Abstract
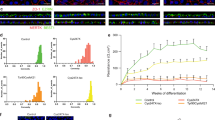
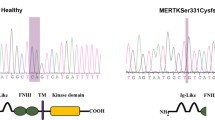
Oculocutaneous albinism (OCA) is characterized by reduced melanin biosynthesis affecting the retina, thus impairing visual function. The disease pathology of OCA is poorly understood at the cellular level due to unavailability of suitable biological model systems. This study aimed to develop a disease-specific in vitro model for OCA type 1A, the most severe form caused by TYR (tyrosinase) gene mutations, using retinal pigment epithelium (RPE) differentiated from patient-derived human-induced pluripotent stem cells (hiPSCs). A comparative study between healthy and OCA1A RPE cells revealed that while healthy RPE cells exhibited timely onest of pigmentation during differentiation, OCA1A RPE cells failed to pigment even after an extended culture period. This observation was validated by ultrastructural studies using electron microscopy, hinting at melanosome-specific defects. Immunocytochemistry demonstrated abnormal expression patterns of melanogenesis-specific protein markers in OCA1A RPE cells, indicating reduced or absence of melanin synthesis. Next, a quantitative assay was performed to confirm the absence of melanin production in OCA1A RPE cells. Tyrosinase assay showed no activity in OCA1A compared with healthy RPE, suggesting non-functionality of TYR, further corroborated by western blot analysis showing complete absence of the protein. Gene expression by RNA sequencing of healthy and OCA1A RPE cells uncovered differential gene expression associated with lens development, visual perception, transmembrane transporter activity, and key signaling pathways. This disease-in-a-dish model of OCA1A provides an excellent platform to understand disease mechanism, identify potential therapeutic targets, and facilitate gene therapy or gene correction.




Similar content being viewed by others
References
Adams DR, Menezes S, Jauregui R, et al. 2019 One-year pilot study on the effects of nitisinone on melanin in patients with OCA-1B. JCI Insight 4 e124387
Baghbaderani BA, Tain X, Neo BH, et al. 2015 cGMP-manufactured human induced pluripotent stem cells are available for pre-clinical and clinical applications. Stem Cell Rep. 5 647–659
Bakker R, Wagstaff EL, Kruijt CC, et al. 2022 The retinal pigmentation pathway in human albinism: Not so black and white. Prog. Retin. Eye Res. 91 101091
Blasiak J, Hyttinen JMT, Szczepanska J, et al. 2021 Potential of long non-coding RNAs in age-related macular degeneration. Int. J. Mol. Sci. 22 9178
Chong JX, Ouwenga R, Anderson RL, et al. 2012 A population-based study of autosomal-recessive disease-causing mutations in a founder population. Am. J. Hum. Genet. 91 608–620
Gargiulo A, Bonetti C, Montefusco S, et al. 2009 AAV-mediated tyrosinase gene transfer restores melanogenesis and retinal function in a model of oculo-cutaneous albinism type I (OCA1). Mol. Ther. 17 1347–1354
George A, Sharma R, Pfister T, et al. 2022 In vitro disease modeling of oculocutaneous albinism type 1 and 2 using human induced pluripotent stem cell-derived retinal pigment epithelium. Stem Cell Rep. 17 173–186
Jeyabalan N, Ghosh A, Mathias GP, et al. 2022 Rare eye diseases in India: A concise review of genes and genetics. Indian J. Ophthalmol. 70 2232–2238
Konala VB, Nandakumar S, Battu R, et al. 2020 Derivation of three induced pluripotent stem cell lines under feeder-free culture conditions from peripheral blood mononuclear cells (PBMC) of Indian patients suffering from inherited retinal diseases carrying different mutations. Stem Cell Res. 45 101757
Kromberg JGR, Flynn KA and Kerr RA 2023 Determining a worldwide prevalence of oculocutaneous albinism: a systematic review. Invest. Ophthalmol. Vis. Sci. 64 14
Liu S, Kuht HJ, Moon EH, et al. 2021 Current and emerging treatments for albinism. Surv. Ophthalmol. 66 362–377
Mabula JB, Chalya PL, Mchembe MD, et al. 2012 Skin cancers among Albinos at a university teaching hospital in Northwestern Tanzania: a retrospective review of 64 cases. BMC Dermatol. 12 5
Maiorano NA and Hindges R 2012 Non-coding RNAs in retinal development. Int. J. Mol. Sci. 13 558–578
Marçon CR and Maia M 2019 Albinism: epidemiology, genetics, cutaneous characterization, psychosocial factors. An. Bras. Dermatol. 94 503–520
Mohan R 2019 Eye of the beholder: Rare eye diseases in focus. J. Neurosci. Res. 97 3–6
Mondal S, Thampi A and Puranik M 2018 Kinetics of melanin polymerization during enzymatic and nonenzymatic oxidation. J. Phys. Chem. B 122 2047–2063
Nguengang Wakap S, Lambert DM, Olry A, et al. 2020 Estimating cumulative point prevalence of rare diseases: analysis of the Orphanet database. Eur. J. Hum. Genet. 28 165–173
Pan T, Zhu J, Hwu W, et al. 2012 The role of apha-synuclein in melanin synthesis in melanoma and dopaminergic neuronal cells. PLoS One 7 e45183
Raposo G and Marks MS 2007 Melanosomes - dark organelles enlighten endosomal membrane transport. Nat. Rev. Mol. Cell. Biol. 8 786–797
Ray K, Chaki M and Sengupta M 2007 Tyrosinase and ocular diseases: some novel thoughts on the molecular basis of oculocutaneous albinism type 1. Prog. Retin. Eye Res. 26 323–358
Renugadevi K, Sil AK, Perumalsamy V, et al. 2010 Spectrum of candidate gene mutations associated with Indian familial oculocutaneous and ocular albinism. Mol. Vis. 16 1514–1524
Sharma R, Khristov V, Rising A, et al. 2019 Clinical-grade stem cell-derived retinal pigment epithelium patch rescues retinal degeneration in rodents and pigs. Sci. Transl. Med. 11 5580
Sharma R, George A, Nimmagadda M, et al. 2021 Epithelial phenotype restoring drugs suppress macular degeneration phenotypes in an iPSC model. Nat. Commun. 12 7293
Summers CG, Connett JE, Holleschau AM, et al. 2014 Does levodopa improve vision in albinism? Results of a randomized, controlled clinical trial. Clin. Exp. Ophthalmol. 42 713–721
Surendran H, Nandakumar S, Reddy KVB, et al. 2021 Transplantation of retinal pigment epithelium and photoreceptors generated concomitantly via small molecule-mediated differentiation rescues visual function in rodent models of retinal degeneration. Stem Cell Res. Ther. 12 70
Surendran H, Soundararajan L, Reddy KVB, et al. 2022 An improved protocol for generation and characterization of human-induced pluripotent stem cell-derived retinal pigment epithelium cells. STAR Protoc. 3 101803
Teramae A, Kobayashi Y, Kunimoto H, et al. 2019 The molecular basis of chemical chaperone therapy for oculocutaneous albinism type 1A. J. Invest. Dermatol. 139 1143–1149
Wang N and Hebert DN 2006 Tyrosinase maturation through the mammalian secretory pathway: bringing color to life. Pigment Cell Res. 19 3–18
Widlund HR and Fisher DE 2003 Microphthalamia-associated transcription factor: a critical regulator of pigment cell development and survival. Oncogene 22 3035–3041
Acknowledgements
The authors thank the Next Generation Genomics Facility (NGGF) and the Central Imaging and Flow Cytometry Facility (CIFF) at the Bangalore LifeScience Cluster. Jasmin MR from the Centre for Cellular and Molecular Platforms (C-CAMP), Bengaluru, is acknowledged for her technical help with Western blots. The authors are grateful to Jair Montford, National Eye Institute, NIH, Bethesda, for the electron microscopy work. The authors are also thankful to their collaborators, Prof. Ramaswamy Subramanian and Dr. Kanaga Vijayan, Purdue University, Indiana, for their inputs during the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Corresponding editor: Sudha Bhattacharya
This article is part of the Topical Collection: The Rare Genetic Disease Research Landscape in India.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Subramani, J., Patlolla, N., Battu, R. et al. Generation and characterization of retinal pigment epithelium from patient iPSC line to model oculocutaneous albinism (OCA)1A disease. J Biosci 49, 21 (2024). https://doi.org/10.1007/s12038-023-00406-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12038-023-00406-7