivo. STAR Protoc. 2022;3(1):101217. https://doi.org/10.1016/j.xpro.2022.101217.
Rodriguez-Garcia A, Lynn RC, Poussin M, et al. CAR-T cell-mediated depletion of immunosuppressive tumor-associated macrophages promotes endogenous antitumor immunity and augments adoptive immunotherapy. Nat Commun. 2021;12(1):877. https://doi.org/10.1038/s41467-021-20893-2.
Roshan MM, Young A, Reinheimer K, et al. Dynamic assessment of cell viability, proliferation and migration using real time cell analyzer system (RTCA). Cytotechnology. 2015;67(2):379–86. https://doi.org/10.1007/s10616-014-9692-5.
Shalapour S, Lin XJ, Bastian IN, et al. Inflammation-induced IgA+ cells dismantle anti-liver cancer immunity. Nature. 2017;551(7680):340–5. https://doi.org/10.1038/nature24302.
Shimizu Y, Suzuki T, Yoshikawa T, et al. Next-generation cancer immunotherapy targeting glypican-3. Front Oncol. 2019;9:248. https://doi.org/10.3389/fonc.2019.00248.
Tokunaga Y, Sasaki T, Goto S, et al. Enhanced antitumor responses of tumor antigen-specific TCR T cells genetically engineered to produce IL7 and CCL19. Mol Cancer Ther. 2022;21(1):138–48. https://doi.org/10.1158/1535-7163.MCT-21-0400.
Villablanca EJ, Raccosta L, Zhou D, et al. Tumor-mediated liver X receptor-alpha activation inhibits CC chemokine receptor-7 expression on dendritic cells and dampens antitumor responses. Nat Med. 2010;16(1):98–105. https://doi.org/10.1038/nm.2074.
Weber EW, Parker KR, Sotillo E, et al. Transient rest restores functionality in exhausted CAR-T cells through epigenetic remodeling. Science. 2021;372(6537):eaba1786. https://doi.org/10.1126/science.aba1786.
Xie G, Ivica NA, Jia B, et al. CAR-T cells targeting a nucleophosmin neoepitope exhibit potent specific activity in mouse models of acute myeloid leukaemia. Nat Biomed Eng. 2021;5(5):399–413. https://doi.org/10.1038/s41551-020-00625-5.
Yamada Y, Harada M, Yamaguchi A, et al. Technical Performance and Clinical Effectiveness of Drop Type With Adjustable Concentrator-Cell Free and Concentrated Ascites Reinfusion Therapy. Artif Organs. 2017;41(12):1135–44. https://doi.org/10.1111/aor.12933.
Yi M, Zheng X, Niu M, et al. Combination strategies with PD-1/PD-L1 blockade: current advances and future directions. Mol Cancer. 2022;21(1):28. https://doi.org/10.1186/s12943-021-01489-2.
Yu S, Li A, Liu Q, et al. Chimeric antigen receptor T cells: a novel therapy for solid tumors. J Hematol Oncol. 2017;10(1):78. https://doi.org/10.1186/s13045-017-0444-9.
Zhang X, Fu X, Li T, et al. The prognostic value of myeloid derived suppressor cell level in hepatocellular carcinoma: a systematic review and meta-analysis. PLoS One. 2019;14(12):e225327. https://doi.org/10.1371/journal.pone.0225327.
Zhong G, Zhao W, Li Y, et al. MAGEA1 and hTERT Peptide Treatment Improves the Potency of The Dendritic Cell- Cytotoxic T Lymphocytes (DC-CTL) Immunotherapy in DAC Treated Acute Myeloid Leukemia. J Cancer. 2022;13(4):1252–60. https://doi.org/10.7150/jca.66501.
Miao TG, Wang LJ, Ma LW, et al. Effects of radiofrequency ablation therapy on T-cell immune function in patients with primary liver cancer[J]. Chinese Journal of Minimally Invasive Surgery, 2016;16(06):538–540.
Acknowledgements
We are grateful to the team of Professor Yan Li and Shanghai Model Organism for providing the humanized NSG mouse model and teaching us how to perform the animal experiments. We are also grateful to Zhengjun Zhou PhD for helping us establish the 3D microfluidic model of HCC. Finally, we would like to thank the surgeons who acquired the resected samples from patients during surgery.
Funding
This project was supported by grants from the National Natural Science Foundation of China (82073216), the Projection of Shanghai Science and Technology Committee (20S11906300, 21ZR1477600), the youth project of Shanghai Municipal Health Commission (20204Y0229), Sailing Project of “Scientific and Technological Innovation Action Plan” of Shanghai Science and Technology Commission (20YF1406100). Shanghai Municipal Health Commission, Collaborative Innovation Cluster Project, 2019CXJQ02.
Author information
Authors and Affiliations
Contributions
Weizhong Wu developed the study concept and supervised this project. Lili Lu performed the in-vitro essay and wrote the manuscript. Bin Lu designed CAR structure and generated the CAR plasmids. Jinjin Bai prepared lentivirus. Shuxiu Xiao made the animal essay and processed data. Zhiyuan Lin was responsible for statistical analysis. Zhengqing Song helped with the in vivo experiments. All authors read and approved the final manuscript. Wei Li and Yuhong Zhou were responsible for the clinical trial regimen and patient administration.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The Ethics Committee of the Zhongshan Hospital Biomedical Research Department provided ethical approval (Approval No. B2020-211R), and informed consent for collecting and preserving samples and details was obtained from each patient.
Xenograft of humanized NSG mice experiments were approved by the Animal Experimentation Ethics Committee of Zhongshan Hospital, Fudan University (supplementary materials). And all the humanized mice owned qualification certificate (2017010014018) and production license.
The clinical trial has been registered at Chinese Clinical Trial Registery (www.chictr.org.cn) as ChiCTR2000036458.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Li-Li Lu, Shu-xiu Xiao and Zhi-yuan Lin are co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Additional file 1:
Supplementary Figure 1. Establishment of CAR-Ts high expansion system in vitro.
Additional file 2:
Supplementary methods and materials.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lu, LL., Xiao, Sx., Lin, Zy. et al. GPC3-IL7-CCL19-CAR-T primes immune microenvironment reconstitution for hepatocellular carcinoma therapy. Cell Biol Toxicol 39, 3101–3119 (2023). https://doi.org/10.1007/s10565-023-09821-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-023-09821-w