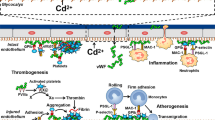
Abstract
Human exposure to environmental arsenic induces cardiovascular diseases such as arrhythmias, hypertension, and arteriosclerosis. Here, we review the toxicological and cardiovascular impacts of arsenic in in vitro cardiac and vascular models. The mechanism of arsenic-induced cardiovascular impairments includes oxidative stress, epigenetic modifications, chromatin instability, subcellular damage, and premature aging. The different types of cardiac and vascular cells exhibit distinct responses to arsenic exposure. Arsenic causes arrhythmias, which involve alteration of cardiomyocyte potassium channels and, in turn, repolarization issues. This is mainly due to redox signals that cause epigenetic modifications of potassium channels. On the other hand, vascular lesions, such as damage to blood vessels, occur mainly due to an imbalance in redox levels. This imbalance leads to premature senescence of cells and stop the cell cycle. Furthermore, intracellular accumulation of calcium and ferrous ions plays a major role in arsenic-induced vascular cell apoptosis and cardiomyocyte ferroptosis, respectively.






Similar content being viewed by others
Availability of data and materials
All data and materials supporting this review can be approached from public domain that comply with field standards, and no materials need to be made available from our side.
Code availability
Not applicable.
Abbreviations
- AT1R:
-
Angiotensin II type I receptor
- As3MT:
-
Arsenite methyltransferase
- CDC2:
-
Cell division control 2
- DSBs:
-
DNA double-strand breaks
- FasL:
-
Factor-associated suicide ligand
- hERG:
-
Human ether-a-go-go-related gene
- HUVECs:
-
Human umbilical vein endothelial cells
- IK1 :
-
Inward rectifier potassium current
- MMAIII :
-
Monomethylarsonous acid
- Nrf2:
-
Nuclear factor erythroid-2-related factor 2
- KCNJ2:
-
Potassium inwardly rectifying channel subfamily J member 2
- KCNE1:
-
Potassium voltage-gated channel subfamily E regulatory subunit 1
- KCNH2:
-
Potassium voltage-gated channel subfamily H member 2
- KCNQ1:
-
Potassium voltage-gated channel subfamily Q member 1
- IKr :
-
Rapidly activating delayed rectifier potassium current
- ROS:
-
Reactive oxygen species
- NADPH:
-
Reduced nicotinamide adenine dinucleotide phosphate
- SA-β-Gal:
-
Senescence β-galactosidase
- IKs :
-
Slowly activating delayed rectifying potassium current
- VECs:
-
Vascular endothelial cells
- VSMCs:
-
Vascular smooth muscle cells
References
Allison P, Huang T, Broka D, Parker P, Barnett JV, Camenisch TD (2013) Disruption of canonical TGFbeta-signaling in murine coronary progenitor cells by low level arsenic. Toxicol Appl Pharmacol 272:147–153. https://doi.org/10.1016/j.taap.2013.04.035
Balarastaghi S, Rezaee R, Hayes AW, Yarmohammadi F, Karimi G (2023) Mechanisms of arsenic exposure-induced hypertension and atherosclerosis: an updated overview. Biol Trace Elem Res 201:98–113. https://doi.org/10.1007/s12011-022-03153-2
Bao LZ, Shi HL (2010) Arsenite induces endothelial cell permeability increase through a reactive oxygen species-vascular endothelial growth factor pathway. Chem Res Toxicol 23:1726–1734. https://doi.org/10.1021/tx100191t
Bao ZY, Han ZB, Zhang B, Yu Y, Xu ZH, Ma WY, Ding FZ, Zhang L, Yu MX, Liu SZ, Jin MY, Yan GG, Huang Q, Wang XX, Hua BJ, Yang F, Li Y, Liu Y, Zagidullin N, Carvalho K, Li BX, Wang N, Cai BZ (2019) Arsenic trioxide blocked proliferation and cardiomyocyte differentiation of human induced pluripotent stem cells: implication in cardiac developmental toxicity. Toxicol Lett 309:51–58. https://doi.org/10.1016/j.toxlet.2019.03.008
Berry LD, Gould KL (1996) Regulation of Cdc2 activity by phosphorylation at T14/Y15. Prog Cell Cycle Res 2:99–105. https://doi.org/10.1007/978-1-4615-5873-6_10
Bessho M, Aki T, Funakoshi T, Unuma K, Noritake K, Kato C, Uemura K (2013) Rho-kinase inhibitor Y-27632 attenuates arsenic trioxide toxicity in H9c2 cardiomyoblastoma cells. Cardiovasc Toxicol 13:267–277. https://doi.org/10.1007/s12012-013-9206-2
Brown RA, Shantsila E, Varma C, Lip GYH (2017) Current understanding of atherogenesis. Am J Med 130:268–282. https://doi.org/10.1016/j.amjmed.2016.10.022
Bunderson M, Coffin JD, Beall HD (2002) Arsenic induces peroxynitrite generation and cyclooxygenase-2 protein expression in aortic endothelial cells: possible role in atherosclerosis. Toxicol Appl Pharmacol 184:11–18. https://doi.org/10.1006/taap.2002.9492
Cai ZH, Zhang YQ, Zhang YT, Miao XF, Li S, Yang H, Ling QJ, Hoffmann PR, Huang Z (2019) Use of a mouse model and human umbilical vein endothelial cells to investigate the effect of arsenic exposure on vascular endothelial function and the associated role of Calpains. Environ Health Persp 127:77003. https://doi.org/10.1289/EHP4538
Celik I, Gallicchio L, Boyd K, Lam TK, Matanoski G, Tao XG, Shiels M, Hammond E, Chen LW, Robinson KA, Caulfield LE, Herman JG, Guallar E, Alberg AJ (2008) Arsenic in drinking water and lung cancer: a systematic review. Environ Res 108:48–55. https://doi.org/10.1016/j.envres.2008.04.001
Chao JI, Hsu SH, Tsou TC (2006) Depletion of securin increases arsenite-induced chromosome instability and apoptosis via a p53-independent pathway. Toxicol Sci 90:73–86. https://doi.org/10.1093/toxsci/kfj070
Chen Y, Dorn GW 2nd (2013) PINK1-phosphorylated mitofusin 2 is a Parkin receptor for culling damaged mitochondria. Science 340:471–475. https://doi.org/10.1126/science.1231031
Chen XC, Shan HL, Zhao JL, Hong Y, Bai YL, Sun IH, Pan ZW, Zhang Y, Yang BF, Du ZM (2010) L-type calcium current (ICa, L) and inward rectifier potassium current (IK1) are involved in QT prolongation induced by arsenic trioxide in rat. Cell Physiol Biochem 26:967–974. https://doi.org/10.1159/000324005
Chen XX, Jiang YJ, Zeng T, Li JJ (2020) Overexpression of the long noncoding RNA NEAT1 protects against As2O3-induced injury of cardiomyocyte by inhibiting the miR-124/NF-κB signaling pathway. Eur Rev Med Pharmacol Sci 24:1378–1390. https://doi.org/10.26355/eurrev_202002_20195
Cheng YH, Ou BR, Cheng LC, Lu JH, Yeh JY (2008) Glutathione regulation in arsenic-induced porcine aortic endothelial cells. Toxicol in Vitro 22:1832–1839. https://doi.org/10.1016/j.tiv.2008.08.006
Chu WF, Li C, Qu XF, Zhao D, Wang XL, Yu XR, Cai FL, Liang HH, Zhang Y, Zhao X, Li BX, Qiao GF, Dong DL, Lu YJ, Du ZM, Yang BF (2012) Arsenic-induced interstitial myocardial fibrosis reveals a new insight into drug-induced long QT syndrome. Cardiovasc Res 96:90–98. https://doi.org/10.1093/cvr/cvs230
Cui YX, Dong L, Zhang M, Liu YN, Chen YH, Jia MZ, Chen KP, Wang H, Shi YW, Ma TY, Chen JH (2023) Long-term exposure to arsenic in drinking water leads to myocardial damage by oxidative stress and reduction in NO. Toxicology 492:153529. https://doi.org/10.1016/j.tox.2023.153529
Cui Y, Han Z, Hu Y, Song G, Hao C, Xia H, Ma X (2012) MicroRNA-181b and microRNA-9 mediate arsenic-induced angiogenesis via NRP1. J Cell Physiol 227:772–783. https://doi.org/10.1002/jcp.22789
Demer LL, Tintut Y (2014) Inflammatory, metabolic, and genetic mechanisms of vascular calcification. Arterioscler Thromb Vasc Biol 34:715–723. https://doi.org/10.1161/ATVBAHA.113.302070
D’Ippoliti D, Santelli E, De Sario M, Scortichini M, Davoli M, Michelozzi P (2015) Arsenic in drinking water and mortality for cancer and chronic diseases in central Italy, 1990–2010. PLoS ONE 10:e0138182. https://doi.org/10.1371/journal.pone.0138182
Dodmane PR, Arnold LL, Pennington KL, Singh RK, Cardoso APF, Cohen SM (2015) Effect of trivalent arsenicals on cell proliferation in mouse and human microvascular endothelial cells. Toxicol Rep 2:833–837. https://doi.org/10.1016/j.toxrep.2015.05.009
Domingo-Relloso A, Makhani K, Riffo-Campos AL, Tellez-Plaza M, Klein KO, Subedi P, Zhao JY, Moon KA, Bozack AK, Haack K, Goessler W, Umans JG, Best LG, Zhang Y, Herreros-Martinez M, Glabonjat RA, Schilling K, Galvez-Fernandez M, Kent JW Jr, Sanchez TR, Taylor KD, Johnson WC, Durda P, Tracy RP, Rotter JI, Rich SS, Berg DVD, Kasela S, Lappalainen T, Vasan RS, Joehanes R, Howard BV, Levy D, Lohman K, Liu YM, Fallin MD, Cole SA, Mann KK, Navas-Acien A (2022) Arsenic exposure, blood DNA methylation, and cardiovascular disease. Circ Res 131:e51–e69. https://doi.org/10.1161/CIRCRESAHA.122.320991
Dutta M, Ghosh D, Ghosh AK, Bose G, Chattopadhyay A, Rudra S, Dey M, Bandyopadhyay A, Pattari SK, Mallick S, Bandyopadhyay D (2014) High fat diet aggravates arsenic induced oxidative stress in rat heart and liver. Food Chem Toxicol 66:262–277. https://doi.org/10.1016/j.fct.2014.01.050
Fan L, Zhang Y, Shi D, Xi R, Zhang Z, Wang X (2021) Hypoxia enhances the cytotoxic effect of As4S4 on rat ventricular H9c2 cells through activation of ubiquitin-proteasome system. J Trace Elem Med Biol 66:126720. https://doi.org/10.1016/j.jtemb.2021.126720
Farzan SF, Howe CG, Zens MS, Palys T, Channon JY, Li ZG, Chen Y, Karagas MR (2017) Urine arsenic and arsenic metabolites in U.S. adults and biomarkers of inflammation, oxidative stress, and endothelial dysfunction: a cross-sectional study. Environ Health Perspect 125:127002. https://doi.org/10.1289/EHP2062
Feng XN, Liu QY, Wang S, Cen L, Li HP (2021) Arsenopyrite weathering in acid rain: arsenic transfer and environmental implications. J Hazard Mater 420:126612. https://doi.org/10.1016/j.jhazmat.2021.126612
Fujiwara Y, Yamamoto C, Hirooka T, Terada N, Satoh M, Kaji T (2008) Arsenite but not arsenate inhibits general proteoglycan synthesis in cultured arterial smooth muscle cells. J Toxicol Sci 33:487–492. https://doi.org/10.2131/jts.33.487
Geisler S, Holmstrom KM, Skujat D, Fiesel FC, Rothfuss OC, Kahle PJ, Springer W (2010) PINK1/Parkin-mediated mitophagy is dependent on VDAC1 and p62/SQSTM1. Nat Cell Biol 12:119-U70. https://doi.org/10.1038/ncb2012
Gribble MO, Tang WY, Shang Y, Pollak J, Umans JG, Francesconi KA, Goessler W, Silbergeld EK, Guallar E, Cole SA, Fallin MD, Navas-Acien A (2014) Differential methylation of the arsenic(III) methyltransferase promoter according to arsenic exposure. Arch Toxicol 88:275–282. https://doi.org/10.1007/s00204-013-1146-x
Grunnet M, Hansen RS, Olesen SP (2008) hERG1 channel activators: a new anti-arrhythmic principle. Prog Biophys Mol Biol 98:347–62. https://doi.org/10.1016/j.pbiomolbio.2009.01.002
Guo XN, Liu XN, Wang JQ, Fu XY, Yao JY, Zhang XD, Jackson S, Li JY, Zhang W, Sun DJ (2020) Pigment epithelium-derived factor (PEDF) ameliorates arsenic-induced vascular endothelial dysfunction in rats and toxicity in endothelial EA.hy926 cells. Environ Res 186:109506. https://doi.org/10.1016/j.envres.2020.109506
Hackethal C, Kopp JF, Sarvan I, Schwerdtle T, Lindtner O (2021) Total arsenic and water-soluble arsenic species in foods of the first German total diet study (BfR MEAL study). Food Chem 346:128913. https://doi.org/10.1016/j.foodchem.2020.128913
Halatek T, Sinczuk-Walczak H, Rabieh S, Wasowicz W (2009) Association between occupational exposure to arsenic and neurological, respiratory and renal effects. Toxicol Appl Pharm 239:193–199. https://doi.org/10.1016/j.taap.2009.04.022
Hirano S, Cui X, Li S, Kanno S, Kobayashi Y, Hayakawa T, Shraim A (2003) Difference in uptake and toxicity of trivalent and pentavalent inorganic arsenic in rat heart microvessel endothelial cells. Arch Toxicol 77:305–312. https://doi.org/10.1007/s00204-003-0447-x
Hirano S, Kobayashi Y, Hayakawa T, Cui X, Yamamoto M, Kanno S, Shraim A (2005) Accumulation and toxicity of monophenyl arsenicals in rat endothelial cells. Arch Toxicol 79:54–61. https://doi.org/10.1007/s00204-004-0598-4
Hofer E, Schweighofer B (2007) Signal transduction induced in endothelial cells by growth factor receptors involved in angiogenesis. Thromb Haemost 97:355–363. https://doi.org/10.1160/th06-08-0470
Hossain E, Ota A, Takahashi M, Karnan S, Damdindorj L, Konishi Y, Konishi H, Hosokawa Y (2013) Arsenic upregulates the expression of angiotensin II Type I receptor in mouse aortic endothelial cells. Toxicol Lett 220:70–75. https://doi.org/10.1016/j.toxlet.2013.04.006
Hu B, Zhu XL, Fan QX, Li HX, Zou CW (2012) Experimental study on inhibition of rat ventricular Ik1 by RNA interference targeting the KCNJ2 gene. Biosci Trends 6:26–32. https://doi.org/10.5582/bst.2012.v6.1.26
Huang Z, Hoffmann FW, Norton RL, Hashimoto AC, Hoffmann PR (2011) Selenoprotein K is a novel target of m-Calpain, and cleavage is regulated by toll-like receptor-induced calpastatin in macrophages. J Biol Chem 286:34830–34838. https://doi.org/10.1074/jbc.M111.265520
Huang T, Barnett JV, Camenisch TD (2014) Cardiac epithelial-mesenchymal transition is blocked by monomethylarsonous acid(III). Toxicol Sci 142:225–38. https://doi.org/10.1093/toxsci/kfu170
Huang T, Ditzel EJ, Perrera AB, Broka DM, Camenisch TD (2015) Arsenite disrupts zinc-dependent TGFbeta2-SMAD activity during murine cardiac progenitor cell differentiation. Toxicol Sci 148:409–420. https://doi.org/10.1093/toxsci/kfv191
Hubaux R, Becker-Santos DD, Enfield KS, Rowbotham D, Lam S, Lam WL, Martinez VD (2013) Molecular features in arsenic-induced lung tumors. Mol Cancer 12:20. https://doi.org/10.1186/1476-4598-12-20
Hunyady L, Catt KJ (2006) Pleiotropic AT1 receptor signaling pathways mediating physiological and pathogenic actions of angiotensin II. Mol Endocrinol 20:953–970. https://doi.org/10.1210/me.2004-0536
Huq ME, Fahad S, Shao ZF, Sarven MS, Khan IA, Alam M, Saeed M, Ullah H, Adnan M, Saud S, Cheng QM, Ali S, Wahid F, Zamin M, Raza MA, Saeed B, Riaz M, Khan WU (2020) Arsenic in a groundwater environment in Bangladesh: occurrence and mobilization. J Environ Manage 262:110318. https://doi.org/10.1016/j.jenvman.2020.110318
Hussain MM, Wang JX, Bibi I, Shahid M, Niazi NK, Iqbal J, Mian IA, Shaheen SM, Bashir S, Shah NS, Hina K, Rinklebe J (2021) Arsenic speciation and biotransformation pathways in the aquatic ecosystem: the significance of algae. J Hazard Mater 403:124027. https://doi.org/10.1016/j.jhazmat.2020.124027
Islam S, Rahman MM, Islam MR, Naidu R (2016) Arsenic accumulation in rice: consequences of rice genotypes and management practices to reduce human health risk. Environ Int 96:139–155. https://doi.org/10.1016/j.envint.2016.09.006
Itoh K, Wakabayashi N, Katoh Y, Ishii T, Igarashi K, Engel JD, Yamamoto M (1999) Keap1 represses nuclear activation of antioxidant responsive elements by Nrf2 through binding to the amino-terminal Neh2 domain. Genes Dev 13:76–86. https://doi.org/10.1101/gad.13.1.76
Jiang YN, Du WJ, Chu Q, Qin Y, Tuguzbaeva G, Wang H, Li A, Li GY, Li YY, Chai L, Yue E, Sun X, Wang ZG, Pavlov V, Yang BF, Bai YL (2018) Downregulation of long non-coding RNA Kcnq1ot1: an important mechanism of arsenic trioxide-induced long QT syndrome. Cell Physiol Biochem 45:192–202. https://doi.org/10.1159/000486357
Jimi S, Uchiyama M, Takaki A, Suzumiya J, Hara S (2004) Mechanisms of cell death induced by cadmium and arsenic. Ann N Y Acad Sci 1011:325–331. https://doi.org/10.1007/978-3-662-41088-2_32
Jomova K, Jenisova Z, Feszterova M, Baros S, Liska J, Hudecova D, Rhodes CJ, Valko M (2011) Arsenic: toxicity, oxidative stress and human disease. J Appl Toxicol 31:95–107. https://doi.org/10.1002/jat.1649
Kala SV, Neely MW, Kala G, Prater CI, Atwood DW, Rice JS, Lieberman MW (2000) The MRP2/cMOAT transporter and arsenic–glutathione complex formation are required for biliary excretion of arsenic. J Biol Chem 275:33404–8. https://doi.org/10.1074/jbc.M007030200
Kao YH, Yu CL, Chang LW, Yu HS (2003) Low concentrations of arsenic induce vascular endothelial growth factor and nitric oxide release and stimulate angiogenesis in vitro. Chem Res Toxicol 16:460–468. https://doi.org/10.1021/tx025652a
Kapaj S, Peterson H, Liber K, Bhattacharya P (2006) Human health effects from chronic arsenic poisoning: a review. J Environ Sci Health A Tox Hazard Subst Environ Eng 41:2399–2428. https://doi.org/10.1080/10934520600873571
Khan I, Awan SA, Rizwan M, Ali S, Zhang XQ, Huang LK (2021) Arsenic behavior in soil-plant system and its detoxification mechanisms in plants: a review. Environ Pollut 286:117389. https://doi.org/10.1016/j.envpol.2021.117389
Kobayashi M, Li L, Iwamoto N, Nakajima-Takagi Y, Kaneko H, Nakayama Y, Eguchi M, Wada Y, Kumagai Y, Yamamoto M (2009) The antioxidant defense system Keap1-Nrf2 comprises a multiple sensing mechanism for responding to a wide range of chemical compounds. Mol Cell Biol 29:493–502. https://doi.org/10.1128/MCB.01080-08
Kunrath J, Gurzau E, Gurzau A, Goessler W, Gelmann ER, Thach TT, McCarty KM, Yeckel CW (2013) Blood pressure hyperreactivity: an early cardiovascular risk in normotensive men exposed to low-to-moderate inorganic arsenic in drinking water. J Hypertens 31:361–369. https://doi.org/10.1097/HJH.0b013e32835c175f
Lee PC, Ho IC, Lee TC (2005) Oxidative stress mediates sodium arsenite-induced expression of heme oxygenase-1, monocyte chemoattractant protein-1, and interleukin-6 in vascular smooth muscle cells. Toxicol Sci 85:541–550. https://doi.org/10.1093/toxsci/kfi101
Leslie EM, Haimeur A, Waalkes MP (2004) Arsenic transport by the human multidrug resistance protein 1 (MRP1/ABCC1). Evidence that a tri-glutathione conjugate is required. J Biol Chem 279:32700–8. https://doi.org/10.1074/jbc.M404912200
Li B, Sun Y, Sun X, Wang Y, Li X, Kumagai Y, Sun G (2007) Monomethylarsonous acid induced cytotoxicity and endothelial nitric oxide synthase phosphorylation in endothelial cells. Bull Environ Contam Toxicol 78:455–458. https://doi.org/10.1007/s00128-007-9178-7
Li JX, Shen YQ, Cai BZ, Zhao J, Bai XP, Lu YJ, Li XQ (2010) Arsenic trioxide induces the apoptosis in vascular smooth muscle cells via increasing intracellular calcium and ROS formation. Mol Biol Rep 37:1569–1576. https://doi.org/10.1007/s11033-009-9561-z
Li X, Shi Y, Wei Y, Ma X, Li Y, Li R (2012) Altered expression profiles of microRNAs upon arsenic exposure of human umbilical vein endothelial cells. Environ Toxicol Pharmacol 34:381–387. https://doi.org/10.1016/j.etap.2012.05.003
Li C, Qu XF, Xu WX, Qu N, Mei L, Liu Y, Wang XL, Yu XR, Liu ZY, Nie D, Liu Y, Yan JL, Yang BF, Lu YJ, Chu WF (2013) Arsenic trioxide induces cardiac fibroblast apoptosis in vitro and in vivo by up-regulating TGF-β1 expression. Toxicol Lett 219:223–230. https://doi.org/10.1016/j.toxlet.2013.03.024
Li YN, Xi MM, Guo Y, Hai CX, Yang WL, Qin XJ (2014) NADPH oxidase-mitochondria axis-derived ROS mediate arsenite-induced HIF-1alpha stabilization by inhibiting prolyl hydroxylases activity. Toxicol Lett 224:165–174. https://doi.org/10.1016/j.toxlet.2013.10.029
Li JL, Duan XX, Dong DD, Zhang Y, Li W, Zhao L, Nie HF, Sun GF, Li B (2015) Hepatic and nephric NRF2 pathway up-regulation, an early antioxidant response, in acute arsenic-exposed mice. Int J Environ Res Public Health 12:12628–12642. https://doi.org/10.3390/ijerph121012628
Li MN, Qian M, Kyler K, Xu J (2018) Endothelial-vascular smooth muscle cells interactions in atherosclerosis. Front Cardiovasc Med 5:151. https://doi.org/10.3389/fcvm.2018.00151
Liang X, Wu T, Wang Y, Wei T, Zou L, Bai C, Liu N, Zhang T, Xue Y, Tang M (2020) CdTe and CdTe@ZnS quantum dots induce IL-1ß-mediated inflammation and pyroptosis in microglia. Toxicol in Vitro 65:104827. https://doi.org/10.1016/j.tiv.2020.104827
Liao PJ, Hsu KH, Chiou HY, Chen CJ, Lee CH (2021) Joint effects of genomic markers and urinary methylation capacity associated with inorganic arsenic metabolism on the occurrence of cancers among residents in arseniasis-endemic areas: a cohort subset with average fifteen-year follow-up. Biomed J 44:S218–S225. https://doi.org/10.1016/j.bj.2020.10.005
Lind L, Araujo JA, Barchowsky A, Belcher S, Berridge BR, Chiamvimonvat N, Chiu WA, Cogliano VJ, Elmore S, Farraj AK, Gomes AV, Mchale CM, Meyer-Tamaki KB, Posnack NG, Vargas HM, Yang X, Zeise L, Zhou CC, Smith MT (2021) Key characteristics of cardiovascular toxicants. Environ Health Perspect 129:95001. https://doi.org/10.1289/EHP9321
Lipton SA, Choi YB, Pan ZH, Lei SZ, Chen HS, Sucher NJ, Loscalzo J, Singel DJ, Srtamler JS (1993) A redox-based mechanism for the neuroprotective and neurodestructive effects of nitric oxide and related nitroso-compounds. Nature 364:626–632. https://doi.org/10.1038/364626a0
Liu F, Jan KY (2000) DNA damage in arsenite- and cadmium-treated bovine aortic endothelial cells. Free Radic Biol Med 28:55–63. https://doi.org/10.1016/s0891-5849(99)00196-3
Liu Q, Hilsenbeck S, Gazitt Y (2003) Arsenic trioxide-induced apoptosis in myeloma cells: p53-dependent G1 or G2/M cell cycle arrest, activation of caspase-8 or caspase-9, and synergy with APO2/TRAIL. Blood 101:4078–4087. https://doi.org/10.1182/blood-2002-10-3231
Liu Y, Zhao D, Qiu F, Zhang LL, Liu SK, Li YY, Liu MT, Wu D, Wang JX, Ding XQ, Liu YX, Dong CJ, Shao XQ, Yang BF, Chu WF (2017) Manipulating PML SUMOylation via silencing UBC9 and RNF4 regulates cardiac fibrosis. Mol Ther 25:666–678. https://doi.org/10.1016/j.ymthe.2016.12.021
Luo SK, Tong L (2021) Structure and function of the separase–securin complex. Subcell Biochem 96:217–232. https://doi.org/10.1007/978-3-030-58971-4_4
Martin-Pardillos A, Sosa C, Sorribas V (2013) Arsenic increases Pi-mediated vascular calcification and induces premature senescence in vascular smooth muscle cells. Toxicol Sci 131:641–653. https://doi.org/10.1093/toxsci/kfs313
Mendez MA, González-Horta C, Sánchez-Ramírez B, Ballinas-Casarrubias L, Cerón RH, Morales DV, Terrazas FAB, Ishida MC, Gutiérrez-Torres DS, Saunders RJ, Drobná Z, Fry RC, Buse JB, Loomis D, García-Vargas GG, Razo LMD, Stýblo M (2016) Chronic Exposure to arsenic and markers of cardiometabolic risk: a cross-sectional study in Chihuahua, Mexico. Environ Health Perspect 124:104–111. https://doi.org/10.1289/ehp.1408742
Nakano T, Takahashi T, Yamamoto C, Kaji T, Fujiwara Y (2021b) Arsenite induces tissue factor synthesis through Nrf2 activation in cultured human aortic smooth muscle cells. J Toxicol Sci 46:187–192. https://doi.org/10.2131/jts.46.187
Nakayama M, Takahashi K, Komaru T, Fukuchi M, Shioiri H, Ki S, Kitamuro T, Shirato K, Yamaguchi T, Suematsu M, Shibahara S (2001) Increased expression of heme oxygenase-1 and bilirubin accumulation in foam cells of rabbit atherosclerotic lesions. Arterioscler Thromb Vasc Biol 21:1373–1377. https://doi.org/10.1161/hq0801.093592
Naujokas MF, Anderson B, Ahsan H, Aposhian HV, Graziano JH, Thompson C, Suk WA (2013) The broad scope of health effects from chronic arsenic exposure: update on a worldwide public health problem. Environ Health Perspect 121:295–302. https://doi.org/10.1289/ehp.1205875
Negro Silva LF, Lemaire M, Lemarié CA, Plourde D, Bolt AM, Chiavatti C, Bohle DS, Slavkovich V, Graziano JH, Lehoux S, Mann KK (2017) Effects of inorganic arsenic, methylated arsenicals, and arsenobetaine on atherosclerosis in the mouse model and the role of As3mt-mediated methylation. Environ Health Perspect 125:077001. https://doi.org/10.1289/EHP806
Negro Silva LF, Makhani K, Lemaire M, Lemarie CA, Plourde D, Bolt AM, Chiavatti C, Bohle DS, Lehoux S, Goldberg MS, Mann KK (2021) Sex-specific effects of prenatal and early life inorganic and methylated arsenic exposure on atherosclerotic plaque development and composition in adult ApoE(-/-) mice. Environ Health Persp 129(5):57008. https://doi.org/10.1289/EHP8171
Nelken NA, Coughlin SR, Gordon D, Wilcox JN (1991) Monocyte chemoattractant protein-1 in human atheromatous plaques. J Clin Investig 88:1121–1127. https://doi.org/10.1172/JCI115411
Nuntharatanapong N, Chen K, Sinhaseni P, Keaney JF (2005) EGF receptor-dependent JNK activation is involved in arsenite-induced p21Cip1/Waf1 upregulation and endothelial apoptosis. American journal of physiology. Heart Circ Physiol 289:H99–H107. https://doi.org/10.1152/ajpheart.00901.2004
Pace C, Banerjee TD, Welch B, Khalili R, Dagda RK, Angermann J (2016) Monomethylarsonous acid, but not inorganic arsenic, is a mitochondria-specific toxicant in vascular smooth muscle cells. Toxicol in Vitro 35:188–201. https://doi.org/10.1016/j.tiv.2016.06.006
Pereira FE, Coffin JD, Beall HD (2007) Activation of protein kinase C and disruption of endothelial monolayer integrity by sodium arsenite: potential mechanism in the development of atherosclerosis. Toxicol Appl Pharmacol 220:164–177. https://doi.org/10.1016/j.taap.2006.12.035
Perry MD, Ng CA, Mangala MM, Ng TYM, Hines AD, Liang W, Xu MJO, Hill AP, Vandenberg JI (2020) Pharmacological activation of IKr in models of long QT Type 2 risks overcorrection of repolarization. Cardiovasc Res 116:1434–1445. https://doi.org/10.1093/cvr/cvz247
Pesce M, Duda GN, Forte G, Girao H, Raya A, Roca-Cusachs P, Sluijter JPG, Tschöpe C, Van Linthout S (2023) Cardiac fibroblasts and mechanosensation in heart development, health and disease. Nat Rev Cardiol 20(5):309–324. https://doi.org/10.1038/s41569-022-00799-2
Phan NN, Li KL, Lin YC (2018) Arsenic induces cardiac rhythm dysfunction and acylcarnitines metabolism perturbation in rats. Toxicol Mech Methods 28:423–431. https://doi.org/10.1080/15376516.2018.1440679
Pi J, Horiguchi S, Sun Y, Nikaido M, Shimojo N, Hayashi T, Yamauchi H, Itoh K, Yamamoto M, Sun G, Waalkes MP, Kumagai Y (2003) A potential mechanism for the impairment of nitric oxide formation caused by prolonged oral exposure to arsenate in rabbits. Free Radic Biol Med 35:102–13. https://doi.org/10.1016/s0891-5849(03)00269-7
Pinto AR, Ilinykh A, Ivey MJ, Kuwabara JT, D’Antoni ML, Debuque R, Chandran A, Wang L, Arora K, Rosenthal NA, Tallquist MD (2016) Revisiting cardiac cellular composition. Circ Res 118:400–9. https://doi.org/10.1161/CIRCRESAHA.115.307778
Podgorski J, Berg M (2020) Global threat of arsenic in groundwater. Science 368:845–850. https://doi.org/10.1126/science.aba1510
Pysher MD, Chen QM, Vaillancourt RR (2008) Arsenic alters vascular smooth muscle cell focal adhesion complexes leading to activation of FAK-src mediated pathways. Toxicol Appl Pharmacol 231:135–141. https://doi.org/10.1016/j.taap.2008.04.002
Raghu KG, Cherian OL (2009) Characterization of cytotoxicity induced by arsenic trioxide (a potent anti-APL drug) in rat cardiac myocytes. J Trace Elem Med Biol 23:61–68. https://doi.org/10.1016/j.jtemb.2008.10.001
Ramos O, Carrizales L, Yáñez L, Mejía J, Batres L, Ortíz D, Díaz-Barriga F (1995) Arsenic increased lipid peroxidation in rat tissues by a mechanism independent of glutathione levels. Environ Health Perspect 103(Suppl 1):85–88. https://doi.org/10.1289/ehp.95103s185
Rebuzzini P, Civello C, Fassina L, Zuccotti M, Garagna S (2021) Functional and structural phenotyping of cardiomyocytes in the 3D organization of embryoid bodies exposed to arsenic trioxide. Sci Rep 11:23116. https://doi.org/10.1038/s41598-021-02590-8
Sanchez-Soria P, Broka D, Monks SL, Camenisch TD (2012) Chronic low-level arsenite exposure through drinking water increases blood pressure and promotes concentric left ventricular hypertrophy in female mice. Toxicol Pathol 40:504–512. https://doi.org/10.1177/0192623311432297
Savoia C, Burger D, Nishigaki N, Montezano A, Touyz RM (2011) Angiotensin II and the vascular phenotype in hypertension. Expert Rev Mol Med 13:1–25. https://doi.org/10.1017/S1462399411001815
Seino Y, Ikeda U, Ikeda M, Yamamoto K, Misawa Y, Hasegawa T, Kano S, Shimada K (1994) Interleukin 6 gene transcripts are expressed in human atherosclerotic lesions. Cytokine 6:87–91. https://doi.org/10.1016/1043-4666(94)90013-2
Seo J, Cho DH, Lee HJ, Sung MS, Lee JY, Won KJ, Park JH, Jo I (2016) Citron Rho-interacting kinase mediates arsenite-induced decrease in endothelial nitric oxide synthase activity by increasing phosphorylation at threonine 497: mechanism underlying arsenite-induced vascular dysfunction. Free Radic Biol Med 90:133–144. https://doi.org/10.1016/j.freeradbiomed.2015.11.020
Shan HL, Zhang Y, Cai BZ, Chen X, Fan YH, Yang LL, Chen XC, Liang HH, Zhang Y, Song XH, Xu CQ, Lu YJ, Yang BF, Du ZM (2013) Upregulation of microRNA-1 and microRNA-133 contributes to arsenic-induced cardiac electrical remodeling. Int J Cardiol 167:2798–2805. https://doi.org/10.1016/j.ijcard.2012.07.009
Sharifi AM, Akbarloo N, Darabi R, Larijani B (2004) Study of correlation between elevation of blood pressure and tissue ACE activity during development of hypertension in 1K1C rats. Vascul Pharmacol 41:15–20. https://doi.org/10.1016/j.vph.2004.03.002
Shi YF, Wei YD, Qu SS, Wang Y, Li YL, Li RG (2010) Arsenic induces apoptosis of human umbilical vein endothelial cells through mitochondrial pathways. Cardiovasc Toxicol 10:153–160. https://doi.org/10.1007/s12012-010-9073-z
Simeonova PP, Hulderman T, Harki D, Luster MI (2003) Arsenic exposure accelerates atherogenesis in apolipoprotein E(-/-) mice. Environ Health Perspect 111:1744–8. https://doi.org/10.1289/ehp.6332
Soucy NV, Klei LR, Mayka DD, Barchowsky A (2004) Signaling pathways for arsenic-stimulated vascular endothelial growth factor-a expression in primary vascular smooth muscle cells. Chem Res Toxicol 17:555–563. https://doi.org/10.1021/tx034193q
Souza ACF, de Paiva Coimbra JL, Ervilha LOG, Bastos DSS, Cossolin JFS, Santos EC, Oliveira LL, Machado-Neves M (2020) Arsenic induces dose-dependent structural and ultrastructural pathological remodeling in the heart of Wistar rats. Life Sci 257:118132. https://doi.org/10.1016/j.lfs.2020.118132
Srivastava S, Vladykovskaya EN, Haberzettl P, Sithu SD, D’Souza SE, States JC (2009) Arsenic exacerbates atherosclerotic lesion formation and inflammation in ApoE-/- mice. Toxicol Appl Pharmacol 241:90–100. https://doi.org/10.1016/j.taap.2009.08.004
Steinmaus C, Bates MN, Yuan Y, Kalman D, Atallah R, Rey OA, Biggs ML, Hopenhayn C, Moore LE, Hoang BK, Smith AH (2006) Arsenic methylation and bladder cancer risk in case-control studies in Argentina and the United States. J Occup Environ Med 48:478–488. https://doi.org/10.1097/01.jom.0000200982.28276.70
Straif K, Benbrahim-Tallaa L, Baan R, Grosse Y, Secretan B, El Ghissassi F, Bouvard V, Guha N, Freeman C, Galichet L, Cogliano V, WHO, (2009) A review of human carcinogens-Part C: metals, arsenic, dusts, and fibres. Lancet Oncol 10:453–454. https://doi.org/10.1016/s1470-2045(09)70134-2
Sumi D, Sasaki T, Miyataka H, Himeno S (2011) Rat H9c2 cardiac myocytes are sensitive to arsenite due to a modest activation of transcription factor Nrf2. Arch Toxicol 85:1509–1516. https://doi.org/10.1007/s00204-011-0700-7
Suriyo T, Watcharasit P, Thiantanawat A, Satayavivad J (2012) Arsenite promotes apoptosis and dysfunction in microvascular endothelial cells via an alteration of intracellular calcium homeostasis. Toxicol in Vitro 26:386–395. https://doi.org/10.1016/j.tiv.2011.12.017
Takayama Y, Masuzaki Y, Mizutani F, Iwata T, Maeda E, Tsukada M, Nomura K, Ito Y, Chisaki Y, Murata K (2021) Associations between blood arsenic and urinary arsenic species concentrations as an exposure characterization tool. Sci Total Environ 750:141517. https://doi.org/10.1016/j.scitotenv.2020.141517
Tallquist MD, Molkentin JD (2017) Redefining the identity of cardiac fibroblasts. Nat Rev Cardiol 14(8):484–491. https://doi.org/10.1038/nrcardio.2017.57
Tang DL, Kang R, Berghe TV, Vandenabeele P, Kroemer G (2019) The molecular machinery of regulated cell death. Cell Res 29:347–364. https://doi.org/10.1038/s41422-019-0164-5
Tsai SH, Hsieh MS, Chen L, Liang YC, Lin JK, Lin SY (2001) Suppression of Fas ligand expression on endothelial cells by arsenite through reactive oxygen species. Toxicol Lett 123:11–19. https://doi.org/10.1016/s0378-4274(01)00373-3
Tsai MH, Chen SC, Wang HJ, Yu HS, Chang LW (2005) A mouse model for the study of vascular permeability changes induced by arsenic. Toxicol Mech Methods 15:433–437. https://doi.org/10.1080/15376520500195640
Tsou TC, Tsai FY, Hsieh YW, Li LA, Yeh SC, Chang LW (2005) Arsenite induces endothelial cytotoxicity by down-regulation of vascular endothelial nitric oxide synthase. Toxicol Appl Pharmacol 208:277–284. https://doi.org/10.1016/j.taap.2005.03.001
Tsou TC, Tsai FY, Yeh SC, Chang LW (2006) ATM/ATR-related checkpoint signals mediate arsenite-induced G2/M arrest in primary aortic endothelial cells. Arch Toxicol 80:804–810. https://doi.org/10.1007/s00204-006-0110-4
Vahter M (2009) Effects of arsenic on maternal and fetal health. Annu Rev Nutr 29:381–399. https://doi.org/10.1146/annurev-nutr-080508-141102
Veenema R, Casin KM, Sinha P, Kabir R, Mackowski N, Taube N, Bedja D, Chen R, Rule A, Kohr MJ (2019) Inorganic arsenic exposure induces sex-disparate effects and exacerbates ischemia-reperfusion injury in the female heart. Am J Physiol Heart Circ Physiol 316:H1053–H1064. https://doi.org/10.1152/ajpheart.00364.2018
Wang Y, Tang M (2019) PM2.5 induces ferroptosis in human endothelial cells through iron overload and redox imbalance. Environ Pollut 254(Pt A):112937. https://doi.org/10.1016/j.envpol.2019.07.105
Wang L, Kou MC, Weng CY, Hu LW, Wang YJ, Wu MJ (2012) Arsenic modulates heme oxygenase-1, interleukin-6, and vascular endothelial growth factor expression in endothelial cells: roles of ROS, NF-κB, and MAPK pathways. Arch Toxicol 86:879–896. https://doi.org/10.1007/s00204-012-0845-z
Wang QQ, Lan YF, Rehman K, Jiang YH, Maimaitiyiming Y, Zhu DY, Naranmandura H (2015) Effect of arsenic compounds on the in vitro differentiation of mouse embryonic stem cells into cardiomyocytes. Chem Res Toxicol 28:351–353. https://doi.org/10.1021/tx500286t
Wang XT, Mou Y, Yue Z, Zhang HY, Su XJ, Wang Y, Li RG, Sun X (2016) Arsenite suppresses angiogenesis of vascular endothelial cells mediated by Platelet Derived Growth Factor Receptor-beta. Environ Toxicol Pharmacol 46:168–173. https://doi.org/10.1016/j.etap.2016.07.009
Wang Y, Xiong L, Wu T, Zhang T, Kong L, Xue Y, Tang M (2018) Analysis of differentially changed gene expression in EA.hy926 human endothelial cell after exposure of fine particulate matter on the basis of microarray profile. Ecotoxicol Environ Saf 159:213–220. https://doi.org/10.1016/j.ecoenv.2018.05.002
Wang WJ, Wang QL, Zou ZL, Zheng FY, Zhang AH (2020a) Human arsenic exposure and lung function impairment in coal-burning areas in Guizhou. China Ecotoxicol Environ Saf 190:110174. https://doi.org/10.1016/j.ecoenv.2020.110174
Wang Y, Kong L, Wu T, Tang M (2020b) Urban particulate matter disturbs the equilibrium of mitochondrial dynamics and biogenesis in human vascular endothelial cells. Environ Pollut 264:114639. https://doi.org/10.1016/j.envpol.2020.114639
Wang Y, Liu N, Huang X, Hu W, Ma Y, Liang Y, Xie W, Tang M (2021) Atmospheric particulate matter impedes autophagic flux by impairing lysosomal milieu and integrity in human umbilical vein endothelial cells (HUVECs). Sci Total Environ 761:143290. https://doi.org/10.1016/j.scitotenv.2020.143290
Wang LY, Liu SG, Gao C, Chen H, Li J, Lu JR, Yuan Y, Zheng XL, He HB, Zhang XX, Zhang RD, Zhang YY, Wu Y, Lin W, Zheng HY (2022) Arsenic trioxide-induced cardiotoxicity triggers ferroptosis in cardiomyoblast cells. Hum Exp Toxicol 41:9603271211064536. https://doi.org/10.1177/09603271211064537
Wāng Y, Han Y, Xu DX (2024) Developmental impacts and toxicological hallmarks of silver nanoparticles across diverse biological models. Environ Sci Ecotechnol 19:100325. https://doi.org/10.1016/j.ese.2023.100325
Watanabe M, Funakoshi T, Unuma K, Aki T, Uemura K (2014) Activation of the ubiquitin-proteasome system against arsenic trioxide cardiotoxicity involves ubiquitin ligase Parkin for mitochondrial homeostasis. Toxicology 322:43–50. https://doi.org/10.1016/j.tox.2014.04.008
Wei S, Qiu TM, Yao XF, Wang NN, Jiang LP, Jia X, Tao Y, Wang ZD, Pei P, Zhang JY, Zhu YH, Yang G, Liu XF, Liu S, Sun XC (2020) Arsenic induces pancreatic dysfunction and ferroptosis via mitochondrial ROS-autophagy-lysosomal pathway. J Hazard Mater 384:121390. https://doi.org/10.1016/j.jhazmat.2019.121390
Weng CY, Chiou SY, Wang L, Kou MC, Wang YJ, Wu MJ (2014) Arsenic trioxide induces unfolded protein response in vascular endothelial cells. Arch Toxicol 88:213–26. https://doi.org/10.1007/s00204-013-1101-x
Wu XA, Larsson HP (2020) Insights into Cardiac IKs (KCNQ1/KCNE1) Channels Regulation. Int J Mol Sci 21(24):9440. https://doi.org/10.3390/ijms21249440
Xu XD, Liu SS, Aodengqimuge WHL, Hu MR, Xing C, Song L (2017) Arsenite induces vascular endothelial cell dysfunction by activating IRE1 α/XBP1s/HIF1 α-dependent ANGII signaling. Toxicol Sci 160:315–328. https://doi.org/10.1093/toxsci/kfx184
Xue LL, Zhao ZJ, Zhang YF, Liao J, Wu M, Wang MG, Sun J, Gong HQ, Guo M, Li SH, Zheng Y (2020) Dietary exposure to arsenic and human health risks in western Tibet. Sci Total Environ 731:138840. https://doi.org/10.1016/j.scitotenv.2020.138840
Yancy SL, Shelden EA, Gilmont RR, Welsh MJ (2005) Sodium arsenite exposure alters cell migration, focal adhesion localization and decreases tyrosine phosphorylation of focal adhesion kinase in H9C2 myoblasts. Toxicol Sci 84:278–286. https://doi.org/10.1093/toxsci/kfi032
Yu CX, Zhang YY, Wu XY, Tang HX, Liang XQ, Xue ZM, Xue YD, Li J, Zhu H, Huo R, Ban T (2019) Transient receptor potential melastatin 4 contributes to early-stage endothelial injury induced by arsenic trioxide. Toxicol Lett 312:98–108. https://doi.org/10.1016/j.toxlet.2019.04.035
Zeigler AC, Chandrabhatla AS, Christiansen SL, Nelson AR, Holmes JW, Saucerman JJ (2021) Network model-based screen for FDA-approved drugs affecting cardiac fibrosis. CPT Pharmacomet Syst Pharmacol 10:377–388. https://doi.org/10.1002/psp4.12599
Zeisberg EM, Kalluri R (2010) Origins of cardiac fibroblasts. Circ Res 107(11):1304–1312. https://doi.org/10.1161/CIRCRESAHA.110.231910
Zhang J, Mu XL, Xu WP, Martin FL, Alamdar A, Liu LP, Tian MP, Huang QY, Shen HQ (2014) Exposure to arsenic via drinking water induces 5-hydroxymethylcytosine alteration in rat. Sci Total Environ 497–498:618–625. https://doi.org/10.1016/j.scitotenv.2014.08.009
Zhang Y, Wu XX, Li Y, Zhang HY, Li ZG, Zhang Y, Zhang LY, Ju JM, Liu X, Chen XH, Glybochko PV, Nikolenko V, Kopylov P, Xu CQ, Yang BF (2016) Endothelial to mesenchymal transition contributes to arsenic-trioxide-induced cardiac fibrosis. Sci Rep 6:33787. https://doi.org/10.1038/srep33787
Zhao XY, Feng TM, Chen H, Shan HL, Zhang Y, Lu YJ, Yang BF (2008) Arsenic trioxide-induced apoptosis in H9c2 cardiomyocytes: implications in cardiotoxicity. Basic Clin Pharmacol Toxicol 102:419–425. https://doi.org/10.1111/j.1742-7843.2007.00150.x
Zhao X, Shi YQ, Yan CC, Feng PF, Wang X, Zhang R, Zhang X, Li BX (2015) Up-regulation of miR-21 and miR-23a contributes to As2O3-induced hERG channel deficiency. Basic Clin Pharmacol Toxicol 116:516–523. https://doi.org/10.1111/bcpt.12348
Zhao JX, Li A, Mei YY, Zhou Q, Li YB, Li K, Xu Q (2021) The association of arsenic exposure with hypertension and blood pressure: A systematic review and dose-response meta-analysis. Environ Pollut 289:117914. https://doi.org/10.1016/j.envpol.2021.117914
Zhou L, Xu ZF, Zhou JW, Fan PK (2022) Natural arsenic source, migration, and flux in a catchment on the Southern Tibetan Plateau. Sci Total Environ 838:155898. https://doi.org/10.1016/j.scitotenv.2022.155898
Zuo Z, Liu ZY, Gao TC, Yin YY, Wang ZD, Hou YY, Fu JQ, Liu SN, Wang HH, Xu YY, Pi JB (2019) Prolonged inorganic arsenic exposure via drinking water impairs brown adipose tissue function in mice. Sci Total Environ 668:310–317. https://doi.org/10.1016/j.scitotenv.2019.03.008
Funding
This work was supported by the National Natural Science Foundation of China (grant number 82103883), Research Fund of Anhui Institute of Translational Medicine (2022zhyx-C15), and Scientific Research Fund from Anhui Medical University (2021xkj010).
Author information
Authors and Affiliations
Contributions
YW involved in conceptualization, critical thinking, writing—original draft, review and editing, supervision, and project administration. LM, CW, TG, and YH involved in literature retrieval, figure drawing, and table compilation. D-XX involved in supervision and resources. All authors read and approved the final manuscript. Use of large language models, artificial intelligence applications, or algorithmic tools: The authors declare that they have not used any of large language models, artificial intelligence applications, or algorithmic tools in the preparation or revision of their manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wāng, Y., Ma, L., Wang, C. et al. Cardiovascular adverse effects and mechanistic insights of arsenic exposure: a review. Environ Chem Lett 22, 1437–1472 (2024). https://doi.org/10.1007/s10311-023-01677-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10311-023-01677-0