Abstract
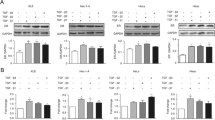
Breast cancer progression, metastasis and recurrence are largely driven by breast cancer stem cells (BCSCs), which constitute a subset of tumor cells exhibiting stem cell characteristics. In this study, we evaluated the role of estrogen-related receptor alpha (ERRα) in the migration, invasion and angiogenesis of BCSCs. The inhibition of ERRα using XCT790 or knockdown of ERRα using shRNA inhibited the mammosphere formation efficiency, as well as the migration and invasion of BCSCs derived from the mammospheres of MCF7 and MDA-MB-231 (MB231) cells. Conversely, the overexpression of ERRα significantly increased the migration and invasion of BCSCs derived from the mammosphere. In addition, the XCT790 treatment or shERRα significantly downregulated the epithelial-mesenchymal transition (EMT), as evidenced by the downregulation in the expression of vimentin, Snail, Slug and N-cadherin in the mammospheres of MCF7 and MB231 cells. The chorioallantoic membrane assay showed that the conditioned media from XCT790-treated and shERRα cells significantly inhibited blood vessel formation and vessel length. Furthermore, XCT790 treatment or shERRα also downregulated the expression of molecular markers of angiogenesis, such as VEGF-A and Ang-2 in the mammospheres. Conversely, the overexpression of ERRα in MCF7 cells significantly increased both EMT and angiogenesis. These findings suggest that ERRα inhibits the migration, invasion and angiogenesis of BCSCs, suggesting as a potential target for breast cancer therapy.




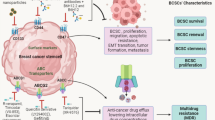
Similar content being viewed by others
Data availability
Data is provided within the manuscript or supplementary information files. Any other data available from the corresponding author upon reasonable request.
Abbreviations
- Ang-2:
-
Angiotensin-2
- BCSC:
-
Breast cancer stem cell
- bFGF:
-
Basic fibroblast growth factor
- CSC:
-
Cancer stem cell
- DMEM:
-
Dulbecco’s modified eagle medium
- EGF:
-
Epidermal growth factor
- ER:
-
Estrogen receptor
- ERRα:
-
Estrogen-related receptor alpha
- EMT:
-
Epithelial-mesenchymal transition
- FBS:
-
Fetal bovine serum
- FITC:
-
Fluorescein isothiocyanate
- HER2:
-
Human epidermal growth factor receptor 2
- L15:
-
Leibovitz 15
- MB231:
-
MDA-MB-231
- MFE:
-
Mammosphere forming efficiency
- TNBC:
-
Triple-negative breast cancer
- VEGF:
-
Vascular endothelial growth factor
- XCT790:
-
3-[4-(2,4-Bis-trifluoromethylbenzyloxy)-3-methoxyphenyl]-2-cyano-N-(5-trifluoromethyl-1,3,4-thiadiazol-2-yl) acrylamide
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49. https://doi.org/10.3322/caac.21660.
Van Mechelen M, Van Herck A, Punie K, Nevelsteen I, Smeets A, Neven P, et al. Behavior of metastatic breast cancer according to subtype. Breast Cancer Res Treat. 2020;181:115–25. https://doi.org/10.1007/s10549-020-05597-3.
van Maaren MC, de Munck L, Strobbe LJA, Sonke GS, Westenend PJ, Smidt ML, et al. Ten-year recurrence rates for breast cancer subtypes in the Netherlands: a large population-based study. Int J Cancer. 2019;144:263–72. https://doi.org/10.1002/ijc.31914.
Welch DR, Hurst DR. Defining the hallmarks of metastasis. Cancer Res. 2019;79:3011–27. https://doi.org/10.1158/0008-5472.CAN-19-0458.
Ayob A, Ramasamy TS. Cancer stem cells as key drivers of tumour progression. J Biomed Sci. 2018;25:20. https://doi.org/10.1186/s12929-018-0426-4.
Babaei G, Aziz SGG, Jaghi NZZ. EMT, cancer stem cells and autophagy; the three main axes of metastasis. Biomed Pharmacother. 2021;133:110909. https://doi.org/10.1016/J.BIOPHA.2020.110909.
Wang D, Lu P, Zhang H, Luo M, Zhang X, Wei X, et al. Oct-4 and nanog promote the epithelial-mesenchymal transition of breast cancer stem cells and are associated with poor prognosis in breast cancer patients. Oncotarget. 2014;5:10803–15. https://doi.org/10.18632/oncotarget.2506.
Ayoub NM, Jaradat SK, Al-Shami KM, Alkhalifa AE. Targeting angiogenesis in breast cancer: current evidence and future perspectives of novel anti-angiogenic approaches. Front Pharmacol. 2022;13:838133. https://doi.org/10.3389/FPHAR.2022.838133/BIBTEX.
Fantozzi A, Gruber DC, Pisarsky L, Heck C, Kunita A, Yilmaz M, et al. VEGF-mediated angiogenesis links EMT-induced cancer stemness to tumor initiation. Cancer Res. 2014;74:1566–75. https://doi.org/10.1158/0008-5472.CAN-13-1641.
Liu Y, Ma H, Yao J. ERα, a key target for cancer therapy: a review. Onco Targets ther. 2020;21:13:2183–91. https://doi.org/10.2147/OTT.S236532.
Deblois G, Giguère V. Oestrogen-related receptors in breast cancer: control of cellular metabolism and beyond. Nat Rev Cancer. 2013;13:27–36. https://doi.org/10.1038/NRC3396.
Manna S, Bostner J, Sun Y, Miller LD, Alayev A, Schwartz NS, et al. ERRα is a marker of tamoxifen response and survival in triple-negative breast cancer. Clin Cancer Res. 2016;22:1421–31. https://doi.org/10.1158/1078-0432.CCR-15-0857.
Ma JH, Qi J, Lin SQ, Zhang CY, Liu FY, Xie WD, et al. STAT3 targets ERRα to promote epithelial–mesenchymal transition, migration, and invasion in triple-negative breast cancer cells. Mol Cancer Res. 2019;17:2184–95. https://doi.org/10.1158/1541-7786.MCR-18-1194.
Suzuki T, Miki Y, Moriya T, Shimada N, Ishida T, Hirakawa H, et al. Estrogen-related receptor α in human breast carcinoma as a potent prognostic factor. Cancer Res. 2004;64:4670–76. https://doi.org/10.1158/0008-5472.CAN-04-0250.
Stein RA, Chang C, Kazmin DA, Way J, Schroeder T, Wergin M, et al. Estrogen-related receptor α is critical for the growth of estrogen receptor–negative breast cancer. Cancer Res. 2008;68:8805–12. https://doi.org/10.1158/0008-5472.CAN-08-1594.
Bianco S, Lanvin O, Tribollet V, Macari C, North S, Vanacker JM. Modulating estrogen receptor-related receptor-α activity inhibits cell proliferation. J Biol Chem. 2009;284:23286–92. https://doi.org/10.1074/JBC.M109.028191.
Wu YM, Chen ZJ, Liu H, Wei WD, Lu LL, Yang XL, et al. Inhibition of ERRα suppresses epithelial mesenchymal transition of triple negative breast cancer cells by directly targeting fibronectin. Oncotarget. 2015;6:25588–601. https://doi.org/10.18632/oncotarget.4436.
Berman AY, Manna S, Schwartz NS, Katz YE, Sun Y, Behrmann CA, et al. ERRα regulates the growth of triple-negative breast cancer cells via S6K1-dependent mechanism. Signal Transduct Target Ther. 2017;2:17035. https://doi.org/10.1038/sigtrans.2017.35.
Naik M, Brahma P, Dixit M. A cost-effective and eefficient chick ex-ovo CAM assay protocol to assess angiogenesis. Methods Protoc. 2018;1:19. https://doi.org/10.3390/mps1020019.
Kue CS, Tan KY, Lam ML, Lee HB. Chick embryo chorioallantoic membrane (CAM): an alternative predictive model in acute toxicological studies for anti-cancer drugs. Exp Anim. 2015;64:129–38. https://doi.org/10.1538/expanim.14-0059.
The public health service responds to commonly asked questions. ILAR J. 1991;33(4):68–70. https://doi.org/10.1093/ilar.33.4.68.
Thomas D, Thiagarajan PS, Rai V, Reizes O, Lathia J, Egelhoff T. Increased cancer stem cell invasion is mediated by myosin IIB and nuclear translocation. Oncotarget. 2016;7:47586–92. https://doi.org/10.18632/oncotarget.9896.
Wu Y, Sarkissyan M, Vadgama J. Epithelial-mesenchymal transition and breast cancer. J Clin Med. 2016;5:13. https://doi.org/10.3390/jcm5020013.
Mani SA, Guo W, Liao M-J, Eaton ENg, Ayyanan A, Zhou AY, et al. The epithelial-mesenchymal transition generates cells with properties of stem cells. Cell. 2008;133:704–15. https://doi.org/10.1016/j.cell.2008.03.027.
Chen C, Zhao S, Karnad A, Freeman JW. The biology and role of CD44 in cancer progression: therapeutic implications. J Hematol Oncol. 2018;11:64. https://doi.org/10.1186/S13045-018-0605-5.
Yang L, Shi P, Zhao G, Xu J, Peng W, Zhang J, et al. Targeting cancer stem cell pathways for cancer therapy. Signal Transduct Target Ther. 2020;5:8. https://doi.org/10.1038/s41392-020-0110-5.
Ricci-Vitiani L, Pallini R, Biffoni M, Todaro M, Invernici G, Cenci T, et al. Tumour vascularization via endothelial differentiation of glioblastoma stem-like cells. Nature. 2010;468:824–8. https://doi.org/10.1038/nature09557.
Xiong YQ, Sun HC, Zhang W, Zhu XD, Zhuang PY, Zhang JB, et al. Human hepatocellular carcinoma tumor–derived endothelial cells manifest increased angiogenesis capability and drug resistance compared with normal endothelial cells. Clin Cancer Res. 2009;15:4838–46. https://doi.org/10.1158/1078-0432.CCR-08-2780.
Duan H, Liu Y, Gao Z, Huang W. Recent advances in drug delivery systems for targeting cancer stem cells. Acta Pharm Sin B. 2021;11:55–70. https://doi.org/10.1016/j.apsb.2020.09.016.
Muduli K, Prusty M, Pradhan J, Samal AP, Sahu B, Roy DS, et al. Estrogen-related receptor alpha (ERRα) promotes cancer stem cell-like characteristics in breast cancer. Stem Cell Rev Rep. 2023;19:2807–19. https://doi.org/10.1007/s12015-023-10605-2.
Croker AK, Goodale D, Chu J, Postenka C, Hedley BD, Hess DA, et al. High aldehyde dehydrogenase and expression of cancer stem cell markers selects for breast cancer cells with enhanced malignant and metastatic ability. J Cell Mol Med. 2009;13:2236–52. https://doi.org/10.1111/j.1582-4934.2008.00455.x.
Li W, Ma H, Zhang J, Zhu L, Wang C, Yang Y. Unraveling the roles of CD44/CD24 and ALDH1 as cancer stem cell markers in tumorigenesis and metastasis. Sci Rep. 2017;7:13856. https://doi.org/10.1038/s41598-017-14364-2.
Felcht M, Luck R, Schering A, Seidel P, Srivastava K, Hu J, et al. Angiopoietin-2 differentially regulates angiogenesis through TIE2 and integrin signaling. J Clin Invest. 2012;122:1991–2005. https://doi.org/10.1172/JCI58832.
Acknowledgements
Not applicable.
Funding
This work was supported by the Indian Council of Medical Research (ICMR) (45/30/2020-BIO/BMS), Government of India and Science and Engineering Research Board (SERB), DST (EMR/2016/006964). KM, MP and JP are supported by Research Fellowships from UGC, ICMR and CSIR, respectively, Government of India. We also acknowledge the infrastructure support available through the DBT-BUILDER program (BT/INF/22/SP42155/2021).
Author information
Authors and Affiliations
Contributions
Conceptualization, KM, SE and KSR; methodology, KM, JP, MP, APS and SE; validation, KM, JP, APS and SE; analysis, KM, JP and SE; writing-original draft preparation, KM and SE; writing-review and editing, KM, JP, MP, KSR and SE; supervision, KSR and SE; project administration, SE; funding acquisition, KM and SE. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publish
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Muduli, K., Pradhan, J., Prusty, M. et al. Estrogen-related receptor alpha (ERRα) promotes the migration, invasion and angiogenesis of breast cancer stem cell-like cells. Med Oncol 41, 78 (2024). https://doi.org/10.1007/s12032-024-02329-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12032-024-02329-1