Abstract
Background
Adenocarcinomas show a stepwise progression from atypical adenomatous hyperplasia (AAH) through adenocarcinoma in situ (AIS) to invasive adenocarcinoma (IA). Immunoglobulin superfamily containing leucine-rich repeat (ISLR) is a marker of tumor-restraining cancer-associated fibroblasts (CAFs), which are distinct from conventional, strongly α-smooth muscle actin (αSMA)-positive CAFs. Fibroblast activation protein (FAP) has been focused on as a potential therapeutic and diagnostic target of CAFs.
Methods
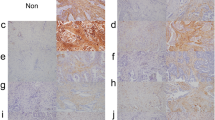
We investigated the changes in protein expression during adenocarcinoma progression in the pre-existing alveolar septa by assessing ISLR, αSMA, and FAP expression in normal lung, AAH, AIS, and IA. Fourteen AAH, seventeen AIS, and twenty IA lesions were identified and randomly sampled. Immunohistochemical analysis was performed to evaluate cancer-associated changes and FAP expression in the pre-existing alveolar structures.
Results
Normal alveolar septa expressed ISLR. The ISLR level in the alveolar septa decreased in AAH and AIS tissues when compared with that in normal lung tissue. The αSMA-positive area gradually increased from the adjacent lung tissue (13.3% ± 15%) to AIS (87.7% ± 14%), through AAH (70.2% ± 21%). Moreover, the FAP-positive area gradually increased from AAH (1.69% ± 1.4%) to IA (11.8% ± 7.1%), through AIS (6.11% ± 5.3%). Protein expression changes are a feature of CAFs in the pre-existing alveolar septa that begin in AAH. These changes gradually progressed from AAH to IA through AIS.
Conclusions
FAP-positive fibroblasts may contribute to tumor stroma formation in early-stage lung adenocarcinoma, and this could influence the development of therapeutic strategies targeting FAP-positive CAFs for disrupting extracellular matrix formation.




Similar content being viewed by others
Data availability
All relevant data are presented in the manuscript.
References
Succony L, Rassl DM, Barker AP et al (2021) Adenocarcinoma spectrum lesions of the lung: detection, pathology and treatment strategies. Cancer Treat Rev 99:102237
World Health Organization (2021). Thoracic tumours, WHO classification of Tumours, 5th Edition, Volume 5. International Agency for Research on Cancer
Noguchi M (2010) Stepwise progression of pulmonary adenocarcinoma-clinical and molecular implications. Cancer Metastasis Rev 29:15–21
Travis WD, Brambilla E, Noguchi M et al (2011) International association for the study of lung cancer/american thoracic society/european respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol 6:244–285
Kalluri R, Zeisberg M (2006) Fibroblasts in cancer. Nat Rev Cancer 6:392–401
Chen Y, McAndrews KM, Kalluri R (2021) Clinical and therapeutic relevance of cancer-associated fibroblasts. Nat Rev Clin Oncol 18:792–804
Maeda K, Enomoto A, Hara A et al (2016) Identification of Meflin as a potential marker for mesenchymal stromal cells. Sci Rep 6:22288
Kobayashi H, Gieniec KA, Wright JA (2021) The balance of stromal BMP signaling mediated by GREM1 and ISLR drives colorectal carcinogenesis. Gastroenterology 160:1224-1239.e30
Mizutani Y, Kobayashi H, Iida T et al (2019) Meflin-positive cancer-associated fibroblasts inhibit pancreatic carcinogenesis. Cancer Res 79:5367–5381
Miyai Y, Sugiyama D, Hase T et al (2022) Meflin-positive cancer-associated fibroblasts enhance tumor response to immune checkpoint blockade. Life Sci Alliance 5:e202101230
Augsten M (2014) Cancer-associated fibroblasts as another polarized cell type of the tumor microenvironment. Front Oncol 4:62
Avery D, Govindaraju P, Jacob M et al (2018) Extracellular matrix directs phenotypic heterogeneity of activated fibroblasts. Matrix Biol 67:90–106
Öhlund D, Handly-Santana A, Biffi G et al (2017) Distinct populations of inflammatory fibroblasts and myofibroblasts in pancreatic cancer. J Exp Med 214:579–596
Mathew S, Scanlan MJ, Mohan Raj BK et al (1995) The gene for fibroblast activation protein α (FAP), a putative cell surface-bound serine protease expressed in cancer stroma and wound healing, maps to chromosome band 2q23. Genomics 25:335–337
Kimura T, Monslow J, Klampatsa A et al (2019) Loss of cells expressing fibroblast activation protein has variable effects in models of TGF-β and chronic bleomycin-induced fibrosis. Am J Physiol Lung Cell Mol Physiol 317:L271–L282
Puré E, Blomberg R (2018) Pro-tumorigenic roles of fibroblast activation protein in cancer: back to the basics. Oncogene 37:4343–4357
Fitzgerald AA, Weiner LM (2020) The role of fibroblast activation protein in health and malignancy. Cancer Metastasis Rev 39:783–803
Moreno-Ruiz P, Corvigno S, te Grootenhuis NC et al (2021) Stromal FAP is an independent poor prognosis marker in non-small cell lung adenocarcinoma and associated with p53 mutation. Lung Cancer 155:10–19
Liao Y, Ni Y, He R et al (2013) Clinical implications of fibroblast activation protein-α in non-small cell lung cancer after curative resection: a new predictor for prognosis. J Cancer Res Clin Oncol 139:1523–1528
Min KW, Kim DH, Noh YK et al (2021) Cancer-associated fibroblasts are associated with poor prognosis in solid type of lung adenocarcinoma in a machine learning analysis. Sci Rep 11:16779
Pellinen T, Paavolainen L, Martín-Bernabé A et al (2023) Fibroblast subsets in non-small cell lung cancer: associations with survival, mutations, and immune features. J Natl Cancer Inst 115:71–82
Privé BM, Boussihmad MA, Timmermans B et al (2023) Fibroblast activation protein-targeted radionuclide therapy: background, opportunities, and challenges of first (pre)clinical studies. Eur J Nucl Med Mol Imaging 50:1906–1918
Windisch P, Zwahlen DR, Giesel FL et al (2021) Clinical results of fibroblast activation protein (FAP) specific PET for non-malignant indications: systematic review. EJNMMI Res 11:18
Giesel FL, Adeberg S, Syed M et al (2021) FAPI-74 PET/CT using either 18F-AlF or cold-kit 68Ga labeling: biodistribution, radiation dosimetry, and tumor delineation in lung cancer patients. J Nucl Med 62:201–207
Lo A, Wang LS, Scholler J et al (2015) Tumor-promoting desmoplasia is disrupted by depleting FAP-expressing stromal cells. Cancer Res 75:2800–2810
Wang LCS, Lo A, Scholler J et al (2014) Targeting fibroblast activation protein in tumor stroma with chimeric antigen receptor T cells can inhibit tumor growth and augment host immunity without severe toxicity. Cancer Immunol Res 2:154–166
Aghajanian H, Kimura T, Rurik JG et al (2019) Targeting cardiac fibrosis with engineered T cells. Nature 573:430–433
Kostrikov S, Johnsen KB, Braunstein TH et al (2021) Optical tissue clearing and machine learning can precisely characterize extravasation and blood vessel architecture in brain tumors. Commun Biol 4:815
Kanda Y (2013) Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant 48:452–458
Nurmik M, Ullmann P, Rodriguez F et al (2020) In search of definitions: cancer-associated fibroblasts and their markers. Int J Cancer 146:895–905
Sivakumar S, San Lucas FA, McDowell TL et al (2017) Genomic landscape of atypical adenomatous hyperplasia reveals divergent modes to lung adenocarcinoma. Cancer Res 77:6119–6130
Acharya PS, Zukas A, Chandan V et al (2006) Fibroblast activation protein: a serine protease expressed at the remodeling interface in idiopathic pulmonary fibrosis. Hum Pathol 37:352–360
Yotsukura M, Asamura H, Suzuki S et al (2020) Prognostic impact of cancer-associated active fibroblasts and invasive architectural patterns on early-stage lung adenocarcinoma. Lung Cancer 145:158–166
Lavie D, Ben-Shmuel A, Erez N et al (2022) Cancer-associated fibroblasts in the single-cell era. Nat Cancer 3:793–807
Fan MH, Zhu Q, Li HH et al (2016) Fibroblast activation protein (FAP) accelerates collagen degradation and clearance from lungs in mice. J Biol Chem 291:8070–8089
Zhang HE, Hamson EJ, Koczorowska MM et al (2019) Identification of novel natural substrates of fibroblast activation protein-alpha by differential degradomics and proteomics. Mol Cell Proteomics 18:65–85
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
This research was supported by JSPS KAKENHI [Grant number JP19K09314].
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Toru Kimura, Takashi Akazawa, Yu Mizote, Harumi Nakamura, Miki Sakaue, Tomohiro Maniwa, Yasushi Shintani, Keiichiro Honma, Hideaki Tahara, and Jiro Okami carried out material preparation, and data collection and analysis. Toru Kimura wrote the first draft of the manuscript, and all authors commented on previous versions. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no competing interest exists.
Ethics approval and consent to participate
This study was performed in line with the principles of the Declaration of Helsinki. The study was approved by the Institutional Review Board of the Osaka International Cancer Institute (June 12, 2019. Approval No. 19050). Written informed consent was obtained from all patients.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Kimura, T., Akazawa, T., Mizote, Y. et al. Progressive changes in the protein expression profile of alveolar septa in early-stage lung adenocarcinoma. Int J Clin Oncol (2024). https://doi.org/10.1007/s10147-024-02507-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10147-024-02507-1