Abstract
Patient education and informed consent are required prior to adjuvant radiation therapy (RT) for early breast cancer (EBC), and include the role, rationale, potential toxicities and practicalities of the treatment process. Current education of patients about RT is verbal, in the form of a consultation by a radiation oncologist, often supplemented with print or online materials. This approach is limited by its doctor-dependency and non-standardised nature. Video education is being recognised increasingly as an opportunity to remediate this and appeal to patients’ preference for visual learning. The purpose of this study was to design and produce a video as an educational adjunct for EBC patients’ viewing prior to adjuvant RT, and to evaluate its acceptability through content analysis of three online focus group discussions, among ten participants with EBC requiring RT. After qualitative content analysis of the focus group transcripts, data were summarised into three main categories: (1) understanding of RT, (2) ease of engagement with the video and (3) anxiety and preparedness for RT. The 18-min video was positively received by all participants, and discussion feedback was used to inform improvements to the video. This focus group study demonstrated that the video was well understood, informative and acceptable to EBC patients in preparing them for RT. The effectiveness of the video in improving knowledge and alleviating distress in preparation for therapy will be further evaluated in an ethics-approved biphasic quasi-experimental study.
Similar content being viewed by others
Introduction
Adjuvant radiation therapy (RT) after breast-conserving reduces the risk of both locoregional and distant recurrence and improves overall survival in women with early breast cancer (EBC) [1, 2]. The uptake of RT can be limited due to its perceived complexity and potential side effects, which warrants that patients attain a minimum baseline understanding of essential information to adequately consent and collaborate through their treatment [3]. Both historically and currently, the most common form of RT education is one-on-one verbal communication with the radiation oncologist (RO) during the initial consultation and is often reinforced with print and occasionally online materials [4]. Surveys of Australian EBC patients have identified informational needs to be highest during the initial RO consultation, where the patient is educated on potential benefits and risks of RT, to provide adequate informed consent [5, 6]. However, verbal education has limitations, including that it is doctor-dependent and non-standardised in quality and depth [4]. Similarly, print and online information is often non-individualised and poorly understood in the presence of language barriers or low health literacy [7, 8]. There has been a rapid expansion of internet-based information wherein breast cancer is the most frequently researched cancer [9], yet a substantial proportion of online information may be inaccurate or irrelevant [5].
Despite the growing importance assigned to RT education in the literature, substantial numbers of EBC patients continue to report unmet informational needs and suboptimal treatment knowledge, particularly relating to side effects of RT [5, 10]. Additionally, the mechanism underpinning RT is not generally familiar to patients, as radiation is a complex concept with limited visual or sensory stimuli [11], so patients may struggle to conceptualise RT or conflate its use with perceived harms [12]. Traditional verbal and print material is often inadequate in capturing this, giving rise to an appetite for modalities that appeal to preferences for visual learning and extend patient education beyond merely a verbal discussion and generic written material [4]. The evolving area of breast cancer RT education literature is increasingly recognising video technology as an opportunity to remediate the limitations of current educational modalities [7, 8, 13, 14].
The objective of this study was to design and produce an educational video to meet the informational needs of EBC patients commencing adjuvant RT at a metropolitan tertiary teaching hospital. Subsequently, the study aimed to evaluate acceptability of the video through content analysis of focus group discussions, to inform improvements to the video.
Methods
Study Overview
This study involved the design and production of a video as an educational adjunct for EBC patients prior to commencing adjuvant RT, with the view to replace part of the standard verbal education delivered during the initial RO consultation. The video underwent qualitative evaluation by content analysis of three focus group discussions among EBC patients commencing RT. Study approval was obtained from the Western Sydney Local Health District (WSLHD) Human Research Ethics Committee (Number 2021: ETH12077).
Video Development
Video development occurred in three phases: pre-production, production and post-production, summarised in Fig. 1. To maximise authenticity and familiarity, all staff and filming locations were within the Westmead Breast Cancer Institute (WBCI) or Crown Princess Mary Cancer Centre Westmead (CPMCCW). Production and post-production services were completed by the WSLHD Corporate Communications. Simulations of RT apparatuses and imperceptible concepts such as radiation and internal patient anatomy were procured using Virtual Environment for Radiotherapy Training (VERT) software (version 2.9) [15]. The video covered the 30-item Knowledge of RT scale identified as seminal by the “RT Prepare” study [16]. Table 1 provides an overview of the 18-min video.
Summary of steps in pre-production, production and post-production of video. Abbreviations: RO, radiation oncologist; K-RT, Knowledge of Radiation Therapy; MD, Doctor of Medicine; WSLHD, Western Sydney Local Health District; VERT, Virtual Environment for Radiotherapy Training; DIBH, Deep Inspiration Breath Hold
Participant Recruitment
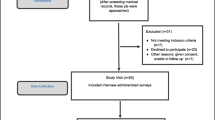
Convenience sampling was used to recruit EBC patients presenting to WBCI or CPMCCW between March and June 2022 for their initial RO consultation, into three focus groups of three to four participants each. Eligible women were aged > 18 years, with sufficient English language proficiency, hearing and vision, diagnosed with unilateral EBC and scheduled to receive standard adjuvant RT in 15–25 fractions after breast-conserving surgery. Patients with a prior history of RT, mastectomy, breast reconstruction, significant active psychiatric disorder or who were pregnant, lactating or deemed unsuitable by their clinician were ineligible. Eligible patients were provided information by their Breast RO and invited to participate, after RT consent but prior to RT commencement. Ethics approval included trial consent on day of RT consent, provided sufficient time was allowed for trial consideration, or later, prior to RT. Participants with written informed trial consent viewed an online screening of the video, immediately prior to focus group discussions, which were held via Zoom due to COVID-19.
Data Collection
Immediately after providing informed consent, trial participants were asked to complete a brief questionnaire to obtain demographic information and quantify their level of distress using the National Comprehensive Cancer Network’s Distress Thermometer. Clinical data about their EBC, treatment regimen and Eastern Co-operative Oncology Group (ECOG) performance status, were collected from medical records. For staging of EBC, the American Joint Committee on Cancer’s Tumour, Node, Metastases (TNM) system was used. All participant data were de-identified and input into Excel™. Every three or four participants were grouped in order of recruitment into one of three focus groups. The approximately 30-min-long focus group discussions were facilitated and audio-recorded via Zoom. The discussion was moderated by author YM, supervised by YJ, with prompts stimulating reflection on video effectiveness pertaining to understanding of RT, anxiety, preparedness and ease of engagement. Audio recordings were transcribed verbatim.
Data Analysis
Demographic data were descriptively grouped into categories. Excel™ was used to produce descriptive statistics to represent participant data as percentages and means. Once accurate transcriptions of focus groups were confirmed, they were uploaded onto NVivo (QSR-International), a qualitative data management and coding software. Digital recordings were deleted. Data were analysed by content analysis, wherein transcripts were reviewed line-by-line by two authors independently, generating initial codes that were then further synthesised into meaningful code categories. The final analysis was completed by two authors (YM, YJ) independently and discussed until consensus reached.
Results
Participants
Ten women participated in three focus groups between May and July 2022, with four participants in the initial group, and three in both latter groups. Mean age of the women was 62 years (range 43–74 years). Most women were married or in a de-facto relationship (90%), and all resided within surrounding suburbs of our metropolitan hospital. While all participants were English-speaking, 30% spoke an additional language at home and 40% were born overseas. Employment statuses included full-time (30%), part-time (10%), retired (30%) and other work (30%), including volunteering and homemaker roles. The highest level of education attained ranged from school certificate or diploma qualifications (60%) to higher school certificate (20%) and university education (20%). All women were ECOG 0–1. The participants’ EBCs were left-sided for 70%, while 30% were right-sided. The majority of tumours were T1 (60%), with the remainder T2 (20%) and Tis (20%); all tumours were N0. Additionally, 70% of women reported low distress scores of ≤ 3, and 30% reported distress scores ≥ 4. None received chemotherapy. Participant demographic and clinical data are summarised (Online Resource 1).
Focus Group Findings
After analysis of the focus group transcripts, codes emerged under three main categories: (1) understanding of RT, (2) ease of engagement with video and (3) anxiety and preparedness for RT. These categories, as well as the codes within them and supportive direct quotes, are presented in Table 2.
Understanding of RT
The category of understanding of RT included four main codes: improved understanding and expectations, learning new information, the video as a complement to other information sources and clarity of video content. Although most participants acknowledged they had some understanding of RT after their initial RO consultation, viewing the video enhanced most women’s understanding of RT. In particular, participants found the level of detail and step-by-step explanation improved understanding and provided expectations. There was also an appreciation of the ability to visualise the size and motion of the linear accelerator. Most participants found the video content to be clear, but two participants raised that the explanation of the typical weekly RT schedule and machine service was fast-paced and not articulated clearly. While some participants felt the video alone could have replaced hours of independent research and conversation with the RO, most women appreciated the video as a complement to other educational modalities.
Ease of Engagement with Video
The category of ease of engagement with the video included three main codes: usefulness of graphics in representing concepts, appropriateness of video duration and pace and appropriateness of vocabulary. All participants appreciated the incorporation of graphics, with some women attributing this to the appeal of visual modes of learning. Participants were satisfied with the length and thoroughness of the video. However, while most felt the video was appropriately paced, some expressed that parts were fast-paced and would benefit from watching the video multiple times. All participants felt that the video language was understandable and pitched at an appropriate level.
Anxiety and Preparedness for RT
Feedback regarding the effect of the video on anxiety and preparedness for RT included four codes of reduced anxiety towards RT, increased feelings of preparedness, changes in level of concern regarding RT and unanswered questions remaining around RT. Participants expressed that the video reduced their anxiety and made them feel increasingly prepared for RT. Some women who had already commenced RT expressed that seeing the video previously would have reduced their apprehension. After viewing the video, most participants felt their level of concern regarding RT had decreased or remained unchanged; one participant found the listing of side effects made her more concerned about starting RT. While most women felt the video comprehensively answered their questions, some women expressed uncertainty around contracting COVID-19 during treatment, consequences of missed RT sessions, differences in completing RT at other WSLHD hospitals and what follow-up and imaging are indicated after treatment completion.
General Positive and Other Reactions to Video
Among the three focus group discussions, the video was positively received by all ten participants, and all would recommend it to other women commencing RT. The focus groups suggested improvements, such as incorporating statistics on RT efficacy. Also, with the volume of information being provided, participants felt it would be beneficial to have external access to the video and share it with family members.
Discussion
This study qualitatively evaluated the acceptability and effectiveness of a breast cancer RT video designed to educate and facilitate informed consent during the initial RO consultation. The video modality provides an approach to standardising depth and quality of the plethora of information that EBC patients encounter. Reception was largely positive with regard to ease of engagement with the video, its ability to improve understanding of RT and increase feelings of preparedness. The multi-modal incorporation of visual, auditory and written stimuli within the video appealed to participants, allowing the portrayal of abstract concepts such as radiation. To accommodate the low health literacy noted in 60% of Australian adults, the video was tailored to an eighth-grade level [17]. The video also balanced comprehensiveness and succinctness, with its duration within the typical range documented in the literature of 16–25 min, and being shorter than the standard RO verbal consultation of up to 40 min, amongst the practice of the RO authors.
The positive reception to this video is consistent with the growing body of evidence supporting video education in breast cancer RT education literature. Several recent studies have demonstrated educational videos to be a superior form of breast cancer RT education, leading to substantial improvements in patient self-reported knowledge [7, 8, 13], post-consult anxiety [7, 8, 13, 14], heightened confidence in providers [7] and better decision-making [7]. However, of these studies, only one single-arm study of 20 participants targeted the initial RO consult and reported the 7.5-min video to be a feasible intervention that decreased patient-reported anxiety [14]. Our study is the first to incorporate VERT simulations into a breast cancer RT educational video that is intended to be viewed by patients during an initial RO consultation. VERT-based education sessions have reliably demonstrated improvement of RT knowledge in EBC patients [18].
Although the majority of feedback was positive in nature, the discussions generated several insightful suggestions prompting the team to consider minor enhancements to optimise the video. These include subtitling the video to improve understandability, translating versions, and creating alternative versions with accessibility information for other WSLHD hospitals. Other suggestions were difficult to action, such as addressing the effect of COVID-19 on RT treatment despite being valid and pertinent, as policies and procedures are frequently changing. As such, it would be optimal to seek specific advice based on contemporary local policy. Similarly, patient-specific questions on follow-up imaging after RT completion or statistical recurrence risk data would be better suited to discussion with the RO after viewing the video.
There were challenges and limitations encountered in this study, some of which are inherent to focus group methodology. One potential limitation is that of volunteer bias, wherein volunteers may be systematically different to the general breast cancer population [19]. This may have further been compounded by the inclusion criteria for English proficiency. However, this study captured women across a range of ages, educational levels and linguistic backgrounds. Similarly, the phenomenon of group bias arises in focus groups, wherein participants may opt to maintain group consensus rather than present their true opinion. Overall, the focus group methodology was conducive to the aim of gathering preliminary feedback on the newly created video. Although a face-to-face format would have been preferred due to non-verbal communication and visual cues [20], Zoom emerged as a non-inferior alternative during COVID-19 [21]. The pandemic also saw delays in participant recruitment, which limited this study to three focus groups. The smaller groups not only facilitated equal discussion opportunities among participants, but are substantiated by previous work demonstrating 80% of discussion themes are discoverable within two to three focus groups [22]. Another challenge was creating a video specific enough to educate and answer patient questions but general enough to maintain relevance to most patients. Hence, two additional video modules were created to be integrated into the core video for specific patient groups with lymph node involvement or left-sided cancers.
In the future, the video will be further evaluated within an ethics-approved biphasic quasi-experimental pilot trial. The trial will assess knowledge of RT and evaluate levels of anxiety and distress in EBC patients, who will receive at the initial RO consultation either standard education, or have part of the standard education replaced by this video in addition to the residual standard education and individual patient-specific information. If benefit from video education is demonstrated in the pilot trial over standard practice, this research has the potential to enhance standard EBC RT education at the initial RO consultation. Multimedia-based interventions are cost-effective [23], time-efficient [24] and allow the delivery of high-quality education remotely. Further efforts will be required to extend the generalisability of this video to include patients from culturally and linguistically diverse backgrounds, and other health areas.
Conclusions
An educational video was created for EBC patients prior to commencing RT, to replace part of the standard verbal education offered during the initial RO consultation, to be followed immediately by an individualised discussion with the RO. This video was qualitatively reviewed with content analysis after focus group discussions within this population. The video was positively received in terms of engagement, ability to improve understanding, alleviate anxiety and increase preparedness for RT.
Data Availability
Research data are not available at this time.
Code Availability
No.
References
Haussmann J, Corradini S, Nestle-Kraemling C, Bölke E, Freddy Joel Djiepmo N, Tamaskovics B et al (2020) Recent advances in radiotherapy of breast cancer. Radiat Oncol J 15:1–10
Darby S, McGale P, Correa C, Taylor C, Arriagada R, Clarke M et al (2011) Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet 378:1707–1716
Waller A, Forshaw K, Bryant J, Mair S (2014) Interventions for preparing patients for chemotherapy and radiotherapy: a systematic review. Support Care Cancer 22:2297–2308
Savage K, Arif S, Smoke M, Farrell T (2017) Preferences in learning styles and modes of information delivery in patients receiving first-day education for radiation therapy. J Med Imaging Radiat Sci 48:193–198
Halkett GK, Kristjanson LJ, Lobb E, Little J, Shaw T, Taylor M et al (2012) Information needs and preferences of women as they proceed through radiotherapy for breast cancer. Patient Educ Couns 86:396–404
Halkett GK, Kristjanson LJ, Lobb E, O’Driscoll C, Taylor M, Spry N (2010) Meeting breast cancer patients’ information needs during radiotherapy: what can we do to improve the information and support that is currently provided? Eur J Cancer 19:538–547
Sulakvelidze N, Burdick B, Kaklamani V, Tilton K, Baker K, Kim J et al (2019) Evaluating the effect of a video education curriculum for first time breast cancer patients: a prospective RCT feasibility study. J Cancer Educ 34:1234–1240
Kumar KA, Balazy KE, Gutkin PM, Jacobson CE, Chen JJ, Karl JJ et al (2021) Association between patient education videos and knowledge of radiation treatment. Int J Radiat Oncol Biol Phys 109:1165–1175
McHugh SM, Corrigan M, Morney N, Sheikh A, Lehane E, Hill AD (2011) A quantitative assessment of changing trends in internet usage for cancer information. World J Surg 35:253–257
Bolderston A (2008) Mixed messages? A comparison between the perceptions of radiation therapy patients and radiation therapists regarding patients’ educational needs. Radiography 14:111–119
Jimenez YA, Wang W, Stuart K, Cumming S, Thwaites D, Lewis S (2018) Breast cancer patients’ perceptions of a virtual learning environment for pretreatment education. J Cancer Educ 33:983–990
Lewis SJ (2015) Finding my own voice through the breast cancer journey: humour, sadness and smurfs. J Med Radiat Sci 62:82–85
Islam T, Musthaffa S, Hoong SM, Filza J, Jamaris S, Cheng ML et al (2020) Development and evaluation of a sustainable video health education program for newly diagnosed breast cancer patients in Malaysia. Support Care Cancer 29:2631–2638
Pembroke M, Bradley J, Mueller M, Mollica M, Nemeth LS (2021) Feasibility of breast radiation therapy video education combined with standard radiation therapy education for patients with breast cancer. Oncol Nurs Forum 48:279–290
Jimenez YA, Lewis SJ (2018) Radiation therapy patient education review and a case study using the virtual environment for radiotherapy training system. J Med Imaging Radiat Sci 49:106–117
Halkett G, O’Connor M, Aranda S, Jefford M, Spry N, Shaw T et al (2014) Protocol for the RT prepare trial: a multiple-baseline study of radiation therapists delivering education and support to women with breast cancer who are referred for radiotherapy. BMJ Open:. https://doi.org/10.1136/bmjopen-2014-006116
Oliffe M, Thompson E, Johnston J, Freeman D, Bagga H, Wong PKK (2019) Assessing the readability and patient comprehension of rheumatology medicine information sheets: a cross-sectional health literacy study. BMJ Open:. https://doi.org/10.1136/bmjopen-2018-024582
Jimenez YA, Cumming S, Wang W, Stuart K, Thwaites DI, Lewis SJ (2018) Patient education using virtual reality increases knowledge and positive experience for breast cancer patients undergoing radiation therapy. Support Care Cancer 26:2879–2888
Nyumba T, Wilson K, Derrick CJ, Mukherjee N (2018) The use of focus group discussion methodology: insights from two decades of application in conservation. Methods Ecol Evol 9:20–32
Tausch AP, Menold N (2016) Methodological aspects of focus groups in health research: results of qualitative interviews with focus group moderators. Glob Qual Nurs Res 3:1–12
Dos Santos Marques IC, Theiss LM, Johnson CY, McLin E, Ruf BA, Vickers SM et al (2021) Implementation of virtual focus groups for qualitative data collection in a global pandemic. Am J Surg 221:918–922
Guest G, Namey E, McKenna K (2016) How many focus groups are enough? Building an evidence base for nonprobability sample sizes. Field Methods 29:3–22
Jones GE, Singletary JH, Cashmore A, Jain V, Abhulimhen J, Chauhan J et al (2016) Developing and assessing the utility of a You-Tube based clinical genetics video channel for families affected by inherited tumours. Fam Cancer 15:351–355
Lam M, Choi M, Lam HR, Agarwal A, Chow R, Chow S et al (2017) Use of multimedia in patient and caregiver education for cancer pain management: a literature review. Ann Palliat Med 6:66–72
Acknowledgements
This research was supported by the Westmead Breast Cancer Institute, Crown Princess Mary Cancer Centre and assisted by the WSLHD Corporate Communications Team in producing and editing the video. We thank A/Prof. Georgia Halkett for providing input during the initial stages of the project and The University of Sydney for access to VERT simulation software.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions Any costs related to submission of manuscript funded by our Cancer Network Radiation Oncology Trust Fund. The production of the video was supported by our hospital. No other funding sources to declare.
Author information
Authors and Affiliations
Contributions
Study conception and design was completed by A/Prof. Kirsty Stuart, Dr Yobelli Jimenez and Yvonne Moussa, with the assistance of all other authors. Video preparation and creation involved all authors. Data collection and analysis were performed by A/Prof. Kirsty Stuart, Dr Yobelli Jimenez and Yvonne Moussa. The first draft of the manuscript was written by Yvonne Moussa. All authors commented on previous versions of the manuscript, and read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Approval for this study was obtained from the Western Sydney Local Health District (LHD) Human Research Ethics Committee (Number 2021: ETH12077).
Consent to Participate
Informed consent was provided by all participants included in the study.
Consent for Publication
The authors affirm that research participants provided informed consent for publication of de-identified data and focus group findings.
Conflict of Interest
The authors declare no competing interests.
Disclaimer
The content of this paper is the responsibility of the authors and does not necessarily represent the official views of the Westmead Breast Cancer Institute or The University of Sydney.
Additional information
Meeting Presentation Information: This study has not been presented at a meeting.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Moussa, Y., Jimenez, Y., Wang, W. et al. The Development and Evaluation of an Educational Video for Breast Cancer Patients Requiring Adjuvant Radiation Therapy. J Canc Educ (2024). https://doi.org/10.1007/s13187-024-02408-x
Accepted:
Published:
DOI: https://doi.org/10.1007/s13187-024-02408-x