Abstract
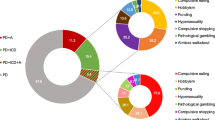
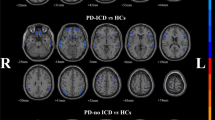
Impulse control disorders (ICDs) are a group of non-motor symptoms of Parkinson disease (PD) leading to significant psychosocial detrimental outcome. The mesocorticolimbic network plays a distinctive role in reward learning and executive decision making and has been suggested to be involved in ICDs in PD. To study morphometric changes of the mesocorticolimbic network in PD with ICD. A total of 18 patients of PD with ICD (PD + ICD), 19 patients of PD without ICD (PD − ICD) and 19 healthy controls (HC) were included in the study. ICDs were diagnosed using Questionnaire for Impulsive-Compulsive Disorders in PD-Rating Scale (QUIP-RS). MRI was done using a 3T scanner and assessment of cortical thickness and subcortical volumes were done using FreeSurfer. Brain regions known to be part of the mesocorticolimbic network were extracted and included for statistical analysis. There was no difference between PD + ICD and PD − ICD with regard to duration of illness or total dopaminergic medication. In comparison to HC, patients with PD + ICD demonstrated atrophy of the left frontal pole, and this atrophy neared significance in comparison to PD − ICD. The QUIP-RS had a negative correlation with left caudate volume in PD + ICD. The PD + ICD group showed distinct morphometric changes in regions involved in the mesocorticolimbic system which may contribute to the presence of ICD.


Similar content being viewed by others
Data availability
Data will be shared upon reasonable request.
References
Alcaro A, Huber R, Panksepp J (2007) Behavioral functions of the mesolimbic dopaminergic system: an affective neuroethological perspective. Brain Res Rev 56(2):283–321
Aracil-Bolaños I, Strafella AP (2016) Molecular imaging and neural networks in impulse control disorders in Parkinson’s disease. Parkinsonism Relat Disord 22:S101–S105
Arias-Carrion O et al (2010) Dopaminergic reward system: a short integrative review. Int Arch Med 3:24
Biundo R et al (2015) Patterns of cortical thickness associated with impulse control disorders in Parkinson’s disease. Move Disord 30(5):688–695
Callesen MB et al (2013) A systematic review of impulse control disorders in Parkinson’s disease. J Parkinsons Dis 3(2):105–138
Ceravolo R et al (2009) Impulse control disorders in Parkinson’s disease: definition, epidemiology, risk factors, neurobiology and management. Parkinsonism Relat Disord 15:S111–S115
Demetriades P, Rickards H, Cavanna AE (2011) Impulse control disorders following deep brain stimulation of the subthalamic nucleus in Parkinson’s disease: clinical aspects. Parkinson’s Disease. https://doi.org/10.4061/2011/658415
Fischl B (2012) FreeSurfer. Neuroimage 62(2):774–781
Gatto EM, Aldinio V (2019) Impulse control disorders in Parkinson’s disease. A brief and comprehensive review. Front Neurol 10:351
Gremel CM, Lovinger DM (2017) Associative and sensorimotor cortico-basal ganglia circuit roles in effects of abused drugs. Genes Brain Behav 16(1):71–85
Hughes AJ et al (1992) Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry 55(3):181–184
Imperiale F et al (2017) Brain structural and functional signatures of impulsive-compulsive behaviours in Parkinson’s disease. Mol Psychiatry 23(2):459–466
Latella D et al (2019) Impulse control disorders in Parkinson’s disease: a systematic review on risk factors and pathophysiology. J Neurol Sci 398:101–106
Martinez E et al (2020) The anterior caudate nucleus supports impulsive choices triggered by pramipexole. Move Disord 35(2):296–305
Parra-Díaz P et al (2021) Does the country make a difference in impulse control disorders? A systematic review. Move Disord Clin Pract 8(1):25–32
Pellicano C et al (2015) Morphometric changes in the reward system of Parkinson’s disease patients with impulse control disorders. J Neurol 262(12):2653–2661
Prasad S et al (2019) Abnormal subcortical volumes and cortical thickness in Parkinson’s disease with impulse control disorders. Ann Indian Acad Neurol 22(4):426
Probst CC, Van Eimeren T (2013) The functional anatomy of impulse control disorders. Curr Neurol Neurosci Reports 13:1–10
Rao H et al (2010) Decreased ventral striatal activity with impulse control disorders in Parkinson’s disease. Move Disord 25(11):1660–1669
Robinson S et al (2009A) resting state network in the motor control circuit of the basal ganglia. BMC Neurosci 10:1–14
Rolls ET, Cheng W, Feng J (2020) The orbitofrontal cortex: reward, emotion and depression. Brain Commun 2(2):fcaa196
Santangelo G et al (2013) Pathological gambling in Parkinson’s disease. A comprehensive review. Parkinsonism Relat Disord 19(7):645–653
Tessitore A et al (2016) Cortical thickness changes in patients with Parkinson’s disease and impulse control disorders. Parkinsonism Relat Disord 24:119–125
Vela L et al (2016) The high prevalence of impulse control behaviors in patients with early-onset Parkinson’s disease: a cross-sectional multicenter study. J Neurol Sci 368:150–154
Voon V et al (2009) Chronic dopaminergic stimulation in Parkinson’s disease: from dyskinesias to impulse control disorders. Lancet Neurol 8(12):1140–1149
Weintraub D (2008) Dopamine and impulse control disorders in Parkinson’s disease. Ann Neurol 64(S2):S93–S100
Funding
The study was funded by Parkinson Disease and movement disorder fund of National Institute of Mental Health and Neurosciences.
Author information
Authors and Affiliations
Contributions
MFA: research project: conception, organization, execution and statistical analysis: design, execution, manuscript preparation: writing of the first draft. SP: research project: conception, organization, execution and statistical analysis: design, execution, manuscript preparation: review and critique. SB: research project: organization, execution, statistical analysis, execution, review and critique. NK: research project, organization, execution and statistical analysis: design, execution, manuscript preparation: review and critique. RK: research project: execution, statistical analysis: review and critique and manuscript preparation: review and critique. VVH: research project: execution, statistical analysis: review and critique and manuscript preparation: review and critique. RM: research project: conception, statistical analysis: design, review and critique, manuscript preparation: review and critique. RY: research project: organization, execution, statistical analysis: review and critique, manuscript preparation: review and critique. JS: research project: conception, execution, statistical analysis: design, review and critique, manuscript preparation: review and critique. PKP: research project: conception, organization, statistical analysis: design, review and critique, manuscript preparation: review and critique.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ansari, M.F., Prasad, S., Bhardwaj, S. et al. Morphometric alterations of the mesocorticolimbic network in Parkinson’s disease with impulse control disorders. J Neural Transm 131, 229–237 (2024). https://doi.org/10.1007/s00702-023-02735-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-023-02735-1