Abstract
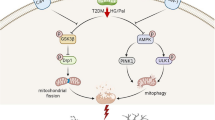
Cognitive impairment is considered to be one of the important comorbidities of diabetes, but the underlying mechanisms are widely unknown. Aquaporin-4 (AQP4) is the most abundant water channel in the central nervous system, which plays a neuroprotective role in various neurological diseases by maintaining the function of glymphatic system and synaptic plasticity. However, whether AQP4 is involved in diabetes-related cognitive impairment remains unknown. β-dystroglycan (β-DG), a key molecule for anchoring AQP4 on the plasma membrane of astrocytes and avoiding its targeting to lysosomes for degradation, can be cleaved by matrix metalloproteinase-9 (MMP-9). β-DG deficiency can cause a decline in AQP4 via regulating its endocytosis. However, whether cleavage of β-DG can affect the expression of AQP4 remains unreported. In this study, we observed that diabetes mice displayed cognitive disorder accompanied by reduction of AQP4 in prefrontal cortex. And we found that bafilomycin A1, a widely used lysosome inhibitor, could reverse the downregulation of AQP4 in diabetes, further demonstrating that the reduction of AQP4 in diabetes is a result of more endocytosis-lysosome degradation. In further experiments, we found diabetes caused the excessive activation of MMP-9/β-DG which leaded to the loss of connection between AQP4 and β-DG, further inducing the endocytosis of AQP4. Moreover, inhibition of MMP-9/β-DG restored the endocytosis-lysosome degradation of AQP4 and partially alleviated cognitive dysfunction in diabetes. Our study sheds new light on the role of AQP4 in diabetes-associated cognitive disorder. And we provide a promising therapeutic target to reverse the endocytosis-lysosome degradation of AQP4 in diabetes, such as MMP-9/β-DG.







Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Biessels GJ, Staekenborg S, Brunner E, Brayne C, Scheltens P (2006) Risk of dementia in diabetes mellitus: a systematic review. Lancet Neurol 5(1):64–74
Diniz Pereira J, Gomes Fraga V, Morais Santos AL, Carvalho MDG, Caramelli P, Braga Gomes K (2021) Alzheimer’s disease and type 2 diabetes mellitus: a systematic review of proteomic studies. J Neurochem 156(6):753–776. https://doi.org/10.1111/jnc.15166
Puig KL, Floden AM, Adhikari R, Golovko MY, Combs CK (2012) Amyloid precursor protein and proinflammatory changes are regulated in brain and adipose tissue in a murine model of high fat diet-induced obesity. PloS One 7(1):e30378. https://doi.org/10.1371/journal.pone.0030378
Liu Y, Liu L, Lu S, Wang D, Liu X, Xie L, Wang G (2011) Impaired amyloid β-degrading enzymes in brain of streptozotocin-induced diabetic rats. J Endocrinol Invest 34(1):26–31
Harrison IF, Ismail O, Machhada A, Colgan N, Ohene Y, Nahavandi P, Ahmed Z, Fisher A et al (2020) Impaired glymphatic function and clearance of tau in an Alzheimer’s disease model. Brain 143(8):2576–2593. https://doi.org/10.1093/brain/awaa179
Nielsen S, Nagelhus EA, Amiry-Moghaddam M, Bourque C, Agre P, Ottersen OP (1997) Specialized membrane domains for water transport in glial cells: high-resolution immunogold cytochemistry of aquaporin-4 in rat brain. J Neurosci 17(1):171–180
Rash JE, Yasumura T, Hudson CS, Agre P, Nielsen S (1998) Direct immunogold labeling of aquaporin-4 in square arrays of astrocyte and ependymocyte plasma membranes in rat brain and spinal cord. Proc Natl Acad Sci USA 95(20):11981–11986
Zeppenfeld DM, Simon M, Haswell JD, D’Abreo D, Murchison C, Quinn JF, Grafe MR, Woltjer RL et al (2017) Association of perivascular localization of aquaporin-4 with cognition and Alzheimer disease in aging brains. JAMA Neurol 74(1):91–99. https://doi.org/10.1001/jamaneurol.2016.4370
Reeves BC, Karimy JK, Kundishora AJ, Mestre H, Cerci HM, Matouk C, Alper SL, Lundgaard I et al (2020) Glymphatic system impairment in Alzheimer’s disease and idiopathic normal pressure hydrocephalus. Trends In Mol Med 26(3):285–295. https://doi.org/10.1016/j.molmed.2019.11.008
Si X, Dai S, Fang Y, Tang J, Wang Z, Li Y, Song Z, Chen Y, et al (2024) Matrix metalloproteinase-9 inhibition prevents aquaporin-4 depolarization-mediated glymphatic dysfunction in Parkinson’s disease. J Ad Res 15(56):125–136.https://doi.org/10.1016/j.jare.2023.03.004
Zhao F, Deng J, Xu X, Cao F, Lu K, Li D, Cheng X, Wang X et al (2018) Aquaporin-4 deletion ameliorates hypoglycemia-induced BBB permeability by inhibiting inflammatory responses. J Neuroinflammation. 15(1):157. https://doi.org/10.1186/s12974-018-1203-8
Nagelhus EA, Ottersen OP (2013) Physiological roles of aquaporin-4 in brain. Physiol Rev 93(4):1543–1562. https://doi.org/10.1152/physrev.00011.2013
Hubbard JA, Szu JI, Binder DK (2018) The role of aquaporin-4 in synaptic plasticity, memory and disease. Brain Res Bull 136:118–129. https://doi.org/10.1016/j.brainresbull.2017.02.011
Liu Y, Hu P-P, Zhai S, Feng W-X, Zhang R, Li Q, Marshall C, Xiao M et al (2022) Aquaporin 4 deficiency eliminates the beneficial effects of voluntary exercise in a mouse model of Alzheimer’s disease. Neural Regen Res 17(9):2079–2088. https://doi.org/10.4103/1673-5374.335169
Liu L, Lu Y, Kong H, Li L, Marshall C, Xiao M, Ding J, Gao J et al (2012) Aquaporin-4 deficiency exacerbates brain oxidative damage and memory deficits induced by long-term ovarian hormone deprivation and D-galactose injection. Int J Neuropsychopharmacol 15(1):55–68. https://doi.org/10.1017/S1461145711000022
Li Y-K, Wang F, Wang W, Luo Y, Wu P-F, Xiao J-L, Hu Z-L, Jin Y et al (2012) Aquaporin-4 deficiency impairs synaptic plasticity and associative fear memory in the lateral amygdala: involvement of downregulation of glutamate transporter-1 expression. Neuropsychopharmacology 37(8):1867–1878. https://doi.org/10.1038/npp.2012.34
Pei L, Yang G, Jiang J, Jiang R, Deng Q, Chen B, Gan X (2013) Expression of aquaporins in prostate and seminal vesicles of diabetic rats. J Sexual Med 10(12):2975–2985. https://doi.org/10.1111/jsm.12276
Wang T, Zhang C, Xie H, Jiang M, Tian H, Lu L, Xu G-T, Liu L et al (2021) Anti-VEGF therapy prevents Müller intracellular edema by decreasing VEGF-A in diabetic retinopathy. Eye Vision (London, England) 8(1):13. https://doi.org/10.1186/s40662-021-00237-3
Zanotto C, Simão F, Gasparin MS, Biasibetti R, Tortorelli LS, Nardin P, Gonçalves C-A (2017) Exendin-4 reverses biochemical and functional alterations in the blood-brain and blood-CSF barriers in diabetic rats. Mol Neurobiol 54(3):2154–2166. https://doi.org/10.1007/s12035-016-9798-1
Del Puerto A, Pose-Utrilla J, Simón-García A, López-Menéndez C, Jiménez AJ, Porlan E, Pajuelo LSM, Cano-García G et al (2021) Kidins220 deficiency causes ventriculomegaly via SNX27-retromer-dependent AQP4 degradation. Mol Psychiatry 26(11):6411–6426. https://doi.org/10.1038/s41380-021-01127-9
Madrid R, Le Maout S, Barrault MB, Janvier K, Benichou S, Mérot J (2001) Polarized trafficking and surface expression of the AQP4 water channel are coordinated by serial and regulated interactions with different clathrin-adaptor complexes. EMBO J 20(24):7008–7021
Hinson SR, Clift IC, Luo N, Kryzer TJ, Lennon VA (2017) Autoantibody-induced internalization of CNS AQP4 water channel and EAAT2 glutamate transporter requires astrocytic Fc receptor. Proc National Acad Sci United States Am 114(21):5491–5496. https://doi.org/10.1073/pnas.1701960114
Ratelade J, Bennett JL, Verkman AS (2011) Evidence against cellular internalization in vivo of NMO-IgG, aquaporin-4, and excitatory amino acid transporter 2 in neuromyelitis optica. J Biol Chem 286(52):45156–45164. https://doi.org/10.1074/jbc.M111.297275
Kitchen P, Salman MM, Halsey AM, Clarke-Bland C, MacDonald JA, Ishida H, Vogel HJ, Almutiri S et al (2020) Targeting aquaporin-4 subcellular localization to treat central nervous system edema. Cell 181:4. https://doi.org/10.1016/j.cell.2020.03.037
Waite A, Brown SC, Blake DJ (2012) The dystrophin-glycoprotein complex in brain development and disease. Trends Neurosci 35(8):487–496. https://doi.org/10.1016/j.tins.2012.04.004
Tham DKL, Joshi B, Moukhles H (2016) Aquaporin-4 cell-surface expression and turnover are regulated by dystroglycan, dynamin, and the extracellular matrix in astrocytes. PloS One 11(10):e0165439. https://doi.org/10.1371/journal.pone.0165439
Sato J, Horibe S, Kawauchi S, Sasaki N, Hirata K-I, Rikitake Y (2018) Involvement of aquaporin-4 in laminin-enhanced process formation of mouse astrocytes in 2D culture: roles of dystroglycan and α-syntrophin in aquaporin-4 expression. J Neurochem 147(4):495–513. https://doi.org/10.1111/jnc.14548
Noell S, Wolburg-Buchholz K, Mack AF, Beedle AM, Satz JS, Campbell KP, Wolburg H, Fallier-Becker P (2011) Evidence for a role of dystroglycan regulating the membrane architecture of astroglial endfeet. Eur J Neurosci 33(12):2179–2186. https://doi.org/10.1111/j.1460-9568.2011.07688.x
Zitka O, Kukacka J, Krizkova S, Huska D, Adam V, Masarik M, Prusa R, Kizek R (2010) Matrix metalloproteinases. Curr Med Chem 17(31):3751–3768
Rohani MG, Parks WC (2015) Matrix remodeling by MMPs during wound repair. Matrix Biology : Journal of the International Society For Matrix Biology 36(44–46):113–121. https://doi.org/10.1016/j.matbio.2015.03.002
Vafadari B, Salamian A, Kaczmarek L (2016) MMP-9 in translation: from molecule to brain physiology, pathology, and therapy. J Neurochem 139(Suppl):2. https://doi.org/10.1111/jnc.13415
Stawarski M, Stefaniuk M, Wlodarczyk J (2014) Matrix metalloproteinase-9 involvement in the structural plasticity of dendritic spines. Front Neuroanat 8:68. https://doi.org/10.3389/fnana.2014.00068
Bozzi M, Sciandra F, Brancaccio A (2015) Role of gelatinases in pathological and physiological processes involving the dystrophin-glycoprotein complex. Matrix Biol 36(44–46):130–137. https://doi.org/10.1016/j.matbio.2015.02.005
Yamada H, Saito F, Fukuta-Ohi H, Zhong D, Hase A, Arai K, Okuyama A, Maekawa R et al (2001) Processing of beta-dystroglycan by matrix metalloproteinase disrupts the link between the extracellular matrix and cell membrane via the dystroglycan complex. Hum Mol Genet 10(15):1563–1569
Michaluk P, Kolodziej L, Mioduszewska B, Wilczynski GM, Dzwonek J, Jaworski J, Gorecki DC, Ottersen OP et al (2007) Beta-dystroglycan as a target for MMP-9, in response to enhanced neuronal activity. J Biol Chem 282(22):16036–16041
Wang H, Yuan M, Yang E, Chen D, Su A, Wu Z (2021) Enterovirus 71 infection induced Aquaporin-4 depolarization by increasing matrix metalloproteinase-9 activity. Neurosci Lett 759:136049. https://doi.org/10.1016/j.neulet.2021.136049
Rao KVR, Reddy PVB, Curtis KM, Norenberg MD (2011) Aquaporin-4 expression in cultured astrocytes after fluid percussion injury. J Neurotrauma 28(3):371–381. https://doi.org/10.1089/neu.2010.1705
Mauvezin C, Neufeld TP (2015) Bafilomycin A1 disrupts autophagic flux by inhibiting both V-ATPase-dependent acidification and Ca-P60A/SERCA-dependent autophagosome-lysosome fusion. Autophagy 11(8):1437–1438. https://doi.org/10.1080/15548627.2015.1066957
Wilczynski GM, Konopacki FA, Wilczek E, Lasiecka Z, Gorlewicz A, Michaluk P, Wawrzyniak M, Malinowska M et al (2008) Important role of matrix metalloproteinase 9 in epileptogenesis. J Cell Biol 180(5):1021–1035. https://doi.org/10.1083/jcb.200708213
Wang Y, Huang C, Guo Q, Chu H (2022) Aquaporin-4 and cognitive disorders. Aging Dis 13(1):61–72. https://doi.org/10.14336/AD.2021.0731
Xue X, Zhang W, Zhu J, Chen X, Zhou S, Xu Z, Hu G, Su C (2019) Aquaporin-4 deficiency reduces TGF-β1 in mouse midbrains and exacerbates pathology in experimental Parkinson’s disease. J Cellular MolMed 23(4):2568–2582. https://doi.org/10.1111/jcmm.14147
Shi W-Z, Zhao C-Z, Zhao B, Shi Q-J, Zhang L-H, Wang Y-F, Fang S-H, Lu Y-B et al (2012) Aggravated inflammation and increased expression of cysteinyl leukotriene receptors in the brain after focal cerebral ischemia in AQP4-deficient mice. Neurosci Bull 28(6):680–692. https://doi.org/10.1007/s12264-012-1281-z
Skucas VA, Mathews IB, Yang J, Cheng Q, Treister A, Duffy AM, Verkman AS, Hempstead BL et al (2011) Impairment of select forms of spatial memory and neurotrophin-dependent synaptic plasticity by deletion of glial aquaporin-4. J Neurosci 31(17):6392–6397. https://doi.org/10.1523/JNEUROSCI.6249-10.2011
Ishida K, Yamada K, Nishiyama R, Hashimoto T, Nishida I, Abe Y, Yasui M, Iwatsubo T (2022) Glymphatic system clears extracellular tau and protects from tau aggregation and neurodegeneration. J Exp Med 219:3. https://doi.org/10.1084/jem.20211275
Saadoun S, Bell BA, Verkman AS, Papadopoulos MC (2008) Greatly improved neurological outcome after spinal cord compression injury in AQP4-deficient mice. Brain 131(Pt 4):1087–1098. https://doi.org/10.1093/brain/awn014
Hinson SR, Pittock SJ, Lucchinetti CF, Roemer SF, Fryer JP, Kryzer TJ, Lennon VA (2007) Pathogenic potential of IgG binding to water channel extracellular domain in neuromyelitis optica. Neurology 69(24):2221–2231
Navaratna D, Fan X, Leung W, Lok J, Guo S, Xing C, Wang X, Lo EH (2013) Cerebrovascular degradation of TRKB by MMP9 in the diabetic brain. J Clin Investig 123(8):3373–3377. https://doi.org/10.1172/JCI65767
Wu L, Zhang K, Sun L, Bai J, Zhang M, Zheng J (2020) Laminin degradation by matrix metalloproteinase 9 promotes ketamine-induced neuronal apoptosis in the early developing rat retina. CNS Neurosci Ther 26(10):1058–1068. https://doi.org/10.1111/cns.13428
Moore SA, Saito F, Chen J, Michele DE, Henry MD, Messing A, Cohn RD, Ross-Barta SE et al (2002) Deletion of brain dystroglycan recapitulates aspects of congenital muscular dystrophy. Nature 418(6896):422–425
Anderson JL, Head SI, Rae C, Morley JW (2002) Brain function in Duchenne muscular dystrophy. Brain 125:Pt 1
Li J, Jia Z, Xu W, Guo W, Zhang M, Bi J, Cao Y, Fan Z et al (2019) TGN-020 alleviates edema and inhibits astrocyte activation and glial scar formation after spinal cord compression injury in rats. Life Sci 222:148–157. https://doi.org/10.1016/j.lfs.2019.03.007
An S, Fu L (2018) Small-molecule PROTACs: An emerging and promising approach for the development of targeted therapy drugs. EBioMedicine 36:553–562. https://doi.org/10.1016/j.ebiom.2018.09.005
Toft-Bertelsen TL, Larsen BR, Christensen SK, Khandelia H, Waagepetersen HS, MacAulay N (2021) Clearance of activity-evoked K+ transients and associated glia cell swelling occur independently of AQP4: a study with an isoform-selective AQP4 inhibitor. Glia 69(1):28–41. https://doi.org/10.1002/glia.23851
Wu Y-J, Lin C-C, Yeh C-M, Chien M-E, Tsao M-C, Tseng P, Huang C-W, Hsu K-S (2017) Repeated transcranial direct current stimulation improves cognitive dysfunction and synaptic plasticity deficit in the prefrontal cortex of streptozotocin-induced diabetic rats. Brain Stimulation 10(6):1079–1087. https://doi.org/10.1016/j.brs.2017.08.007
Acknowledgements
We would like to acknowledge the support provided by Center for Brain Science (The First Affiliated Hospital of Xi’an Jiaotong University, Xi’an, Shaanxi, China) for assistance with experimental facilities.
Funding
This work was supported by programs from the Natural Science Foundation of China (No. 81771168) and Clinical research award of the First Affiliated Hospital of Xi’an Jiaotong University (XJTU1AF-CRF-2018–004).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Ye Yuan, Qiumin Qu, Jin Wang, and Yan Li designed the study; Ye Yuan, Wei Peng, and Jingna Lei performed the research; Ye Yuan, Wei Peng,Yi Zhao, and Beiyu Zhao analyzed data; Ye Yuan wrote the paper. All the authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
All experiments and procedures described in this study were performed in accordance with protocols approved by the Institutional Animal Care and Use Committee at Xi’an Jiaotong University (Xi’an, Shaanxi, China, No. 2019–060). Efforts were made to minimize animal suffering, and all sample sizes for the assessment parameters were calculated to minimize the number of animals used.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12035_2024_4085_MOESM1_ESM.pdf
Supplementary file1 (PDF 80541 KB) Fig. S1A. The purity of primary astrocytes. Representative immunofluorescence images of glial fibrillary acidic protein (GFAP) (green) and DAPI (blue) was showed. B Downregulation of AQP4 induced by high-glucose medium. Representative immunoblot bands and densitometric quantification of AQP4 in primary astrocytes cultured in high-glucose medium under 1 day, 3 days and 7 days (n = 3 independent experiments). Data is presented as mean ± SEM. *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001; ns, not significant. One-way ANOVA with Tukey’s multiple comparisons test was performed. Scale bars are indicated. Fig.S1C. Representative immunoblot bands and densitometric quantification of AQP4 in primary astrocytes pre-treated with 10umol/l Cycloheximide or DMSO for 6 hours (n = 3 independent experiments). One-way ANOVA with Tukey’s multiple comparisons test was performed. Supplementary Fig. S2 The transfection efficiency of lentivirus. Representative immunofluorescence images of green fluorescent protein (GFP) (green) and bright field image was showed. Supplementary Fig. S3 A: Representative IB bands and densitometric quantification of active-MMP-9 and 43-kDA β-DG in the hippocampus of db/db and wt mice (n=3 per group). B: Representative IB bands and densitometric quantification of active-MMP-9 and 30/43 kDA β-DG in the prefrontal cortex of db/db and wt mice (n=3 per group). C: Representative IB bands and densitometric quantification of MMP-2 (n=3 per group). D: Representative IB bands and densitometric quantification of β-DG in the prefrontal cortex of db/db and wt mice administrated with indicated medicine (n=6 per group). Data is presented as mean ± SEM. *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001; ns, not significant. Student’s t-test for (A, B) and One-way ANOVA with Tukey’s multiple comparisons test for (C, D)was performed. Scale bars are indicated
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yuan, Y., Peng, W., Lei, J. et al. AQP4 Endocytosis-Lysosome Degradation Mediated by MMP-9/β-DG Involved in Diabetes Cognitive Impairment. Mol Neurobiol (2024). https://doi.org/10.1007/s12035-024-04085-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12035-024-04085-9