Abstract
Background and Objective
Neuromuscular blocking agents are routinely used in laparoscopic surgery to optimize operative conditions. We compared the effect of a deep and moderate neuromuscular blockade (NMB) on surgical conditions and postoperative outcomes in children undergoing major laparoscopic surgery.
Methods
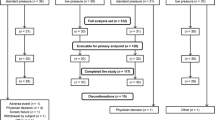
Sixty children aged 2–14 years scheduled to undergo major laparoscopic surgery were randomly allocated to deep (post-tetanic count 1–2 twitches) or moderate (train-of-four 1–2 twitches) NMB groups. The anesthesia was maintained with propofol and remifentanil, and the NMB was maintained with a rocuronium continuous infusion. At the end of the operation, the NMB were antagonized with sugammadex. The intra-abdominal pressure, airway pressure, Leiden Surgical Rating Scale, intraoperative hemodynamics, drug usages, duration of surgery, postoperative recovery time, pain, and complications were compared between the groups.
Results
The maximum and mean intra-abdominal pressure, the peak inspiratory pressure, and mean airway pressure were significantly lower in the deep NMB group than in the moderate NMB group (p < 0.001). The Leiden Surgical Rating Scale and the dosage of rocuronium were significantly higher in the deep NMB group than the moderate NMB group (p < 0.001). The intraoperative hemodynamics, duration of surgery, post-operative recovery time, pain, and the incidence rate of complications were not significantly different between the groups (p > 0.05).
Conclusions
A deep NMB provided better operative conditions and similar recovery profiles compared with a moderate NMB as reversed with sugammadex in children undergoing major laparoscopic surgery.
Clinical Trial Registration
Chinese Clinical Trial Registry, No. ChiCTR2100053821.



Similar content being viewed by others
References
Elhaddad A, Awad M, Shehata SM, Shehata MA. Laparoscopic management of infantile hydrocele in pediatric age group. Pediatr Surg Int. 2022;38(4):581–7.
Diao M, Li L, Kong C, et al. A novel combined enteroscopy and laparoscopy approach to prevent urethral complications in management of rectourethral fistula. Surg Endosc. 2021;35(4):1921–6.
Erol İ, Karamık K, İslamoğlu ME, Ateş M, Savaş M. Outcomes of infants undergoing laparoscopic pyeloplasty: a single-center experience. Urologia. 2019;86(1):27–31.
Martini CH, Boon M, Bevers RF, Aarts LP, Dahan A. Evaluation of surgical conditions during laporoscopic surgery in patients with moderate vs deep neuromuscular block. Br J Anaesth. 2014;112(3):498–505.
Koo BW, Oh AY, Seo KS, Han JW, Han HS, Yoon YS. Randomized clinical trial of moderate versus deep neuromuscular block for low-pressure pneumoperitoneum during laparoscopic cholecystectomy. World J Surg. 2016;40(12):2898–903.
Honing GHM, Martini CH, Olofsen E, et al. Deep neuromuscular block does not improve surgical conditions in patients receiving seveoflurane anaesthesia for laparoscopic renal surgery. Br J Anaesth. 2021;126(2):377–85.
Curry C, Steen K, Craig W, Cary CW, Richard J, Babikian G. Does deep neuromuscular blockade improve operating conditions during minimally invasive anterolateral total hip replacements? A randomized controlled trial. Cureus. 2020;12(9): e10328.
Sümpelmann R, Becke K, Zander R, Witt L. Perioperative fluid management in children: can we sum it all up now? Curr Opin Anaesthesiol. 2019;32(3):384–91.
Diao M, Li L, Li Q, Ye M, Cheng W. Single-incision versus conventional laparoscopic cyst excision and Roux-Y hepaticojejunostomy for children with choledochal cysts: a case-control study. World J Surg. 2013;37(7):1707–13.
Diao M, Li L, Cheng W. Single-incision laparoscopic repair for iatrogenic duodenal injury in children with choledochal cysts. J Laparoendosc Adv Surg Tech A. 2019;29(6):869–72.
Boon M, Martini CH, Aarts LPHJ, Dahan A. The use of surgical rating scales for the evaluation of surgical working conditions during laparoscopic surgery: a scoping review. Surg Endosc. 2019;33(1):19–25.
Boon M, Martini CH, Hellinga M, Bevers R, Aarts L, Dahan A. Influence of variations in arterial PCO2 on surgical conditions during laparoscopic retroperitoneal surgery. Br J Anaesth. 2016;117(1):59–65.
Manworren RC, Hynan LS. Clinical validation of FLACC: preverbal patient pain scale. Pediatr Nurs. 2003;29(2):140–6.
Nervil GG, Medici R, Thomsen JLD, et al. Validation of subjective rating scales for assessment of surgical workspace during laparoscopy. Acta Anaesthesiol Scand. 2017;61(10):1270–7.
Loh P, Yeong CH, Masohood NS, et al. Comparison of deep and moderate neuromuscular blockade in microwave ablation of liver tumors: a randomized-controlled clinical trial. Sci Rep. 2021;11(1):2299.
Wu L, Wei SW, Xiang Z, Yu EY, Qu SQ, Du Z. Effect of neuromuscular block on surgical conditions during short-duration paediatric laparoscopic surgery involving a supraglottic airway. Br J Anaesth. 2021;127(2):281–8.
Honing GHM, Martini CH, Olofsen E, et al. Deep neuromuscular block does not improve surgical conditions in patients receiving sevoflurane anaesthesia for laparoscopic renal surgery. Br J Anaesth. 2021;126(2):377–85.
Schukfeh N, Huber D, Metzelder ML, et al. Impact of capnoperitoneum on renal perfusion and urine production in infant and adolescent pigs: crystalloid versus colloid fluid resuscitation. Eur J Pediatr Surg. 2019;29(6):539–44.
Kuebler JF, Schukfeh N, Vieten G, et al. Arterioportal shunting, splanchnic capillary perfusion, and the effects of colloids during capnoperitoneum in neonatal and adolescent pigs. Surg Endosc. 2018;32(6):2923–31.
Caliskan E, Sanal Bas S, Onay M, et al. Evaluation of renal oxygenation in laparoscopic pediatric surgery by near infrared spectroscopy. Pediatr Surg Int. 2020;36(9):1077–86.
Silveira LGT, Brocca IC, Moraes ES, Brandão MB, Nogueira RJN, de Souza TH. Hemodynamic effects of increased intra-abdominal pressure in critically ill children. J Pediatr (Rio J). 2021;97(5):564–70.
Reijnders-Boerboom GTJA, Albers KI, Jacobs LMC, et al. Low intra-abdominal pressure in laparoscopic surgery: a systematic review and meta-analysis. Int J Surg. 2023;109(5):1400–11.
Voss T, Wang A, DeAngelis M, et al. Sugammadex for reversal of neuromuscular blockade in pediatric patients: results from a phase IV randomized study. Paediatr Anaesth. 2022;32(3):436–45.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
This research was funded by The Wu Jie-Ping Medical Foundation (project number: 320.6750.2021-05-4).
Conflict of interest
Guo Wei, Yong-Xin Li, Ying Chen, Mei Diao, John Wei Zhong, and Shou-Dong Pan have no conflicts of interest that are directly relevant to the content of this article.
Ethics approval
The protocol was approved by the Research Ethics Committee of Capital Institute of Pediatrics, Beijing, China (No. SHERLL2020060). The study was conducted in accordance with all applicable laws, rules, and regulations and with the Declaration of Helsinki and the International Council for Harmonisation guidelines for Good Clinical Practice.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Author contributions
GW: literature review; data curation; methodology; analysis and interpretation of the data; writing - original draft. Y-XL and MD: data curation; analysis and interpretation of the data. YC: literature review; analysis and interpretation of the data. JWZ and S-DP: design of the study; final approval of the version to be published. All authors read and approved the final version of the manuscript.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wei, G., Li, YX., Chen, Y. et al. Comparison of Deep and Moderate Neuromuscular Blockade for Major Laparoscopic Surgery in Children: A Randomized Controlled Trial. Pediatr Drugs (2024). https://doi.org/10.1007/s40272-024-00622-0
Accepted:
Published:
DOI: https://doi.org/10.1007/s40272-024-00622-0