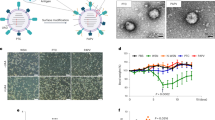
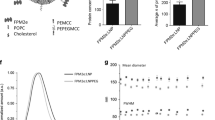
Abstract
KRAS mutations occur commonly in the lung and can lead to the development of non-small cell lung cancer (NSCLC). While the mutated KRAS protein is a neoantigen, it usually does not generate an effective anti-tumor immune response on mucosal/epithelial surfaces. Despite this, mutated KRAS remains a potential target for immunotherapy since immune targeting of this protein in animal models has been effective at eliminating tumor cells. We attempted to develop a KRAS vaccine using mutated and wild-type KRAS peptides in combination with a nanoemulsion (NE) adjuvant. The efficacy of this approach was tested in an inducible mutant KRAS-mouse lung tumor model. Animals were immunized intranasally using NE with KRAS peptides. These animals had decreased CD4+FoxP3+ T cells in both lymph nodes and spleen. Immunized animals also showed higher IFN-γ and IL-17a levels to mutated KRAS that were produced by CD8+ T cells and enhancement in KRAS-specific Th1 and Th17 responses that persisted for 3 months after the last vaccination. Importantly, the immunized animals had significantly decreased tumor incidence compared to control animals. In conclusion, a mucosal approach to KRAS vaccination demonstrated the ability to induce local KRAS-specific immune responses in the lung and resulted in reduced tumor incidence.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
Data are contained within the article.
References
Cekani E, Epistolio S, Dazio G, Cefalì M, Wannesson L, Frattini M, et al. Molecular biology and therapeutic perspectives for K-Ras mutant non-small cell lung cancers. Cancers. 2022;14:4103.
Ning W, Marti TM, Dorn P, Peng RW. Non-genetic adaptive resistance to KRASG12C inhibition: EMT is not the only culprit. Front Oncol. 2022;12:1004669.
Tu G, Liu Q, Qiu Y, Leung EL, Yao X. In silico study of the acquired resistance caused by the secondary mutations of KRAS G12C protein using long time molecular dynamics simulation and Markov state model analysis. Int J Mol Sci. 2022;23:13845.
Kemp SB, Cheng N, Markosyan N, Sor R, Kim IK, Hallin J, et al. Efficacy of a small molecule inhibitor of KrasG12D in immunocompetent models of pancreatic cancer. Cancer Discov. 2022;13:298–311.
Hallin J, Bowcut V, Calinisan A, Briere DM, Hargis L, Engstrom LD, et al. Anti-tumor efficacy of a potent and selective non-covalent KRASG12D inhibitor. Nat Med. 2022;28:2171–82.
Bannoura SF, Khan HY, Azmi AS. KRAS G12D targeted therapies for pancreatic cancer: has the fortress been conquered? Front Oncol. 2022;12:1013902.
Mizuno T, Katsuya Y, Sato J, Koyama T, Shimizu T, Yamamoto N. Emerging PD-1/PD-L1 targeting immunotherapy in non-small cell lung cancer: current status and future perspective in Japan, US, EU, and China. Front Oncol. 2022;12:925938.
Quan Z, Yang Y, Zheng H, Zhan Y, Luo J, Ning Y, et al. Clinical implications of the interaction between PD-1/PD-L1 and PI3K/AKT/mTOR pathway in progression and treatment of non-small cell lung cancer. J Cancer. 2022;13:3434–43.
Liu C, Zheng S, Wang Z, Wang S, Wang X, Yang L, et al. KRAS-G12D mutation drives immune suppression and the primary resistance of anti-PD-1/PD-L1 immunotherapy in non-small cell lung cancer. Cancer Commun. 2022;42:828–47.
Della Corte CM, Byers LA. Evading the STING: LKB1 loss leads to STING silencing and immune escape in KRAS-mutant lung cancers. Cancer Discov. 2019;9:16–8.
van Maldegem F, Downward J. Mutant KRAS at the heart of tumor immune evasion. Immunity. 2020;52:14–6.
Hamarsheh S, Groß O, Brummer T, Zeiser R. Immune modulatory effects of oncogenic KRAS in cancer. Nat Commun. 2020;11:5439.
Wang SH, Chen J, Smith D, Cao Z, Acosta H, Fan Y, et al. A novel combination of intramuscular vaccine adjuvants, nanoemulsion and CpG produces an effective immune response against influenza A virus. Vaccine. 2020;38:3537–44.
Wang SH, Smith D, Cao Z, Chen J, Acosta H, Chichester JA, et al. Recombinant H5 hemagglutinin adjuvanted with nanoemulsion protects ferrets against pathogenic avian influenza virus challenge. Vaccine. 2019;37:1591–600.
Cao Z, Spilker T, Fan Y, Kalikin LM, Ciotti S, LiPuma JJ, et al. Nanoemulsion is an effective antimicrobial for methicillin-resistant Staphylococcus aureus in infected wounds. Nanomedicine. 2017;12:1177–85.
Wong PT, Wang SH, Ciotti S, Makidon PE, Smith DM, Fan Y, et al. Formulation and characterization of nanoemulsion intranasal adjuvants: effects of surfactant composition on mucoadhesion and immunogenicity. Mol Pharm. 2014;11:531–44.
Guéry L, Hugues S. Th17 cell plasticity and functions in cancer immunity. Biomed Res Int. 2015;2015:314620–11.
Majchrzak K, Nelson MH, Bailey SR, Bowers JS, Yu XZ, Rubinstein MP, et al. Exploiting IL-17-producing CD4+ and CD8+ T cells to improve cancer immunotherapy in the clinic. Cancer Immunol Immunother. 2016;65:247–59.
Pan J, Zhang Q, Sei S, Shoemaker RH, Lubet RA, Wang Y, et al. Immunoprevention of KRAS-driven lung adenocarcinoma by a multipeptide vaccine. Oncotarget. 2017;8:82689–99.
Chung WJ, Daemen A, Cheng JH, Long JE, Cooper JE, Wang BE, et al. Kras mutant genetically engineered mouse models of human cancers are genomically heterogeneous. Proc Natl Acad Sci USA. 2017;114:E10947–55.
Tan YS, Lei YL. Isolation of tumor-infiltrating lymphocytes by Ficoll-Paque density gradient centrifugation. Methods Mol Biol. 2019;1960:93–9.
Li YM, Yu JM, Liu ZY, Yang HJ, Tang J, Chen ZN. Programmed death ligand 1 indicates pre-existing adaptive immune response by tumor-infiltrating CD8+ T cells in non-small cell lung cancer. Int J Mol Sci. 2019;20:5138.
Song L, Ma S, Chen L, Miao L, Tao M, Liu H. Long-term prognostic significance of interleukin-17-producing T cells in patients with non-small cell lung cancer. Cancer Sci. 2019;110:2100–9.
Leem G, Jeon M, Kim KW, Jeong S, Choi SJ, Lee YJ, et al. Tumour-infiltrating bystander CD8+ T cells activated by IL-15 contribute to tumour control in non-small cell lung cancer. Thorax. 2022;77:769–80.
Chen SW, Zhu SQ, Pei X, Qiu BQ, Xiong D, Long X, et al. Cancer cell-derived exosomal circUSP7 induces CD8+ T cell dysfunction and anti-PD1 resistance by regulating the miR-934/SHP2 axis in NSCLC. Mol Cancer. 2021;20:144.
Amado RG, Wolf M, Peeters M, Van Cutsem E, Siena S, Freeman DJ, et al. Wild-type KRAS is required for panitumumab efficacy in patients with metastatic colorectal cancer. J Clin Oncol. 2008;26:1626–34.
Cuzzubbo S, Mangsbo S, Nagarajan D, Habra K, Pockley AG, McArdle SEB. Cancer vaccines: adjuvant potency, importance of age, lifestyle, and treatments. Front Immunol. 2021;11:615240.
Asimgil H, Ertetik U, Çevik NC, Ekizce M, Doğruöz A, Gökalp M, et al. Targeting the undruggable oncogenic KRAS: the dawn of hope. JCI Insight. 2022;7:e153688.
Weng TY, Yen MC, Huang CT, Hung JJ, Chen YL, Chen WC, et al. DNA vaccine elicits an efficient antitumor response by targeting the mutant Kras in a transgenic mouse lung cancer model. Gene Ther. 2014;21:888–96.
Chaft JE, Litvak A, Arcila ME, Patel P, D’Angelo SP, Krug LM, et al. Phase II study of the GI-4000 KRAS vaccine after curative therapy in patients with stage I-III lung adenocarcinoma harboring a KRAS G12C, G12D, or G12V mutation. Clin Lung Cancer. 2014;15:405–10.
Lopes A, Vandermeulen G, Préat V. Cancer DNA vaccines: current preclinical and clinical developments and future perspectives. J Exp Clin Cancer Res. 2019;38:146.
Muscarella P, Bekaii-Saab T, McIntyre K, Rosemurgy A, Ross SB, Richards DA, et al. A phase 2 randomized placebo-controlled adjuvant trial of GI-4000, a recombinant yeast expressing mutated RAS proteins in patients with resected pancreas cancer. J Pancreat Cancer. 2021;7:8–19.
Frafjord A, Buer L, Hammarström C, Aamodt H, Woldbæk PR, Brustugun OT, et al. The immune landscape of human primary lung tumors is Th2 skewed. Front Immunol. 2021;12:764596.
Acknowledgements
This study was supported by the Development Therapy Fund from Rogel Cancer Center, University of Michigan, and Michigan Nanotechnology Institute for Medicine & Biological Sciences.
Funding
This study was supported by the Development Therapy Fund from Rogel Cancer Center, University of Michigan, and Michigan Nanotechnology Institute for Medicine & Biological Sciences.
Author information
Authors and Affiliations
Contributions
SHW and JRB were responsible for designing the methodology and writing the manuscript. SHW, ZC, FM and JC were responsible for the investigation. KW, ST and JCH were responsible for data collection and analysis. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
Animal use protocols were approved by the University of Michigan Institutional Animal Care and Use Committee (IACUC).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, S.H., Cao, Z., Farazuddin, M. et al. A novel intranasal peptide vaccine inhibits non-small cell lung cancer with KRAS mutation. Cancer Gene Ther 31, 464–471 (2024). https://doi.org/10.1038/s41417-023-00717-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41417-023-00717-9