Abstract
Background
The mediastinal shift angle is a new fetal magnetic resonance imaging (MRI) index that is reportedly correlated with postnatal survival in fetuses with congenital diaphragmatic hernia. However, its correlation in patients with congenital pulmonary airway malformation (CPAM) has not been assessed.
Objective
This study aimed to establish a normal range for the right/left mediastinal shift angles, to evaluate the mediastinal shift angle in fetuses with CPAM, to compare the mediastinal shift angle with the CPAM volume ratio, and to evaluate the predictive value of the mediastinal shift angle measurements.
Materials and methods
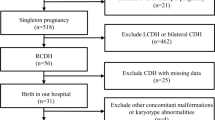
To establish the normal range, we measured the mediastinal shift angle bilaterally in 124 fetuses without any lung abnormality (the control group). Subsequently, the mediastinal shift angle was measured in 32 fetuses pathologically diagnosed with CPAM. Moreover, the mediastinal shift angle and CPAM volume ratio were compared using fetal MRI.
Results
The mean values for the right/left mediastinal shift angles were 18.6°/26.3° and 39.2°/35.9° for control fetuses and fetuses with CPAM, respectively. The mediastinal shift angle and the CPAM volume ratio showed a positive statistical correlation. The area under the curve demonstrated high discriminatory accuracy for the mediastinal shift angle (0.76).
Conclusion
The mediastinal shift angle has potential to replace the CPAM volume ratio for evaluating the severity of CPAM in fetal MRI.
Graphical Abstract







Similar content being viewed by others
Data availability
The datasets generated and/or analyzed in the current study are available from the corresponding author on reasonable request.
References
Stocker JT (2002) Congenital pulmonary airway malformation- a new name for and an expanded classification of congenital cystic adenomatoid malformation of the lung. Histopathology 41:424–430
Sfakianaki AK, Copel JA (2012) Congenital cystic lesions of the lung: congenital cystic adenomatoid malformation and bronchopulmonary sequestration. Rev Obstet Gynecol 5:85–93. PMID: 22866187; PMCID: PMC3410507
Adzick NS, Harrison MR, Crombleholme TM, Flake AW, Howell LJ (1998) Fetal lung lesions: management and outcome. Am J Obstet Gynecol 179:884–889. https://doi.org/10.1016/s0002-9378(98)70183-8
Adzick NS, Kitano Y (2003) Fetal surgery for lung lesions, congenital diaphragmatic hernia, and sacrococcygeal teratoma. Semin Pediatr Surg 12:154–167. https://doi.org/10.1016/S1055-8586(03)00030-1
Quintero RA, Kontopoulos EV, Quintero LF, Landy DC, Gonzalez R, Chmait RH (2013) The observed vs. expected lung-to-head ratio does not correct for the effect of gestational age on the lung-to-head ratio. J Matern Fetal Neonatal Med 26:552–557. https://doi.org/10.3109/14767058.2012.736000
Aspelund G, Fisher JC, Simpson LL, Stolar CJ (2012) Prenatal lung-head ratio: threshold to predict outcome for congenital diaphragmatic hernia. J Matern Fetal Neonatal Med 25:1011–1016. https://doi.org/10.3109/14767058.2011.608442
Jani J, Nicolaides KH, Keller RL, Benachi A, Peralta CF, Favre R, Moreno O, Tibboel D, Lipitz S, Eggink A, Vaast P, Allegaert K, Harrison M, Deprest J (2007) Observed to expected lung area to head circumference ratio in the prediction of survival in fetuses with isolated diaphragmatic hernia. Ultrasound Obstet Gynecol 30:67–71. https://doi.org/10.1002/uog.4052
Victoria T, Danzer E, Adzick NS (2013) Use of ultrasound and MRI for evaluation of lung volumes in fetuses with isolated left congenital diaphragmatic hernia. Semin Pediatr Surg 22:30–36. https://doi.org/10.1053/j.sempedsurg2012.10.006
Savelli S, Bascetta S, Carducci C, Carnevale E, Caforio L, Romiti A, Tomà P (2020) Fetal MRI assessment of mediastinal shift angle in isolated left congenital diaphragmatic hernia: a new postnatal survival predictive tool? Prenat Diagn 40:136–141. https://doi.org/10.1002/pd.5619
Romiti A, Viggiano M, Savelli S, Salvi S, Vicario R, Vassallo C, Valfrè L, Tomà P, Bonito M, Lanzone A, Bagolan P, Caforio L (2022) Comparison of mediastinal shift angles obtained with ultrasound and magnetic resonance imaging in fetuses with isolated left sided congenital diaphragmatic hernia. J Matern Fetal Neonatal Med 35:269–274. https://doi.org/10.1080/14767058.2020.1716714
Amodeo I, Borzani I, Corsani G, Pesenti N, Raffaeli G, Macchini F, Condò V, Persico N, Ghirardello S, Colnaghi M, Mosca F, Cavallaro G (2022) Fetal MRI mediastinal shift angle and respiratory and cardiovascular pharmacological support in newborns with congenital diaphragmatic hernia. Eur J Pediatr 181:323–334. https://doi.org/10.1007/s00431-021-04207-8
Romiti A, Viggiano M, Conforti A, Valfré L, Ravà L, Ciofi Degli Atti M, Bagolan P, Caforio L (2020) Ultrasonographic assessment of mediastinal shift angle (MSA) in isolated left congenital diaphragmatic hernia for the prediction of postnatal survival. J Matern Fetal Neonatal Med 33:1330–1335. https://doi.org/10.1080/14767058.2018.1517329
Crombleholme TM, Coleman B, Hedrick H, Liechty K, Howell L, Flake AW, Johnson M, Adzick NS (2002) Cystic adenomatoid malformation volume ratio predicts outcome in prenatally diagnosed cystic adenomatoid malformation of the lung. J Pediatr Surg 37:331–338. https://doi.org/10.1053/jpsu.2002.30832
Cass DL, Olutoye OO, Cassady CI, Moise KJ, Johnson A, Papanna R, Lazar DA, Ayres NA, Belleza-Bascon B (2011) Prenatal diagnosis and outcome of fetal lung masses. J Pediatr Surg 46:292–298. https://doi.org/10.1016/j.jpedsurg.2010.11.004
Adzick NS, Flake AW, Crombleholme TM (2003) Management of congenital lung lesions. Semin Pediatr Surg 12:10–16. https://doi.org/10.1053/spsu.2003.50002
Di Prima FA, Bellia A, Inclimona G, Grasso F, Teresa M, Cassaro MN (2012) Antenatally diagnosed congenital cystic adenomatoid malformations (CCAM): research review. J Prenat Med 6:22–30
Acknowledgements
We thank Junko Ihara, Taizou Somemori, Keisuke Asano, Masaya Fujiyoshi, Ryota Hiura, and Kasumi Watanabe, MRI technologists at the National Center for Child Health and Development.
Author information
Authors and Affiliations
Contributions
O.M., Y.S., S.I., R.O., M.M., Y.T., Y.I., H.S․, Y.K., Y.H., T.A., and S.N. conceived, supervised, and supported the study. J.T., O.M., and M.M. collated and analyzed the data, performed the statistical analysis, and drafted the initial manuscript. J.T. and O.M. interpreted the images. J.T., O.M., and T.A. edited the manuscript. All authors have reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tsukamoto, J., Miyazaki, O., Saito, Y. et al. Assessment of mediastinal shift angles in congenital pulmonary airway malformation: a new fetal magnetic resonance imaging indicator of congenital lung disease. Pediatr Radiol 54, 715–724 (2024). https://doi.org/10.1007/s00247-024-05852-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-024-05852-5