Abstract
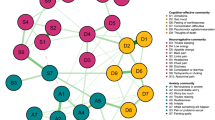
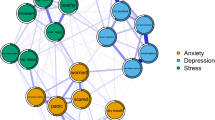
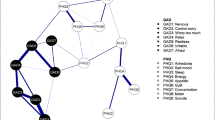
Medical graduate students are known to be susceptible to depression and anxiety, and coping style has been implicated in these pathogenic processes. However, the fine-grained pathways through which positive and negative coping styles (i.e., PCS and NCS) impact depression and anxiety remain unclear. This study aimed to use network analysis to investigate the associations among PCS/NCS, the individual symptoms of depression and anxiety, and their comorbidity among medical graduate students. Three regularized partial correlation networks were estimated based on cross-sectional data from 1582 medical graduate students, including PCS/NCS-depression, PCS/NCS-anxiety, and PCS/NCS-comorbidity networks. Bridge expected influence (BEI) values were calculated for each node within the three networks. The results showed the prevalence rates of mild or more severe depression and anxiety symptoms were 24.21% and 19.91%, respectively, in our sample. PCS and NCS functioned differently in relation to individual symptoms of depression and anxiety. Consistently, PCS had the highest negative BEI, while NCS had the highest positive BEI in the PCS/NCS-depression, PCS/NCS-anxiety, and PCS/NCS-comorbidity networks. PCS had more associations with depression and anxiety symptoms than did NCS. These findings shed light on the distinct pathways through which PCS and NCS may influence depression and anxiety. PCS and NCS were identified as important bridge nodes and transdiagnostic factors within separate depression and anxiety disorders and the comorbidity form, serving as protective and detrimental factors, respectively. Furthermore, PCS was more important than NCS in connecting the symptoms of depression and anxiety. Theoretical and clinical implications are discussed.




Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Almojali, A. I., Almalki, S. A., Alothman, A. S., Masuadi, E. M., & Alaqeel, M. K. (2017). The prevalence and association of stress with sleep quality among medical students. J Epidemiol Glob Health, 7(3), 169–174. https://doi.org/10.1016/j.jegh.2017.04.005.
Bai, W., Xi, H. T., Zhu, Q., Ji, M., Zhang, H., Yang, B. X., & Xiang, Y. T. (2021). Network analysis of anxiety and depressive symptoms among nursing students during the COVID-19 pandemic. Journal of Affective Disorders, 294, 753–760. https://doi.org/10.1016/j.jad.2021.07.072.
Barbosa-Camacho, F. J., Romero-Limon, O. M., Ibarrola-Pena, J. C., Almanza-Mena, Y. L., Pintor-Belmontes, K. J., Sanchez-Lopez, V. A., & Gonzalez-Ojeda, A. (2022). Depression, anxiety, and academic performance in COVID-19: A cross-sectional study. BMC Psychiatry, 22(1). https://doi.org/10.1186/s12888-022-04062-3.
Borsboom, D. (2017). A network theory of mental disorders. World Psychiatry, 16(1), 5–13. https://doi.org/10.1002/wps.20375.
Borsboom, D., & Cramer, A. O. J. (2013). Network Analysis: An Integrative Approach to the Structure of Psychopathology. In S. NolenHoeksema (Ed.), Annual Review of Clinical Psychology, Vol 9 (Vol. 9, pp. 91–121). https://doi.org/10.1146/annurev-clinpsy-050212-185608.
Chen, J., & Chen, Z. (2008). Extended bayesian information Criteria for Model Selection with large model spaces. BIOMETRIKA, 95(3), 759–771. https://doi.org/10.1093/biomet/asn034.
Chen, R., Fang, P., Tan, L., Li, J., & Yu, L. (2022). Factors associated with sleep quality among nurse managers during regular prevention and control of the COVID-19 in China: A cross-sectional study. BMC Nursing, 21(1). https://doi.org/10.1186/s12912-022-01149-w.
Classen, C., Koopman, C., Angell, K., & Spiegel, D. (1996). Coping styles associated with psychological adjustment to advanced breast cancer. Health Psychology, 15(6), 434–437. https://doi.org/10.1037//0278-6133.15.6.434.
Doering, L. V., Dracup, K., Caldwell, M. A., Moser, D. K., Erickson, V. S., Fonarow,G., & Hamilton, M. (2004). Is coping style linked to emotional states in heart failure patients? Journal of Cardiac Failure,10(4), 344–349. https://doi.org/10.1016/j.cardfail.2003.10.001.
Du, X., Wu, Y., & Shen, J. (2013). The impact of burden, positive feelings, coping style and social support on caregivers’ fatigue of dementia patients. Chinese Journal of Behavioral Medicine and Brain Science, 22(7), 611–613. https://pesquisa.bvsalud.org/portal/resource/pt/wpr-437410.
Epskamp, S., & Fried, E. (2018). A tutorial on regularized partial correlation networks. Psychological Methods, 23(4), 617–634. https://doi.org/10.1037/met0000167.
Epskamp, S., Cramer, A., Waldorp, L. J., Schmittmann, V. D., & Borsboom, D. (2012). Qgraph: Network visualizations of relationships in Psychometric Data. Journal of Statistical Software, 48(4), 367–371. https://doi.org/10.18637/jss.v048.i04.
Epskamp, S., Borsboom, D., & Fried, E. I. (2018). Estimating psychological networks and their accuracy: A tutorial paper. Behavior Research Methods, 50(1), 195–212. https://doi.org/10.3758/s13428-017-0862-1.
Everaert, J., & Joormann, J. (2019). Emotion regulation difficulties related to depression and anxiety: A Network Approach to Model relations among symptoms, positive reappraisal, and repetitive negative thinking. Clinical Psychological Science, 7(6), 1304–1318. https://doi.org/10.1177/2167702619859342. Article 2167702619859342.
Fisher, A. J., Bosley, H. G., Fernandez, K. C., Reeves, J. W., Soyster, P. D., Diamond, A. E., & Barkin, J. (2019). Open trial of a personalized modular treatment for mood and anxiety. Behaviour Research and Therapy, 116, 69–79. https://doi.org/10.1016/j.brat.2019.01.010.
Fried, E. I. (2015). Problematic assumptions have slowed down depression research: Why symptoms, not syndromes are the way forward. Frontiers in Psychology, 6, 309. https://doi.org/10.3389/fpsyg.2015.00309.
Fried, E. I., & Nesse, R. M. (2015). Depression sum-scores don’t add up: why analyzing specific depression symptoms is essential. BMC Medicine, 13. https://doi.org/10.1186/s12916-015-0325-4.
Guo, F., Yi, M., Sun, L., Luo, T., Han, R., Zheng, L., & Gao, C. (2021). A novel model to predict mental distress among medical graduate students in China. BMC Psychiatry, 21(1). https://doi.org/10.1186/s12888-021-03573-9.
Guo, Z., Cui, Y., Yang, T., Liu, X., Lu, H., Zhang, Y., & Zhu, X. (2023). Network analysis of affect, emotion regulation, psychological capital, and resilience among Chinese males during the late stage of the COVID-19 pandemic. Frontiers in Public Health, 11, 1144420. https://doi.org/10.3389/fpubh.2023.1144420.
Hoffart, A., Johnson, S. U., & Ebrahimi, O. V. (2022). Metacognitive beliefs, maladaptive coping strategies, and depressive symptoms: A two-wave network study of the COVID-19 lockdown and reopening. Journal of Psychiatric Research, 152, 70–78. https://doi.org/10.1016/j.jpsychires.2022.06.008.
Hope, V., & Henderson, M. (2014). Medical student depression, anxiety and distress outside North America: A systematic review. Medical Education, 48(10), 963–979. https://doi.org/10.1111/medu.12512.
Jin, Y., Sha, S., Tian, T., Wang, Q., Liang, S., Wang, Z., & Xiang, Y. T. (2022). Network analysis of comorbid depression and anxiety and their associations with quality of life among clinicians in public hospitals during the late stage of the COVID-19 pandemic in China. Journal of Affective Disorders, 314, 193–200. https://doi.org/10.1016/j.jad.2022.06.051.
Jones, P. J., Heeren, A., & McNally, R. J. (2017). Commentary: A network theory of mental disorders. Frontiers in Psychology, 8, 1305–1305. https://doi.org/10.3389/fpsyg.2017.01305.
Jones, P. J., Ma, R., & McNally, R. J. (2021). Bridge centrality: A Network Approach to understanding Comorbidity. Multivariate Behavioral Research, 56(2), 353–367. https://doi.org/10.1080/00273171.2019.1614898.
Kaiser, T., Herzog, P., Voderholzer, U., & Brakemeier, E. L. (2021). Unraveling the comorbidity of depression and anxiety in a large inpatient sample: Network analysis to examine bridge symptoms. Depression and Anxiety, 38(3), 307–317. https://doi.org/10.1002/da.23136.
Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x.
Li, L., Wang, Y., Wang, H., & Xu, M. (2010). Relationship between depression and trait coping style in middle school students of Chongqing. Acta Academiae Medicinae Militaris Tertiae, 32(10), 1071–1073. https://www.cabidigitallibrary.org/doi/full/10.5555/20113052650.
Li, Y., Cong, X., Chen, S., & Li, Y. (2021). Relationships of coping styles and psychological distress among patients with insomnia disorder. BMC Psychiatry, 21(1). https://doi.org/10.1186/s12888-021-03254-7.
Li, N., Fan, L., Wang, Y., Wang, J., & Huang, Y. (2022). Risk factors of psychological distress during the COVID-19 pandemic: The roles of coping style and emotional regulation. Journal of Affective Disorders, 299, 326–334. https://doi.org/10.1016/j.jad.2021.12.026.
Li, J., Wang, Q., Guan, C., Luo, L., & Hu, X. (2022a). Compassion fatigue and compassion satisfaction among Chinese palliative care nurses: A province-wide cross-sectional survey. Journal of Nursing Management, 30(7). https://doi.org/10.1111/jonm.13708.
Li, W., Chen, J., Li, M., Smith, A. P., & Fan, J. (2022c). The effect of exercise on academic fatigue and sleep quality among university students. Frontiers in Psychology, 13, 1025280–1025280. https://doi.org/10.3389/fpsyg.2022.1025280.
Liang, S., Liu, C., Rotaru, K., Li, K., Wei, X., Yuan, S., & Liu, X. (2022). The relations between emotion regulation, depression and anxiety among medical staff during the late stage of COVID-19 pandemic: A network analysis. Psychiatry Research, 317, 114863. https://doi.org/10.1016/j.psychres.2022.114863.
Liao, H., Tang, W., Huang, Y., Liu, M., Zhang, Y., Zhang, L., & Ai, T. (2020). Stressors, coping styles, and anxiety & depression in pediatric nurses with different lengths of service in six tertiary hospitals in Chengdu, China. Translational Pediatrics, 9(6), 827–834. https://doi.org/10.21037/tp-20-439.
McInerney, A. M., Lindekilde, N., Nouwen, A., Schmitz, N., & Deschenes, S. S. (2022). Diabetes distress, depressive symptoms, and anxiety symptoms in people with type 2 diabetes: A Network Analysis Approach to understanding comorbidity. Diabetes Care, 45(8), 1715–1723. https://doi.org/10.2337/figshare.19692721.
Meyer, J. D., Murray, T. A., Brower, C. S., Cruz-Maldonado, G. A., Perez, M. L., Ellingson, L. D., & Wade, N. G. (2022). Magnitude, timing and duration of mood state and cognitive effects of acute moderate exercise in major depressive disorder. Psychology of Sport and Exercise, 61, 102172. https://doi.org/10.1016/j.psychsport.2022.102172.
Morse, L., Paul, S. M., Cooper, B. A., Oppegaard, K., Shin, J., Calvo-Schimmel, A., & Miaskowski, C. (2023). Higher stress in Oncology patients is Associated with Cognitive and Evening physical fatigue severity. Journal of Pain and Symptom Management, 65(3), 203–215. https://doi.org/10.1016/j.jpainsymman.2022.11.017.
Mullarkey, M., Marchetti, I., & Beevers, C. (2019). Using Network Analysis to identify central symptoms of adolescent depression. Journal of Clinical Child and Adolescent Psychology: The Official Journal for the Society of Clinical Child and Adolescent Psychology American Psychological Association Division, 53(4), 656–668. https://doi.org/10.1080/15374416.2018.1437735.
Muller, L., & Spitz, E. (2003). Multidimensional assessment of coping: Validation of the brief COPE among French population. Encephale, 29(6), 507–518. (Evaluation multidimensionnelle du coping: validation du Brief COPE sur une population française.).
Nie, A., Su, X., Zhang, S., Guan, W., & Li, J. (2020). Psychological impact of COVID-19 outbreak on frontline nurses: A cross-sectional survey study. Journal of Clinical Nursing, 29(21–22), 4217–4226. https://doi.org/10.1111/jocn.15454.
Pang, Y., Fang, H., Li, L., Chen, M., Chen, Y., & Chen, M. (2021). Predictive factors of anxiety and depression among nurses fighting coronavirus disease 2019 in China. International Journal of Mental Health Nursing, 30(2), 524–532. https://doi.org/10.1111/inm.12817.
Peng, P., Chen, Q., Liang, M., Liu, Y., Chen, S., Wang, Y., & Liu, T. (2022). A network analysis of anxiety and depression symptoms among Chinese nurses in the late stage of the COVID-19 pandemic. Frontiers in Public Health, 10, 996386. https://doi.org/10.3389/fpubh.2022.996386.
Spitzer, R. L., Kroenke, K., Williams, J. B., & Löwe, B. (2006). A brief measure for assessing generalized anxiety disorder: The GAD-7. Archives of Internal Medicine, 166(10), 1092–1097. https://doi.org/10.1001/archinte.166.10.1092.
Tan, T., Liu, W., Zhao, Q., Hou, Y., Yang, Y., Wu, X., & Hu, G. (2023). Anxiety, depression, psychological stress and coping style in medical postgraduates in southeastern China when restricted to commuting between the campus and hospital during the COVID-19 pandemic. Frontiers in Psychiatry, 13, 1035075. https://doi.org/10.3389/fpsyt.2022.1035075.
Theberath, M., Bauer, D., Chen, W., Salinas, M., Mohabbat, A. B., Yang, J., & Wahner-Roedler, D. L. (2022). Effects of COVID-19 pandemic on mental health of children and adolescents: A systematic review of survey studies. SAGE Open Medicine, 10, 20503121221086712–20503121221086712. https://doi.org/10.1177/20503121221086712.
Thompson, G., McBride, R. B., Hosford, C. C., & Halaas, G. (2016). Resilience among medical students: The role of coping style and social support. Teaching and Learning in Medicine, 28(2), 174–182. https://doi.org/10.1080/10401334.2016.1146611.
Tibshirani, R. (1996). Regression Shrinkage and Selection via the Lasso. Journal of the Royal Statistical Society. Series B (Methodological).
Ukueberuwa, D. M., & Arnett, P. A. (2014). Evaluating the role of coping style as a moderator of fatigue and risk for future cognitive impairment in multiple sclerosis. Journal of the International Neuropsychological Society, 20(7), 751–755. https://doi.org/10.1017/s1355617714000587.
Wan, Y., Chen, R., Wang, S., Clifford, A., Zhang, S., Orton, S., & FangbiaoTao (2020). Associations of coping styles with nonsuicidal self-injury in adolescents: Do they vary with gender and adverse childhood experiences? Child Abuse & Neglect, 104, 104470–104470. https://doi.org/10.1016/j.chiabu.2020.104470.
Wang, D., Chen, J., Liu, X., Jin, Y., Ma, Y., Xiang, X., & Hou, X. (2022). Major impact of coping styles on anxiety and depression symptoms in Healthcare workers during the outbreak of COVID-19. Frontiers in Psychology, 13, 813295–813295. https://doi.org/10.3389/fpsyg.2022.813295.
Wu, H., Li, H., Li, X., Su, W., Tang, H., Yang, J., & Yang, L. (2022). Psychological Health and Sleep Quality of Medical graduates during the Second Wave of COVID-19 pandemic in post-epidemic era. Frontiers in Public Health, 10, 876298. https://doi.org/10.3389/fpubh.2022.876298.
Xiao, H., Shu, W., Li, M., Li, Z., Tao, F., Wu, X., & Hu, Y. (2020). Social Distancing among Medical students during the 2019 Coronavirus Disease Pandemic in China: Disease awareness, anxiety disorder, Depression, and behavioral activities. International Journal of Environmental Research and Public Health, 17(14). https://doi.org/10.3390/ijerph17145047.
Xie, Y. (1998). Reliability and validity of the simplified coping style questionnaire (Chinese). Chin J Clin Psychol, 6(2), 114–115.
Yin, M., Li, W., Yang, Q., Yue, Y., Fang, X., Yang, Z., & Du, X. (2022). The Mediating Role of coping style in the Relationship between Sleep Quality and Burnout: A cross-sectional study among Psychiatric nurses. Frontiers in Psychiatry, 13, 926040. https://doi.org/10.3389/fpsyt.2022.926040.
Yuan, L. L., Lu, L., Wang, X. H., Guo, X. X., Ren, H., Gao, Y. Q., & Pan, B. C. (2021). Prevalence and Predictors of Anxiety and Depressive Symptoms Among International Medical Students in China During COVID-19 Pandemic. Frontiers in Psychiatry, 12, Article 761964. https://doi.org/10.3389/fpsyt.2021.761964.
Yuan, L., Lu, L., Wang, X., Qu, M., Gao, Y., & Pan, B. (2023). Comorbid anxiety and depressive symptoms and the related factors among international medical students in China during COVID-19 pandemic: A cross-sectional study. BMC Psychiatry, 23(1), 165. https://doi.org/10.1186/s12888-023-04638-7.
Zeng, B., Zhao, J., Zou, L., Yang, X., Zhang, X., Wang, W., & Chen, J. (2018). Depressive symptoms, post-traumatic stress symptoms and suicide risk among graduate students: The mediating influence of emotional regulatory self-efficacy. Psychiatry Research, 264, 224–230. https://doi.org/10.1016/j.psychres.2018.03.022.
Zeng, W., Chen, R., Wang, X., Zhang, Q., & Deng, W. (2019). Prevalence of mental health problems among medical students in China: A meta-analysis. Medicine (Baltimore), 98(18), e15337. https://doi.org/10.1097/md.0000000000015337.
Zhang, Y., Cui, Y., Li, Y., Lu, H., Huang, H., Sui, J., & Miao, D. (2024). Network analysis of depressive and anxiety symptoms in older Chinese adults with diabetes mellitus. Frontiers in Psychiatry, 15, https://doi.org/10.3389/fpsyt.2024.1328857.
Zhu, J., Sun, L., Zhang, L., Wang, H., Fan, A., Yang, B., & Xiao, S. (2020). Prevalence and influencing factors of anxiety and depression symptoms in the First-Line Medical Staff fighting against COVID-19 in Gansu. Frontiers in Psychiatry, 11, 386. https://doi.org/10.3389/fpsyt.2020.00386.
Acknowledgements
The authors thank all the individuals who participated in the study and MogoEdit (https://www.mogoedit.com) for professional English language polishing.
Funding
The study was supported by the “Quick Response” Research Project of Air Force Medical University (2022KXKT014).
Author information
Authors and Affiliations
Contributions
Zhihua Guo: Conceptualization, Methodology, Writing - original draft. Yajuan Zhang: Methodology, Writing - original draft. Peiyun Pi: Formal analysis, Writing - original draft. Xia Zhu: Investigation, Formal analysis, Visualization. Yi Cui: Formal analysis, Visualization. Danmin Miao: Conceptualization, Supervision, Writing - Review & Editing. Hongliang Lu: Funding acquisition, Conceptualization, Investigation, Supervision, Writing - Review & Editing.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
All methods were carried out in accordance with the Declaration of Helsinki and with relevant guidelines and regulations. Informed consent was obtained from all participants included in this study. The ethical approval of the study was obtained from the Ethics Committee of the First Affiliated Hospital of the Air Force Medical University (No. KY20202063-F-2).
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Zhihua Guo, Yajuan Zhang and Peiyun Pi contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guo, Z., Zhang, Y., Pi, P. et al. Relations among coping style, and depression and anxiety symptoms in medical graduate students: a transdiagnostic network analysis. Curr Psychol (2024). https://doi.org/10.1007/s12144-024-05912-x
Accepted:
Published:
DOI: https://doi.org/10.1007/s12144-024-05912-x