Abstract
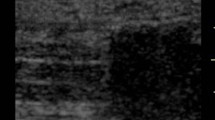
Ultrasound has become a valuable tool for detecting fluid accumulations due to its ability to reveal the nature of the fluid based on its appearance and anatomical location. This case report explores the use of ultrasound in diagnosing an abdominal collection suggestive of peritonitis by introducing an ultrasonographic dynamic sign. A 37-year-old patient, post-rectal tumor surgery, presented with abdominal pain, peritoneal reaction, and clinical deterioration necessitating intensive care. Point-of-care ultrasound revealed a hyperechoic, mobile, image with septa resembling a jellyfish in the subhepatic region, indicating a complicated fluid collection. Abdominal CT confirmed the presence of free fluid in perihepatic and left subphrenic regions. Subsequent surgery revealed peritonitis, anastomosis suture dehiscence, and successful management in the ICU. Recognizing the “abdominal jellyfish sign” and interpreting it appropriately within the relevant clinical context aids in the diagnosis of complicated abdominal collections. Further studies employing alternative methodologies will be necessary to confirm or refute the true significance of this sign in this context.

Similar content being viewed by others
Data Availability
Data will be made available on request.
Code Availability
Not applicable.
Abbreviations
- ICU :
-
Intensive care unit
- POCUS :
-
Point-of-care ultrasound
- CT :
-
Computed tomography
References
Çekiç B, Toslak IE, Şahintürk Y, Cekin AH, Koksel YK, Koroglu M, Demos TC. Differentiating transudative from exudative ascites using quantitative B-mode gray-scale ultrasound histogram. AJR Am J Roentgenol. 2017;209(2):313–9. https://doi.org/10.2214/AJR.16.16509.
Palleri E, Kaiser S, Wester T, Arnell H, Bartocci M. Complex fluid collection on abdominal ultrasound indicates need for surgery in neonates with necrotizing enterocolitis. Eur J Pediatr Surg. 2017;27(2):161–5. https://doi.org/10.1055/s-0036-1580702.
Rudralingam V, Footitt C, Layton B. Ascites matters. Ultrasound. 2017;25(2):69–79. https://doi.org/10.1177/1742271X16680653.
Lee FC. Lung ultrasound-a primary survey of the acutely dyspneic patient. J Intensive Care. 2016;4(1):57. https://doi.org/10.1186/s40560-016-0180-1.
Dugar S, Fox S, Koratala A, Moghekar A, Mehta AC. Lung ultrasonographic signs in pulmonary disease - a video review. J Intensive Care Med. 2023;38(2):220–31. https://doi.org/10.1177/08850666221120221.
Author information
Authors and Affiliations
Contributions
Conceptualization: RAG and IC. Methodology: IC. Formal analysis and investigation: IC. Writing — original draft preparation: IC. Writing — review and editing: IC. Supervision: IC.
Corresponding author
Ethics declarations
Ethics Approval
Approval for this study was waived in accordance with the local regulations because this study is a case report of a single patient and did not include protected health information, data analysis, or testing of a hypothesis and was de-identified.
Consent to Participate
Not applicable.
Consent for Publication
Written informed consent was obtained from the individual for the publication of any potentially identifiable images or data included in this article.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Imaging
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 3568 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheong, I., Gómez, R.A. The Abdominal Jellyfish Sign: An Ultrasonographic Approach for Diagnosing Abdominal Collections — A Case Report. SN Compr. Clin. Med. 6, 15 (2024). https://doi.org/10.1007/s42399-024-01645-x
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-024-01645-x