Abstract
Purpose
TRPV1 is a nonselective Ca2+ channel protein that is widely expressed and plays an important role during the occurrence and development of many cancers. Activation of TRPV1 channels can affect tumour progression by regulating proliferation, apoptosis and migration. Some studies have also shown that activating TRPV1 can affect tumour progression by modulating tumour immunity. However, the effects of TRPV1 on the development of non-small cell lung cancer (NSCLC) have not been explored clearly.
Method
The Cancer Genome Atlas (TCGA) database and spatial transcriptomics datasets from 10 × Genomics were used to analyze TRPV1 expression in various tumour tissues. Cell proliferation and apoptosis were examined by cell counting kit 8 (CCK8), colony formation, and flow cytometry. Immunohistochemistry, qPCR, and western blotting were used to determine the mRNA and protein expression levels of TRPV1 and other related molecules. Tumour xenografts in BALB/C and C57BL/6J mice were used to determine the effects of TRPV1 on NSCLC development in vivo. Neurotransmitter content was examined by LC-MS/MS, ELISA and Immunohistochemistry. Immune cell infiltration was assessed by flow cytometry.
Results
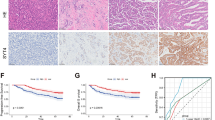
In this study, we found that TRPV1 expression was significantly upregulated in NSCLC and that patients with high TRPV1 expression had a poor prognosis. TRPV1 knockdown can significantly inhibit NSCLC proliferation and induce cell apoptosis through Ca2+-IGF1R signaling. In addition, TRPV1 knockdown resulted in increased infiltration of CD4+ T cells, CD8+ T cells, GZMB+CD8+ T cells and DCs and decreased infiltration of immunosuppressive MDSCs in NSCLC. In addition, TRPV1 knockout effectively decreased the expression of M2 macrophage markers CD163 and increased the expression of M1-associated, costimulatory markers CD86. Knockdown or knockout of TRPV1 significantly inhibit tumour growth and promoted an antitumour immune response through supressing γ-aminobutyric acid (GABA) secretion in NSCLC.
Conclusion
Our study suggests that TRPV1 acts as a tumour promoter in NSCLC, mediating pro-proliferative and anti-apoptotic effects on NSCLC through IGF1R signaling and regulating GABA release to affect the tumour immune response.





Similar content being viewed by others
Data Availability
The datasets generated during the current study are available from the corresponding author on reasonable request.
References
I.S. Ramsey, M. Delling, D.E. Clapham, An introduction to TRP channels. Annu. Rev. Physiol. 68, 619–647 (2006)
K. Yamaguchi et al., Distinct TRPV1- and TRPA1-based mechanisms underlying enhancement of oral ulcerative mucositis-induced pain by 5-fluorouracil. Pain. 157, 1004–1020 (2016)
S. Bertin et al., The ion channel TRPV1 regulates the activation and proinflammatory properties of CD4(+) T cells. Nat. Immunol. 15, 1055–1063 (2014)
L. Li et al., The impact of TRPV1 on Cancer Pathogenesis and Therapy: a systematic review. Int. J. Biol. Sci. 17, 2034–2049 (2021)
M. Hartel et al., Vanilloids in Pancreatic cancer: potential for chemotherapy and pain management. Gut. 55, 519–528 (2006)
R. Marincsak et al., Increased expression of TRPV1 in squamous cell carcinoma of the human tongue. Oral Dis. 15, 328–335 (2009)
G. Czifra et al., Increased expressions of cannabinoid receptor-1 and transient receptor potential vanilloid-1 in human prostate carcinoma. J. Cancer Res. Clin. Oncol. 135, 507–514 (2009)
L.V. Weber et al., Expression and functionality of TRPV1 in Breast cancer cells. Breast Cancer (Dove Med Press. 8, 243–252 (2016)
M.B. Morelli et al., Cross-talk between alpha1D-adrenoceptors and transient receptor potential vanilloid type 1 triggers Prostate cancer cell proliferation. Bmc Cancer. 14, 921 (2014)
B. Sung et al., Capsazepine, a TRPV1 antagonist, sensitizes Colorectal cancer cells to apoptosis by TRAIL through ROS-JNK-CHOP-mediated upregulation of death receptors. Free Radic Biol Med. 53, 1977–1987 (2012)
S. Basu, P. Srivastava, Immunological role of neuronal receptor vanilloid receptor 1 expressed on dendritic cells. Proc. Natl. Acad. Sci. U S A 102, 5120–5125 (2005)
X. Jiang et al., The ion channel TRPV1 gain-of-function reprograms the immune microenvironment to facilitate colorectal tumorigenesis. Cancer Lett. 527, 95–106 (2022)
P. Bryant et al., Capsaicin-sensitive nerves regulate the metabolic response to abdominal sepsis. J. Surg. Res. 112, 152–161 (2003)
Y. Ganor, M. Levite, The neurotransmitter glutamate and human T cells: glutamate receptors and glutamate-induced direct and potent effects on normal human T cells, cancerous human Leukemia and Lymphoma T cells, and autoimmune human T cells. J. Neural Transm (Vienna). 121, 983–1006 (2014)
M. Balood et al., Nociceptor neurons affect cancer immunosurveillance. Nature. 611, 405–412 (2022)
J. Li, Y. Sun, G. Ding, F. Jiang, Persistent pain accelerates xenograft Tumor growth of Breast cancer in rat. Biochem. Biophys. Res. Commun. 495, 2432–2438 (2018)
S. Garcia-Recio et al., Substance P autocrine signaling contributes to persistent HER2 activation that drives malignant progression and drug resistance in Breast cancer. Cancer Res. 73, 6424–6434 (2013)
R. Dantzer, Neuroimmune interactions: from the brain to the Immune System and Vice Versa. Physiol. Rev. 98, 477–504 (2018)
S.H. Jiang et al., Neurotransmitters: emerging targets in cancer. Oncogene. 39, 503–515 (2020)
F. Entschladen et al., Tumour-cell migration, invasion, and Metastasis: navigation by neurotransmitters. Lancet Oncol. 5, 254–258 (2004)
J.K. Bujak et al., Inflammation, Cancer and Immunity-Implication of TRPV1 Channel. Front. Oncol. 9, 1087 (2019)
J. Szolcsanyi, E. Pinter, Z. Helyes, G. Petho, Inhibition of the function of TRPV1-expressing nociceptive sensory neurons by somatostatin 4 receptor agonism: mechanism and therapeutical implications. Curr. Top. Med. Chem. 11, 2253–2263 (2011)
S. Bevan, T. Quallo, D.A. Andersson, TRPV1. Handb. Exp. Pharmacol. 222, 207–245 (2014)
R. Ramer, B. Hinz, Inhibition of cancer cell invasion by cannabinoids via increased expression of tissue inhibitor of matrix metalloproteinases-1. J. Natl. Cancer Inst. 100, 59–69 (2008)
K.C. Thomas et al., Transient receptor potential vanilloid 1 agonists cause endoplasmic reticulum stress and cell death in human lung cells. J. Pharmacol. Exp. Ther. 321, 830–838 (2007)
C.A. Reilly et al., Capsaicinoids cause inflammation and epithelial cell death through activation of vanilloid receptors. Toxicol. Sci. 73, 170–181 (2003)
L.R. Sadofsky et al., Inflammatory stimuli up-regulate transient receptor potential vanilloid-1 expression in human bronchial fibroblasts. Exp. Lung Res. 38, 75–81 (2012)
L. Li et al., Transient Receptor Potential Cation Channel Subfamily V Member 1 expression promotes Chemoresistance in Non-small-cell Lung Cancer. Front. Oncol. 12, 773654 (2022)
C. Crudden et al., The dichotomy of the insulin-like growth factor 1 receptor: RTK and GPCR: friend or foe for cancer treatment? Growth Horm. Igf Res. 25, 2–12 (2015)
M. Pollak, The insulin and insulin-like growth factor receptor family in neoplasia: an update. Nat. Rev. Cancer. 12, 159–169 (2012)
R. Baserga, The insulin-like growth factor I receptor: a key to Tumor growth? Cancer Res. 55, 249–252 (1995)
R. Baserga, F. Peruzzi, K. Reiss, The IGF-1 receptor in cancer biology. Int. J. Cancer. 107, 873–877 (2003)
M.A. Economou et al., Inhibition of VEGF secretion and experimental choroidal neovascularization by picropodophyllin (PPP), an inhibitor of the insulin-like growth factor-1 receptor. Invest. Ophthalmol. Vis. Sci. 49, 2620–2626 (2008)
R. Baserga, The decline and fall of the IGF-I receptor. J. Cell. Physiol. 228, 675–679 (2013)
B.I. Toth, A. Olah, A.G. Szollosi, T. Biro, TRP channels in the skin. Br. J. Pharmacol. 171, 2568–2581 (2014)
Di B.A. Bartolo et al., Calcium and osteoprotegerin regulate IGF1R expression to inhibit vascular calcification. Cardiovasc. Res. 91, 537–545 (2011)
M. Miura et al., Peripheral sensitization caused by insulin-like growth factor 1 contributes to pain hypersensitivity after tissue injury. Pain. 152, 888–895 (2011)
H.S. Kim et al., Attenuation of natural killer cell functions by capsaicin through a direct and TRPV1-independent mechanism. Carcinogenesis. 35, 1652–1660 (2014)
J.P. White, L. Urban, I. Nagy, TRPV1 function in health and Disease. Curr. Pharm. Biotechnol. 12, 130–144 (2011)
C. Vercelli et al., Expression and functionality of TRPV1 receptor in human MCF-7 and canine CF.41 cells. Vet. Comp. Oncol. 13, 133–142 (2015)
N. Erin, Role of sensory neurons, neuroimmune pathways, and transient receptor potential vanilloid 1 (TRPV1) channels in a murine model of Breast cancer Metastasis. Cancer Immunol. Immunother. 69, 307–314 (2020)
A.H. Zahalka, P.S. Frenette, Nerves in cancer. Nat. Rev. Cancer. 20, 143–157 (2020)
M. Watanabe et al., GABA and GABA receptors in the central nervous system and other organs. Int. Rev. Cytol. 213, 1–47 (2002)
C.G. Wong, T. Bottiglieri, O.R. Snead, GABA, gamma-hydroxybutyric acid, and neurological Disease. Ann. Neurol. 54(6), S3–S12 (2003)
D. Huang et al., Cancer-cell-derived GABA promotes beta-catenin-mediated tumour growth and immunosuppression. Nat. Cell. Biol. 24, 230–241 (2022)
M. Matuszek, M. Jesipowicz, Z. Kleinrok, GABA content and GAD activity in gastric cancer. Med. Sci. Monit. 7, 377–381 (2001)
M. Mazurkiewicz et al., GABA level and GAD activity in human and mouse normal and neoplastic mammary gland. J. Exp. Clin. Cancer Res. 18, 247–253 (1999)
Z. Kleinrok et al., GABA content and GAD activity in colon tumors taken from patients with colon Cancer or from xenografted human colon Cancer cells growing as s.c. tumors in athymic nu/nu mice. J. Physiol. Pharmacol. 49, 303–310 (1998)
B. Zhang et al., B cell-derived GABA elicits IL-10(+) macrophages to limit anti-tumour immunity. Nature. 599, 471–476 (2021)
K. Croitoru et al., Selective modulation of the natural killer activity of murine intestinal intraepithelial leucocytes by the neuropeptide substance P. Immunology. 71, 196–201 (1990)
B.M. Janelsins et al., Neurokinin-1 receptor agonists bias therapeutic dendritic cells to induce type 1 immunity by licensing host dendritic cells to produce IL-12. Blood. 121, 2923–2933 (2013)
Funding
This study was supported by the National Natural Science Foundation of China (No. 82173906); the key project of Ministry of Science and Technology, China (2022YFC2010004); Chinese National Major Project for New Drug Innovation. (No. 2019ZX09201-002-006); the key project of Health Commission of Hunan Province (No.202113010141); Natural Science Foundation of Hunan Province, China (No.2021JJ31063 and No.2021JJ31044). Fundamental Research Funds for the Central Universities of Central South University (No.198101066 and No.208111176).
Author information
Authors and Affiliations
Contributions
Yijing He designed and guided the experiments; Yang Wang conducted the experiments, wrote the manuscript, and analyzed the data; Yu Zhang, Jing Ouyang, Hanying Yi, and Shiyu Wang contributed to the cell experiments; Dongbo Liu, Yingying Dai Ziyang Hong and Wenwu Pei helped to use equipment and instruments. Yijing He, Kun Song, Ling Chen, Wei Zhang, Zhaoqian Liu and Howard L. Mcleod supervised and reviewed the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The animal study was reviewed and approved by the Ethics Committee of the Xiangya Hospital, Central South University, Changsha, China.
Consent for publication
All authors agree to publish.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Y., Zhang, Y., Ouyang, J. et al. TRPV1 inhibition suppresses non-small cell lung cancer progression by inhibiting tumour growth and enhancing the immune response. Cell Oncol. (2023). https://doi.org/10.1007/s13402-023-00894-7
Accepted:
Published:
DOI: https://doi.org/10.1007/s13402-023-00894-7