Abstract
Objectives
Conventional clipping and endovascular treatment are difficult to apply for some giant intracranial aneurysms (GIAs), and sometimes extracranial-to-intracranial (EC-IC) bypass becomes the optional choice. However, not all GIA patients can benefit from it. This study aims to recognize the underlying problems.
Methods
We included eligible patients in our care. Then, we researched from three levels: a retrospective review of clinical data, fluid-structural analysis from two representative patient-specific models, and fluid-structural interaction analysis for idealized models to investigate the hemodynamic and biomechanical mechanisms.
Results
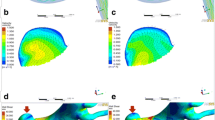
In this article, we report nine patients with GIA who underwent EC-IC surgery. Of them, three experienced dangerous postoperative hemorrhage, and one patient died. Among these three patients, two lacked the A1 segment of the anterior cerebral artery (ACA). The numerical simulation showed that after surgery, for the patient with an unruptured aneurysm and existence of ACA, the wall deformation, wall stress, pressure, and area of the oscillatory shear index (OSI) > 0.2 were decreased by 43%, 39%, 33%, and 13%, while the patient without A1 segment having postoperative hemorrhage showed 36%, 45%, 13%, and 55% increased, respectively. Thus, we postulated a dangerous “stump phenomenon” in such conditions and further demonstrated it from idealized models with different sizes of ACA. Finally, we found a larger anastomosis angle and smaller diameter of the graft can alleviate this effect.
Conclusions
Neurosurgeon should cautiously evaluate the opportunity and risk for such patients who have aplasia of the A1 segment of ACA when making clinical decisions.





Similar content being viewed by others
Data Availability
The original contributions presented in the study are included in the article/ Supplementary Material. Further inquiries can be directed to the corresponding authors.
Abbreviations
- ACA:
-
Anterior cerebral artery
- ALE:
-
Arbitrary Lagrangian–Eulerian
- CFD:
-
Computational fluid dynamics
- CTA:
-
Computed tomography angiography
- EC-IC:
-
Extracranial-to-intracranial
- FSI:
-
Fluid-structural interaction
- GIAs:
-
Giant intracranial aneurysms
- ICA:
-
Internal carotid artery
- MCA:
-
Middle cerebral artery
- NURBS:
-
Non-Uniform Rational B-splines
- OSI:
-
Oscillatory shear index
- RA:
-
Radial artery
- RRT:
-
Relative residence time
- SV:
-
Saphenous vein
- Tawss:
-
Time-averaged wall shear stress
- WSS:
-
Wall shear stress
References
Wiebers, D. O., J. P. Whisnant, J. Huston 3rd., I. Meissner, R. D. Brown Jr., D. G. Piepgras, G. S. Forbes, K. Thielen, D. Nichols, W. M. O’Fallon, J. Peacock, L. Jaeger, N. F. Kassell, G. L. Kongable-Beckman, and J. C. Torner. Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet (Lond, Engl). 362:103–110, 2003.
Raaymakers, T. W., G. J. Rinkel, M. Limburg, and A. Algra. Mortality and morbidity of surgery for unruptured intracranial aneurysms: a meta-analysis. Stroke. 29:1531–1538, 1998.
Drake, C. G. Giant intracranial aneurysms: experience with surgical treatment in 174 patients. Clin Neurosurg. 26:12–95, 1979.
Yasargil, M. Diagnosis and indications for operations in cerebrovascular occlusive disease. Microsurgery applied to neurosurgery Stuttgart. 7:95–119, 1960.
Houkin, K., H. Kamiyama, S. Kuroda, T. Ishikawa, A. Takahashi, and H. Abe. Long-term patency of radial artery graft bypass for reconstruction of the internal carotid artery. J Neurosurg. 90:786–790, 1999.
Yanagisawa, T., H. Kinouchi, T. Sasajima, and H. Shimizu. Long-term follow-up for a giant basilar trunk aneurysm surgically treated by proximal occlusion and external carotid artery to posterior cerebral artery bypass using a saphenous vein graft. J. Stroke Cerebrovasc. Dis. 25:e212–e213, 2016.
Regli, L., D. G. Piepgras, and K. K. Hansen. Late patency of long saphenous vein bypass grafts to the anterior and posterior cerebral circulation. J. Neurosurg. 83:806–811, 1995.
Sanai, N., Z. Zador, and M. T. Lawton. Bypass surgery for complex brain aneurysms: an assessment of intracranial-intracranial bypass. Neurosurgery. 65:670–683, 2009. (discussion 683)
Sekhar, L. N., S. D. Bucur, W. O. Bank, and D. C. Wright. Venous and arterial bypass grafts for difficult tumors, aneurysms, and occlusive vascular lesions: evolution of surgical treatment and improved graft results. Neurosurgery. 44:1207–1223, 1999. (discussion 1223-4)
Jafar, J. J., S. M. Russell, and H. H. Woo. Treatment of giant intracranial aneurysms with saphenous vein extracranial-to-intracranial bypass grafting: indications, operative technique, and results in 29 patients. Neurosurgery. 51:138–144, 2002. (discussion 144-6)
Ishishita, Y., R. Tanikawa, K. Noda, H. Kubota, N. Izumi, M. Katsuno, N. Ota, T. Miyazaki, M. Hashimoto, T. Kimura, and A. Morita. Universal extracranial-intracranial graft bypass for large or giant internal carotid aneurysms: techniques and results in 38 consecutive patients. World Neurosurg. 82:130–139, 2014.
Spetzler, R. F., H. Schuster, and R. A. Roski. Elective extracranial-intracranial arterial bypass in the treatment of inoperable giant aneurysms of the internal carotid artery. J. Neurosurg. 53:22–27, 1980.
Sekhar, L. N., J. M. Duff, C. Kalavakonda, and M. Olding. Cerebral revascularization using radial artery grafts for the treatment of complex intracranial aneurysms: techniques and outcomes for 17 patients. Neurosurgery. 49:646–658, 2001. (discussion 658-9)
Dazeo, N., R. Muñoz, A. P. Narata, H. Fernandez, and I. Larrabide. Intra-saccular device modeling for treatment planning of intracranial aneurysms: from morphology to hemodynamics. Int. J. Comput. Assist. Radiol. Surg. 16:1663–1673, 2021.
Razaghi, R., H. Biglari, and A. Karimi. Risk of rupture of the cerebral aneurysm in relation to traumatic brain injury using a patient-specific fluid-structure interaction model. Comput. Methods Progr. Biomed. 176:9–16, 2019.
Volokh, K. Y. Prediction of arterial failure based on a microstructural bi-layer fiber-matrix model with softening. J. Biomech. 41:447–453, 2008.
Lee, C. J., Y. Zhang, H. Takao, Y. Murayama, and Y. Qian. A fluid-structure interaction study using patient-specific ruptured and unruptured aneurysm: the effect of aneurysm morphology, hypertension and elasticity. J. Biomech. 46:2402–2410, 2013.
Isaksen, J. G., Y. Bazilevs, T. Kvamsdal, Y. Zhang, J. H. Kaspersen, K. Waterloo, B. Romner, and T. Ingebrigtsen. Determination of wall tension in cerebral artery aneurysms by numerical simulation. Stroke. 39:3172–3178, 2008.
Torii, R., M. Oshima, T. Kobayashi, K. Takagi, Tezduyar TEJCM. Fluid–structure interaction modeling of aneurysmal conditions with high and normal blood pressures. Comput. Mech. 38:482–490, 2006.
Sun, H. T., K. Y. Sze, A. Y. S. Tang, A. C. O. Tsang, A. C. H. Yu, and K. W. Chow. Effects of aspect ratio, wall thickness and hypertension in the patient-specific computational modeling of cerebral aneurysms using fluid-structure interaction analysis. En. Appl. Comput. Fluid Mech. 13(1):229–244, 2019.
Russell, J. H., N. Kelson, M. Barry, M. Pearcy, D. F. Fletcher, and C. D. Winter. Computational fluid dynamic analysis of intracranial aneurysmal bleb formation. Neurosurgery. 73:1061–1068, 2013.
Huang, Z., M. Zeng, W. G. Tao, F. Y. Zeng, C. Q. Chen, L. B. Zhang, and F. H. Chen. A hemodynamic mechanism correlating with the initiation of MCA bifurcation aneurysms. AJNR Am. J. Neuroradiol. 41:1217–1224, 2020.
Ford, M. D., N. Alperin, S. H. Lee, D. W. Holdsworth, and D. A. Steinman. Characterization of volumetric flow rate waveforms in the normal internal carotid and vertebral arteries. Physiol. Meas. 26:477–488, 2005.
Costalat, V., M. Sanchez, D. Ambard, L. Thines, N. Lonjon, F. Nicoud, H. Brunel, J. P. Lejeune, H. Dufour, P. Bouillot, J. P. Lhaldky, K. Kouri, F. Segnarbieux, C. A. Maurage, K. Lobotesis, M. C. Villa-Uriol, C. Zhang, A. F. Frangi, G. Mercier, A. Bonafé, L. Sarry, and F. Jourdan. Biomechanical wall properties of human intracranial aneurysms resected following surgical clipping (IRRAs Project). J. Biomech. 44:2685–2691, 2011.
Long, Y., H. Yu, Z. Zhuo, Y. Zhang, Y. Wang, X. Yang, and H. Li. A geometric scaling model for assessing the impact of aneurysm size ratio on hemodynamic characteristics. Biomed. Eng. 13:17, 2014.
Himburg, H. A., D. M. Grzybowski, A. L. Hazel, J. A. LaMack, X. M. Li, and M. H. Friedman. Spatial comparison between wall shear stress measures and porcine arterial endothelial permeability. Am. J. Physiol. Heart Circ. Physiol. 286:H1916–H1922, 2004.
Lawton, M. T., M. G. Hamilton, J. J. Morcos, and R. F. Spetzler. Revascularization and aneurysm surgery: current techniques, indications, and outcome. Neurosurgery. 38:83–92, 1996. (discussion 92-4)
Thines, L., F. Proust, P. Marinho, A. Durand, A. van der Zwan, L. Regli, and J. P. Lejeune. Giant and complex aneurysms treatment with preservation of flow via bypass technique. Neuro-Chirurgie. 62:1–13, 2016.
Sorimachi, T., T. Osada, A. Hirayama, H. Shigematsu, K. Srivatanakul, and M. Matsumae. Preservation of anterior choroidal artery blood flow during trapping of the internal carotid artery for a ruptured blood blister-like aneurysm with high-flow bypass. World Neurosurg. 122:e847–e855, 2019.
Parkinson, R. J., C. S. Eddleman, H. H. Batjer, and B. R. Bendok. Giant intracranial aneurysms: endovascular challenges. Neurosurgery. 59:S103–S112, 2006. (discussion S3-13)
Haque, R., C. Kellner, and R. A. Solomon. Spontaneous thrombosis of a giant fusiform aneurysm following extracranial-intracranial bypass surgery. J. Neurosurg. 110:469–474, 2009.
Cantore, G., A. Santoro, and R. Da Pian. Spontaneous occlusion of supraclinoid aneurysms after the creation of extra-intracranial bypasses using long grafts: report of two cases. Neurosurgery. 44:216–219, 1999. (discussion 219-20)
Possati, G., M. Gaudino, F. Alessandrini, N. Luciani, F. Glieca, C. Trani, C. Cellini, C. Canosa, and G. Di Sciascio. Midterm clinical and angiographic results of radial artery grafts used for myocardial revascularization. J. Thorac. Cardiovasc. Surg. 116:1015–1021, 1998.
Bols, J., J. Degroote, B. Trachet, B. Verhegghe, P. Segers, and J. Vierendeels. A computational method to assess the in vivo stresses and unloaded configuration of patient-specific blood vessels. J. Comput. Appl. Math. 246:10–17, 2013.
Cebral, J. R., X. Duan, P. S. Gade, B. J. Chung, F. Mut, K. Aziz, and A. M. Robertson. Regional mapping of flow and wall characteristics of intracranial aneurysms. Ann. Biomed. Eng. 44:3553–3567, 2016.
Cho, K. C., H. Yang, J. J. Kim, J. H. Oh, and Y. B. Kim. Prediction of rupture risk in cerebral aneurysms by comparing clinical cases with fluid-structure interaction analyses. Sci. Rep. 10:18237, 2020.
Voß, S., Glaßer, S., Hoffmann, T., Beuing, O., Weigand, S., Jachau, K., Preim, B., Thévenin, D., Janiga. G., Berg, P.J.C. and medicine mmi. Fluid-structure simulations of a ruptured intracranial aneurysm: constant versus patient-specific wall thickness. 2016;2016.
Shamloo, A., M. A. Nejad, and M. Saeedi. Fluid-structure interaction simulation of a cerebral aneurysm: effects of endovascular coiling treatment and aneurysm wall thickening. J. Mech. Behav. Biomed. Mater. 74:72–83, 2017.
Cebral, J. R., X. Duan, B. J. Chung, C. Putman, K. Aziz, and A. M. Robertson. Wall mechanical properties and hemodynamics of unruptured intracranial aneurysms. AJNR Am. J. Neuroradiol. 36:1695–1703, 2015.
Acknowledgement
Not applicable
Funding
The authors received no financial support for the research authorship and/or publication of this article.
Author information
Authors and Affiliations
Contributions
SL: made substantial contributions to the conception, design, analysis, and interpretation of data, and has drafted the manuscript. SL: made contributions to the design of the work and revision of the manuscript. SL and ZH: made contributions to the acquisition of data. HC & FC: the corresponding author, made contributions to the conception and interpretation of data and has determined the final version to be submitted for publishing. SL, ZH, HC, FC read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that they have no competing interests.
Ethical Approval
This study was approved by the Ethics Committee of Xiangya Hospital.
Consent to Participate
Informed consent was obtained from all individual participants or their guardians.
Consent for Publication
All authors approved this publication.
Additional information
Associate Editor Jamshid Karimov, MD, PhD oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, S., Huang, Z., Chen, H. et al. Proximal Clipping and Distal High-Flow Bypass in the Treatment of Giant/Complex Intracranial Aneurysm: An Opportunity or a Risk from a Fluid-Structural Interaction Analysis. Cardiovasc Eng Tech (2023). https://doi.org/10.1007/s13239-023-00704-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13239-023-00704-z