Abstract
Background
Prediction of cardiac surgery-associated acute kidney injury (CS-AKI) in pediatric patients is crucial to improve outcomes and guide clinical decision-making. This study aimed to develop a supervised machine learning (ML) model for predicting moderate to severe CS-AKI at postoperative day 2 (POD2).
Methods
This retrospective cohort study analyzed data from 402 pediatric patients who underwent cardiac surgery at a university-affiliated children’s hospital, who were separated into an 80%-20% train-test split. The ML model utilized demographic, preoperative, intraoperative, and POD0 clinical and laboratory data to predict moderate to severe AKI categorized by Kidney Disease: Improving Global Outcomes (KDIGO) stage 2 or 3 at POD2. Input feature importance was assessed by SHapley Additive exPlanations (SHAP) values. Model performance was evaluated using accuracy, area under the receiver operating curve (AUROC), precision, recall, area under the precision-recall curve (AUPRC), F1-score, and Brier score.
Results
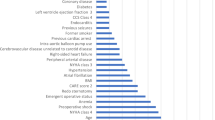
Overall, 13.7% of children in the test set experienced moderate to severe AKI. The ML model achieved promising performance, with accuracy of 0.91 (95% CI: 0.82–1.00), AUROC of 0.88 (95% CI: 0.72–1.00), precision of 0.92 (95% CI: 0.70–1.00), recall of 0.63 (95% CI: 0.32–0.96), AUPRC of 0.81 (95% CI: 0.61–1.00), F1-score of 0.73 (95% CI: 0.46–0.99), and Brier score loss of 0.09 (95% CI: 0.00–0.17). The top ten most important features assessed by SHAP analyses in this model were preoperative serum creatinine, surgery duration, POD0 serum pH, POD0 lactate, cardiopulmonary bypass duration, POD0 vasoactive inotropic score, sex, POD0 hematocrit, preoperative weight, and POD0 serum creatinine.
Conclusions
A supervised ML model utilizing demographic, preoperative, intraoperative, and immediate postoperative clinical and laboratory data showed promising performance in predicting moderate to severe CS-AKI at POD2 in pediatric patients.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information



Similar content being viewed by others
Data availability
Data are available upon reasonable request to the corresponding author.
Abbreviations
- CS-AKI:
-
Cardiac surgery-associated acute kidney injury
- POD:
-
Post-op day
- KDIGO:
-
Kidney Disease: Improving Global Outcomes
- SHAP:
-
SHapley Additive exPlanations
References
Li S, Krawczeski CD, Zappitelli M et al (2011) Incidence, risk factors, and outcomes of acute kidney injury after pediatric cardiac surgery – a prospective multicenter study. Crit Care Med 39:1493–1499. https://doi.org/10.1097/CCM.0b013e31821201d3
Fuhrman DY, Kellum JA (2017) Epidemiology and pathophysiology of cardiac surgery-associated acute kidney injury. Curr Opin Anesthesiol 30:60–65. https://doi.org/10.1097/ACO.0000000000000412
Alten JA, Cooper DS, Blinder JJ et al (2021) Epidemiology of acute kidney injury after neonatal cardiac surgery: a report from the multicenter neonatal and pediatric heart and renal outcomes network. Crit Care Med 49:e941–e951. https://doi.org/10.1097/CCM.0000000000005165
Dong J, Feng T, Thapa-Chhetry B et al (2021) Machine learning model for early prediction of acute kidney injury (AKI) in pediatric critical care. Crit Care 25:288. https://doi.org/10.1186/s13054-021-03724-0
Deng Y-H, Luo X-Q, Yan P et al (2022) Outcome prediction for acute kidney injury among hospitalized children via eXtreme Gradient Boosting algorithm. Sci Rep 12:8956. https://doi.org/10.1038/s41598-022-13152-x
Luo X-Q, Kang Y-X, Duan S-B et al (2023) Machine learning-based prediction of acute kidney injury following pediatric cardiac surgery: model development and validation study. J Med Internet Res 25:e41142. https://doi.org/10.2196/41142
Gist KM, SooHoo M, Mack E et al (2022) Modifying the renal angina index for predicting AKI and related adverse outcomes in pediatric heart surgery. World J Pediatr Congenit Heart Surg 13:196–202. https://doi.org/10.1177/21501351211073615
Onder AM, Rosen D, Mullett C et al (2016) Comparison of intraoperative aminophylline versus furosemide in treatment of oliguria during pediatric cardiac surgery. Pediatr Crit Care Med 17:753–763. https://doi.org/10.1097/PCC.0000000000000834
Khwaja A (2012) KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract 120:c179–c184. https://doi.org/10.1159/000339789
Ke G, Meng Q, Finley T, Wang T, Chen W, Ma W, Ye Q,, Liu T-Y (2017) LightGBM: A Highly Efficient Gradient Boosting Decision Tree. Proceedings of the 31st International Conference on Neural Information Processing Systems, Long Beach, p 3149–3157
Qian Q, Wu J, Wang J et al (2021) Prediction models for AKI in ICU: a comparative study. Int J Gen Med 14:623–632. https://doi.org/10.2147/IJGM.S289671
Lundberg SM, Lee S-I (2017) A unified approach to interpreting model predictions. In: Guyon I, Luxburg UV, Bengio S et al (eds) Advances in neural information processing systems 30. Curran Associates Inc, Red Hook, NY, pp 4765–4774
Jefferies JL, Devarajan P (2016) Early detection of acute kidney injury after pediatric cardiac surgery. Prog Pediatr Cardiol 41:9–16. https://doi.org/10.1016/j.ppedcard.2016.01.011
Tseng P-Y, Chen Y-T, Wang C-H et al (2020) Prediction of the development of acute kidney injury following cardiac surgery by machine learning. Crit Care 24:478. https://doi.org/10.1186/s13054-020-03179-9
Mohamadlou H, Lynn-Palevsky A, Barton C et al (2018) Prediction of acute kidney injury with a machine learning algorithm using electronic health record data. Can J Kidney Health Dis 5:2054358118776326. https://doi.org/10.1177/2054358118776326
Lee H-C, Yoon H-K, Nam K et al (2018) Derivation and validation of machine learning approaches to predict acute kidney injury after cardiac surgery. J Clin Med 7:322. https://doi.org/10.3390/jcm7100322
Penny-Dimri JC, Bergmeir C, Reid CM et al (2021) Machine learning algorithms for predicting and risk profiling of cardiac surgery-associated acute kidney injury. Semin Thorac Cardiovasc Surg 33:735–745. https://doi.org/10.1053/j.semtcvs.2020.09.028
Choe SH, Cho H, Bae J et al (2021) Severity and duration of acute kidney injury and chronic kidney disease after cardiac surgery. J Clin Med 10:1556. https://doi.org/10.3390/jcm10081556
Kiessling A-H, Dietz J, Reyher C et al (2014) Early postoperative serum cystatin C predicts severe acute kidney injury following cardiac surgery: a post-hoc analysis of a randomized controlled trial. J Cardiothorac Surg 9:10. https://doi.org/10.1186/1749-8090-9-10
Krawczeski CD, Woo JG, Wang Y et al (2011) Neutrophil gelatinase-associated lipocalin concentrations predict development of acute kidney injury in neonates and children after cardiopulmonary bypass. J Pediatr 158:1009-1015.e1. https://doi.org/10.1016/j.jpeds.2010.12.057
Guzzi LM, Bergler T, Binnall B et al (2019) Clinical use of [TIMP-2]•[IGFBP7] biomarker testing to assess risk of acute kidney injury in critical care: guidance from an expert panel. Crit Care 23:225. https://doi.org/10.1186/s13054-019-2504-8
Lee J-H, Jung J-Y, Park S-W et al (2018) Risk factors of acute kidney injury in children after cardiac surgery. Acta Anaesthesiol Scand 62:1374–1382. https://doi.org/10.1111/aas.13210
Song X, Liu X, Liu F, Wang C (2021) Comparison of machine learning and logistic regression models in predicting acute kidney injury: a systematic review and meta-analysis. Int J Med Inf 151:104484. https://doi.org/10.1016/j.ijmedinf.2021.104484
Morooka H, Kasugai D, Tanaka A et al (2020) Prognostic impact of parameters of metabolic acidosis in critically Ill children with acute kidney injury: a retrospective observational analysis using the PIC database. Diagnostics 10:937. https://doi.org/10.3390/diagnostics10110937
Acknowledgements
We thank Sherry Kanosky, NP; Tammy Glover, RN; Hafiz Imran Iqbal, MD; Eric Seachrist, MD; and Lennie Samsell, BS, for their extensive chart reviews and retrieval of the data; Kelly Gustafson, RN, for her intraoperative care and efforts; Lesley Cottrell, PhD, for her diligent efforts to structure and organize the data and complete the initial statistical analysis from the dataset; the physicians, nurses, and the medical students who supported the study; and the children and their families who participated in the study and allowed us to learn from their data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Definitions
Baseline serum creatinine: This value is retrieved from laboratory data obtained within the most recent 48 h prior to surgery.
Postoperative day 0 (POD0): This is the day of the surgery, and the laboratory and clinical data points are retrieved from the samples that were obtained immediately after arrival at the cardiac intensive care unit (ICU).
Postoperative eight hours: This data point designates the 8 h after the patient arrives in cardiac ICU.
Postoperative day 1 (POD1): This is the day following surgery and the laboratory and clinical data points are retrieved from the samples that were obtained in that morning between 4:00 AM and 6:00 AM in cardiac ICU as per unit protocol.
Postoperative day 2 (POD2): This is the second day following surgery and the laboratory and clinical data points are retrieved from the samples that were obtained in that morning between 4:00 AM and 6:00 AM in cardiac ICU as per unit protocol.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nagy, M., Onder, A.M., Rosen, D. et al. Predicting pediatric cardiac surgery-associated acute kidney injury using machine learning. Pediatr Nephrol 39, 1263–1270 (2024). https://doi.org/10.1007/s00467-023-06197-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06197-1